Relationship anxiety triggers are specific situations that activate the attachment behavioral system's threat response — shifting your nervous system into fight-or-flight before your conscious mind catches up. According to Thriveworks research, 34 percent of Americans identify romantic relationships as their leading cause of mental health concerns. These triggers are distinct from root causes: triggers are what activates anxiety now, while root causes are the early attachment experiences that shaped how your nervous system responds.
Most articles list generic triggers, but the same situation — a partner not texting back — produces panic in one person and complete indifference in another. The difference is your attachment style. Your early experiences with caregivers wired your nervous system to scan for specific types of threat, and those same scans run automatically in adult relationships. This article maps specific triggers to attachment patterns and explains the neuroscience of why certain moments hijack your body before your mind catches up.
Key takeaway: Relationship anxiety triggers are situations that activate your attachment system's threat detector, including delayed texts, conflict, emotional distance, social media activity, and life transitions. Different attachment styles have different trigger profiles. Understanding your specific triggers through attachment theory and neuroception allows you to interrupt the anxiety cascade before it controls your behavior.
Why Does Your Brain Treat Relationship Threats Like Survival Threats?
Your brain treats relationship threats like survival threats because the attachment behavioral system — the same system that kept you alive as an infant — runs your adult romantic relationships. When this system detects a threat to your bond, it activates proximity-seeking behavior with the same urgency as a physical danger signal (Mikulincer and Shaver, 2003). Hazan and Shaver (1987) demonstrated that romantic love functions as an attachment process mirroring infant-caregiver dynamics, which means your adult relationship fears are running on ancient survival software.
The mechanism behind this is neuroception — a term coined by Porges (2022) to describe your brain's subconscious detection of safety versus danger. Neuroception operates below conscious awareness, scanning faces, tones of voice, and body language for threat cues faster than your thinking mind can process them. When neuroception works well, it helps you accurately read social situations. When it becomes miscalibrated through early attachment disruption, ordinary moments — a partner's neutral expression, a brief silence during dinner — get flagged as danger.
What happens after that flag depends on your attachment style. Anxiously attached individuals respond with hyperactivation — an intensified, chronic search for reassurance and closeness that escalates rather than resolves (Mikulincer and Shaver, 2003). Avoidantly attached individuals respond with deactivation — suppressing attachment needs and pulling away. Both are protective strategies your nervous system learned early. Neither is a character flaw.
The Neuroception Check-In (for all insecure attachment styles)
- Pause and notice where in your body you first feel relationship distress — chest, stomach, throat, jaw
- Name whether the sensation signals danger (something bad is happening) or disconnection (I am losing contact with my person)
- Ask yourself: "Am I responding to what is happening right now, or to what happened before?"
- Place one hand on the area of distress and take three slow breaths
This builds interoceptive awareness — the capacity to distinguish present-moment signals from pattern-matched threat memories stored in implicit memory. For anxiously attached individuals, this interrupts the hyperactivation cycle at its earliest point. For avoidantly attached individuals, it creates a moment of contact with feelings that typically get suppressed before they reach awareness.
What Are the Most Common Relationship Anxiety Triggers?
The most common relationship anxiety triggers are situations that signal potential rejection, abandonment, or loss of connection — and research has identified eight specific categories. Simpson and Rholes (2017) found that anxious attachment features are not constant but are evoked by specific stressful situations that threaten relationship stability or quality.
-
Inconsistent communication — Delayed text responses, sudden changes in messaging frequency, or shifts in tone activate a finely tuned radar for partner emotional availability (Levine and Heller, 2010). Your attachment system reads these gaps as potential abandonment signals.
-
A significant relationship conflict does not need to be dramatic to trigger disproportionate distress. Major conflict discussions activate reactive behavior in anxiously attached individuals not because of the disagreement itself, but because of what it seems to mean about the relationship's stability (Simpson and Rholes, 2017).
-
You know the feeling — your partner is across the room but somehow unreachable. Partner emotional unavailability through withdrawal, distraction, flat affect, or emotional shutdown sends a signal that your attachment figure is gone even when they are physically present (Levine and Heller, 2010).
-
Simpson and Rholes (2017) found that anxious partners can accurately detect relationship-threatening thoughts in their partner's mind. Attractive alternatives and romantic rivals activate this threat monitoring — the radar is sensitive and sometimes uncomfortably accurate.
-
Separation or abandonment cues — Business travel, time apart, even temporary goodbyes produce what Simpson and Rholes (2017) describe as "particularly strong negative emotional reactions" in anxiously attached individuals.
-
A 2025 longitudinal study confirmed that social media jealousy mediates the link between attachment anxiety and relationship dissatisfaction. Ambiguous online activity — a partner liking someone's photo, visible activity without responding to your message — provides endless material for an anxious attachment system to interpret.
-
Phubbing — Being ignored in favor of a phone creates social exclusion feelings that directly activate the attachment system (Journal of Consumer Research). Your partner is physically present but emotionally absent — one of the most confusing signals for an anxious nervous system.
-
Moving in together, getting engaged, or reaching any milestone that raises vulnerability stakes can paradoxically trigger anxiety. Life transitions and increased closeness remind your nervous system that greater closeness means greater potential loss.
The Trigger Inventory (for anxious attachment)
- Write down the last three times you felt a spike of relationship anxiety
- For each, answer: What happened externally? What story did your mind create? What did you do next?
- Look for patterns across all three instances — similar external cues, similar internal narratives, similar behavioral responses
- Circle any triggers that connect to childhood experiences of caregiver unavailability
Anxious attachment drives hypervigilance to availability cues. Mapping your triggers reveals which specific cues your attachment system has learned to flag as threats — often based on early caregiver inconsistency rather than current partner behavior. This exercise moves your trigger patterns from automatic reaction into conscious awareness, which is the first step toward choosing a different response.
How Do Different Attachment Styles Experience Different Triggers?
Different attachment styles experience different triggers because each style developed as an adaptation to a specific caregiving environment — and those adaptations created distinct trigger profiles that persist into adult relationships. What activates panic in one person may barely register for another, and the same external event produces radically different internal responses depending on your attachment wiring.
Anxious Attachment Triggers
Picture this: your partner mentioned they would call after work, and now it is two hours past that time. Your stomach drops. You check your phone again. You draft a text, delete it, draft another. This is what hypervigilance to availability cues looks like in practice. Silence, delayed responses, emotional distance, a partner socializing without you, and any ambiguous situation where connection feels uncertain will activate your system. Simpson and Rholes (2017) confirmed that anxious features emerge specifically in situations threatening relationship stability. If you recognize these patterns, your nervous system likely learned early that caregivers were inconsistently available — so you developed a sensitive alarm for any hint of withdrawal.
Avoidant Attachment Triggers
Research on deactivating strategies reveals a trigger profile that mirrors anxious attachment almost exactly — but in reverse. Where anxious attachment fears abandonment, avoidant attachment fears engulfment. Pressure for closeness, emotional demands, "where is this going?" conversations, loss of autonomy, and partner distress all activate suppression and withdrawal. The nervous system learned that self-reliance was safer than depending on others, so closeness itself becomes the threat signal.
Disorganized and Fearful-Avoidant Triggers
The body tells the story most clearly here: a tightness in the chest pulling you toward your partner while your legs feel ready to run. Both closeness and distance trigger anxiety simultaneously — creating a simultaneous approach-avoidance response that can feel like an internal war (Mikulincer and Shaver, 2003). Intimacy feels dangerous, but so does separation. Disorganized attachment develops when the attachment figure was both the source of comfort and the source of fear, leaving the nervous system with no coherent strategy. The unpredictability of your own reactions compounds the distress.
Secure Attachment Triggers
Securely attached individuals get triggered too — by genuine relationship threats like infidelity, betrayal, or sustained contempt. The difference is their window of tolerance is wider, their recovery is faster, and their responses tend to be proportional to the actual threat rather than amplified by pattern-matched memories.
| Trigger Category | Anxious Response | Avoidant Response | Disorganized Response |
|---|---|---|---|
| Partner silence | Panic, repeated texting, reassurance-seeking | Relief, enjoys the space | Panic then withdrawal, or cycling between both |
| Conflict | Escalation to restore connection | Shutdown, emotional retreat | Flooding, dissociation, or explosive reactivity |
| Increased closeness | Initial relief, then fear of losing it | Suffocation, pulling away | Craving it and fearing it simultaneously |
| Social media activity | Monitoring, interpreting, spiraling | Dismissing it as unimportant | Hypervigilance alternating with forced detachment |
| Life transitions | Anxiety about partner's commitment level | Anxiety about loss of independence | Wanting the milestone and sabotaging it |
| Partner distress | Merging with their emotions, over-functioning | Discomfort, withdrawing, minimizing | Wanting to help but feeling overwhelmed and freezing |
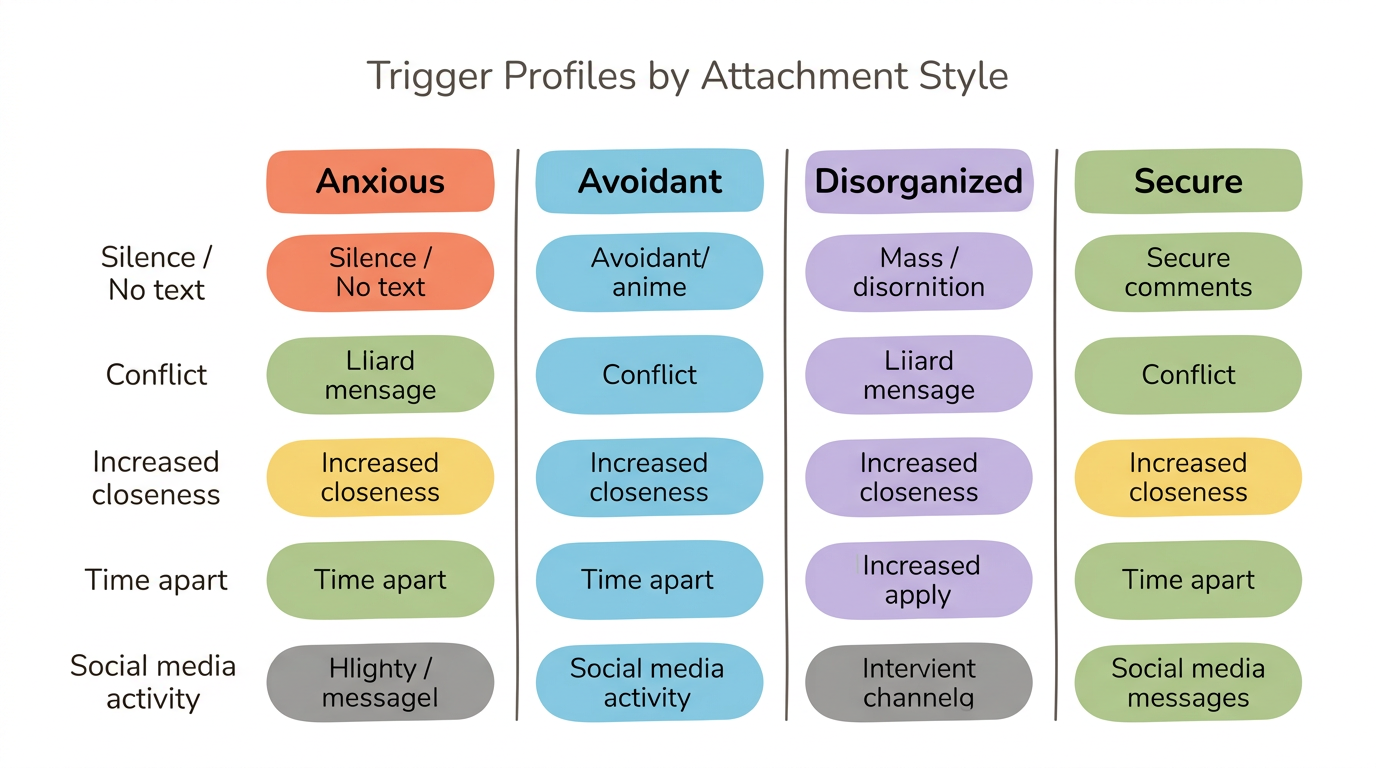
The Attachment Trigger Map (for all insecure attachment styles)
- Draw two columns on a piece of paper
- In the left column, list these ten common triggers: partner silence, conflict, compliments, increased closeness, time apart, social media activity, meeting their friends, discussing the future, partner crying, sexual intimacy
- In the right column, rate each trigger from zero to five for intensity of your reaction
- Color-code each trigger: blue for triggers involving too much distance (anxious pattern), red for triggers involving too much closeness (avoidant pattern), purple for triggers that feel like both simultaneously (disorganized pattern)
- Notice which color dominates your map
This exercise works because it externalizes implicit attachment reactions into a visible pattern — moving threat detection from automatic neuroception into conscious awareness where it can be examined rather than obeyed. Many people discover they have a primary color with secondary patterns, reflecting the complexity of real attachment rather than neat categories.
What Happens in Your Brain and Body When a Trigger Fires?
When a relationship trigger fires, a neurobiological cascade unfolds in milliseconds — your amygdala, stress hormones, and autonomic nervous system respond before your prefrontal cortex even registers what happened. Understanding this cascade explains why you cannot think your way out of a triggered state and why body-based approaches are essential.
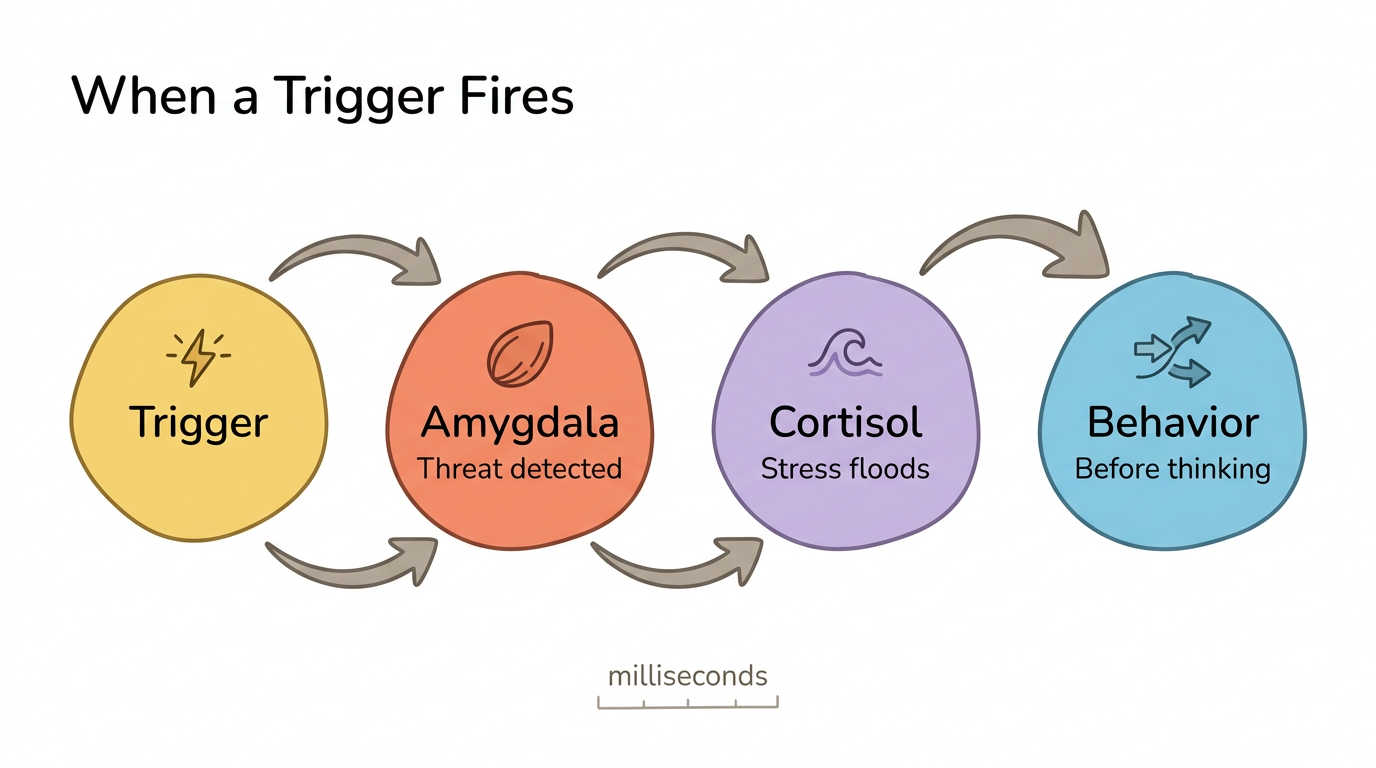
Amygdala hyperreactivity is the starting point. Vrtička and colleagues (2008) found that attachment anxiety correlates with an overactive amygdala response, especially to angry faces and social punishment cues. Your threat detection center is calibrated to high sensitivity — it fires faster and louder than in securely attached individuals, flagging ambiguous social cues as dangerous.
That amygdala signal cascades into heightened activity in the posterior cingulate cortex, which Zhang and colleagues (2021) linked to intensified scanning for separation and threat information. Your brain literally dedicates more processing power to looking for evidence that something is wrong. This is not overthinking — it is your neurology operating as designed, based on what it learned was necessary for survival.
Cortisol dysregulation follows. Powers and colleagues (2006) found that anxious attachment correlates with elevated and flat cortisol profiles — a chronic stress signature rather than the healthy rise-and-fall rhythm of a regulated nervous system. Your stress response is not spiking and recovering. It is running at a constant low-grade hum that makes every new trigger land on an already-activated system.
Perhaps the most counterintuitive finding is the oxytocin paradox. Schneiderman and colleagues (2012) demonstrated that oxytocin — the bonding hormone — is higher in new lovers compared to singles, but it correlates with both interactive reciprocity and relationship worries. The same neurochemical that creates closeness also amplifies threat-monitoring in anxiously attached people. This is why anxiety can intensify when your relationship is going well — more bonding means more oxytocin means more vigilance.
Research by Diamond and colleagues confirmed that partner separation physiology is real and measurable — cortisol changes, disrupted sleep, altered affect, and physical symptoms during partner absence. These effects are more pronounced in those with high attachment anxiety. Your body is not making this up.
For a deeper understanding of how your attachment style shapes your nervous system, the neuroscience points toward one clear conclusion: triggered states are biological events, not personal failures.
The Pendulation Practice (for anxious and disorganized attachment — somatic technique)
- When you notice a trigger has fired, pause wherever you are
- Notice where distress lives in your body — tightness, heat, pressure, heaviness. Stay with it for approximately ten seconds without trying to change it
- Now find one place in your body that feels neutral or calm — feet on the floor, hands in your lap, back against the chair
- Slowly move your attention back and forth between the distressed area and the calm area, spending approximately ten seconds in each location
- Complete five rounds of this back-and-forth movement of attention
This technique is drawn from Somatic IFS (McConnell and Schwartz) and works because anxious and disorganized attachment patterns collapse the nervous system into a single overwhelming state. Pendulation teaches the nervous system that distress and safety can coexist — building the capacity to tolerate triggered feelings without being consumed by them. Over time, this expands your window of tolerance, meaning the same trigger produces a smaller wave.
When Is Relationship Anxiety Actually ROCD?
Relationship anxiety crosses into ROCD (Relationship OCD) when intrusive doubts about your relationship become ego-dystonic — meaning they feel foreign, unwanted, and distressing rather than like genuine concerns you are choosing to think about. Doron and colleagues (2016) found an effect size of d=1.55 for relationship obsessions comparing ROCD to controls, confirming that ROCD represents a distinct clinical pattern rather than ordinary worry.
The spectrum runs from normal relationship worries (occasional, proportional, resolvable through reflection) through attachment-driven anxiety (frequent, disproportionate, temporarily relieved by reassurance) to clinical ROCD (intrusive, ego-dystonic, worsened by compulsive reassurance-seeking). Most people with attachment anxiety sit somewhere in the middle of this spectrum, but recognizing where you fall matters because the treatments differ.
Attachment-driven anxiety responds to felt security, co-regulation, and earned security work. ROCD responds to ERP (Exposure and Response Prevention) — learning to tolerate uncertainty about your relationship without performing compulsive behaviors to neutralize the doubt. Doron and colleagues (2016) also found that ROCD involves catastrophic beliefs about being in the "wrong" relationship (d=1.03 compared to OCD controls), suggesting that the anxiety targets relationship identity at a deep level.
ROCD and attachment anxiety can co-occur and amplify each other. An anxiously attached person may develop ROCD-like patterns where reassurance-seeking becomes compulsive — checking if it is anxiety or intuition fifty times a day rather than twice. If you are wondering whether your doubts mean you should leave the relationship, the pattern of the doubt matters more than its content.
The Thought Source Check (for anxious attachment and ROCD spectrum)
- When a relationship doubt appears, pause and ask: Does this thought feel like mine — something I chose to think about — or does it feel like an intrusion that arrived uninvited?
- Notice what happens when you engage with the thought: Does engaging bring relief and clarity, or does it generate more doubt and more questions?
- Ask: Am I seeking reassurance to feel better right now, or seeking information to make an actual decision?
- If the thought feels intrusive, engaging amplifies it, and reassurance provides only fleeting relief before the doubt returns — note that pattern without acting on it
This distinction matters because ROCD responds to ERP — learning to sit with uncertainty — while attachment-driven anxiety responds to felt security and co-regulation. Treating ROCD with reassurance makes it worse. Treating attachment anxiety with exposure alone misses the relational need underneath. Knowing which pattern you are in guides you toward the right support.
How Can You Interrupt a Trigger Before It Hijacks You?
You can interrupt a trigger by creating a gap between the moment your nervous system activates and the moment you act on that activation. Your nervous system learned these responses for good reason — they were adaptive strategies that kept you safe in an earlier environment. And now you can teach it something new. You do not rewire attachment in a single insight. You rewire it by noticing ten percent earlier, responding ten percent differently, ten percent more often.
If you have ever been in a triggered state, you know how overwhelming it can feel — the urgency to do something, to fix it, to reach out or pull away right now. That urgency is your nervous system doing its job, not evidence that something is actually wrong. The strategies below work not by fighting that urgency, but by giving your system a different option.
Security priming is one of the most researched interrupt strategies. Mikulincer and Shaver demonstrated across multiple studies that bringing to mind images of secure attachment figures reduces threat reactivity. Even imagining a safe person activates neural pathways associated with secure attachment, temporarily widening your window of tolerance. This is not wishful thinking — it is deliberate use of mental imagery to shift neurobiological state.
Co-regulation with a responsive partner provides the most powerful buffer against triggers. Simpson and Rholes (2017) found that partner commitment substantially diminishes anxious individuals' negative responses to triggers. Felt security — the lived experience of a partner who shows up consistently — does not eliminate triggers, but it changes what happens after one fires. If you are in a relationship where communicating your needs is possible, co-regulation can become a shared practice rather than a one-sided demand.
Cognitive restructuring helps you identify the catastrophic story your mind generates — "they did not text back, which means they are leaving me" — and build a more realistic appraisal of the situation. This is not about dismissing your feelings. It is about separating the signal from the noise so you can respond to what is actually happening.
An IFS-informed approach of naming the activated part — "a part of me feels scared right now" — rather than fusing with it ("I am terrified, this relationship is ending") creates distance between you and the reaction. That distance is where choice lives.
The Secure Base Visualization (for anxious attachment)
- Close your eyes and bring to mind someone who has been consistently safe for you — a therapist, grandparent, friend, teacher, or even a fictional character
- Recall a specific moment you felt safe with them — what they said, their tone of voice, their facial expression, how close they were
- Notice what shifts in your body as you hold this image — softening in the chest, slower breathing, release in the shoulders
- Anchor that shift with a physical gesture — hand on heart, fingers touching, or a gentle squeeze of your own wrist
- Practice this visualization daily for two weeks to strengthen the neural pathway, then use the physical anchor when triggered in real time
Security priming works because it activates the same neural pathways that a responsive caregiver would — temporarily providing the felt security that downregulates the amygdala and widens the window of tolerance. For anxiously attached individuals, this offers an internal resource for self-soothing that does not depend on your partner's immediate availability, which is precisely the dependency that keeps the hyperactivation cycle running.
When Should You Seek Professional Help for Relationship Anxiety Triggers?
You should seek professional help when your triggers dominate daily functioning, when anxiety persists regardless of your partner's behavior, or when self-help strategies have not produced noticeable change after three or more months of consistent practice. This is not a sign that something is wrong with you — it is a recognition that some nervous system patterns need the live, attuned presence of another person to shift.
Seeking help is especially worth considering if you notice these patterns: ROCD symptoms that worsen with reassurance, dissociative responses during triggered states, relationships keep ending in ways that feel connected to your trigger responses, or a partner who walks on eggshells to avoid activating you. The 18 to 29 age group shows the highest rates of both anxiety and depression symptoms (CDC, 2024) — if you are in that range, you are far from alone, and early intervention produces better outcomes.
Emotionally Focused Therapy works with couples to identify the negative interaction cycles driven by attachment fears — helping both partners access the vulnerable emotions underneath their surface reactions (Johnson, 2019). CBT is effective for individual cognitive restructuring and has been shown to help approximately 75 percent of couples in distress. Somatic therapies address body-held patterns that cognitive approaches alone cannot reach — particularly important for disorganized attachment, where triggers may bypass language entirely. If you are in an anxious-avoidant dynamic, couples therapy can address the cycle rather than just one partner's triggers.
The Readiness Reflection (for all attachment styles)
- Ask yourself: Have I been working on my triggers for three or more months with no noticeable shift?
- Does my partner modify their behavior to avoid triggering me — and does it still not feel like enough?
- Do I avoid situations — meeting friends, travel, conflict, intimacy — because of anticipated anxiety?
- If you answered yes to two or more of these questions, professional support can provide what self-work alone cannot
Therapy offers an attuned relationship that models secure responsiveness in real time, which is how the attachment system actually rewires. Earned security develops through repeated experiences of rupture and repair with a responsive other — and a skilled therapist provides exactly that.
Frequently Asked Questions
What triggers relationship anxiety the most?
Partner emotional unavailability and inconsistent communication are the most researched triggers. Simpson and Rholes (2017) found that major conflict and separation cues produce the strongest anxiety responses in insecurely attached individuals, especially when partner commitment feels uncertain.
Can relationship anxiety be triggered by a good relationship?
Yes — when closeness increases, insecurely attached individuals may feel more vulnerable, not less. The nervous system interprets unfamiliar safety as suspicious because early attachment experiences taught it that good things precede loss. Schneiderman and colleagues (2012) found that oxytocin amplifies both bonding and threat-monitoring, which explains why anxiety spikes when things are going well.
Do I have relationship anxiety or am I not in love?
Relationship anxiety produces intrusive doubt despite wanting the relationship, while genuine incompatibility typically brings clarity over time. If reassurance helps temporarily but doubt returns within hours, that cyclical pattern points to anxiety rather than authentic misalignment. The quality of the doubt matters more than its content when distinguishing anxiety from intuition.
What does relationship anxiety feel like in the body?
Common somatic markers include chest tightness, stomach dropping, throat constriction, racing heart, shallow breathing, and urgent restless energy. These sensations reflect attachment system activation — your nervous system shifting into fight-or-flight before your conscious mind registers the threat.
Can relationship anxiety ruin a good relationship?
Untreated relationship anxiety can create self-fulfilling prophecies — protest behaviors like excessive texting, jealousy accusations, or emotional withdrawal push partners away, confirming the original fear of abandonment. Simpson and Rholes (2017) found that partner commitment buffers against this cycle, suggesting that felt security from a responsive partner can moderate trigger reactivity. Relationship anxiety can shift with awareness and consistent practice.
How do I stop being triggered in my relationship?
Complete elimination of triggers is not realistic or necessary. The goal is expanding your window of tolerance so triggers produce manageable discomfort rather than overwhelm. Security priming, somatic regulation techniques like pendulation, and co-regulation with a responsive partner are the most evidence-based approaches. You do not need to never feel anxiety — you need to feel it without it running your behavior.
Is relationship anxiety a form of OCD?
Not always, but ROCD (Relationship OCD) is a recognized subtype involving intrusive, unwanted doubts about relationship rightness or partner adequacy. The key distinction is that ROCD thoughts feel ego-dystonic — foreign and distressing — while attachment-driven anxiety feels like a genuine warning. ROCD responds best to ERP therapy rather than reassurance.
Why does social media make my relationship anxiety worse?
Social media provides constant ambiguous cues for an anxious attachment system to interpret as threats — a partner liking someone's photo, online activity without responding to your message, or interaction with attractive others. Research confirms that social media jealousy and surveillance mediate the link between attachment anxiety and relationship dissatisfaction.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Foundational Attachment Works
- Hazan, C., & Shaver, P. (1987). Romantic love conceptualized as an attachment process. Journal of Personality and Social Psychology, 52(3), 511–524.
- Mikulincer, M., & Shaver, P. R. (2003). The attachment behavioral system in adulthood: Activation, psychodynamics, and interpersonal processes. Advances in Experimental Social Psychology, 35, 53–152.
- Levine, A., & Heller, R. (2010). Attached: The new science of adult attachment and how it can help you find — and keep — love. TarcherPerigee.
Research Studies
- Simpson, J. A., & Rholes, W. S. (2017). Adult attachment, stress, and romantic relationships. Current Opinion in Psychology, 13, 19–24.
- Vrtička, P., Andersson, F., Grandjean, D., Sander, D., & Vuilleumier, P. (2008). Individual attachment style modulates human amygdala and striatum activation during social appraisal. PLoS ONE, 3(8), e2868.
- Zhang, X., et al. (2021). Adult attachment anxiety and resting-state brain connectivity in the posterior cingulate cortex. BMC Neuroscience, 22, Article 17.
- Powers, S. I., Pietromonaco, P. R., Gunlicks, M., & Sayer, A. (2006). Dating couples' attachment styles and patterns of cortisol reactivity and recovery in response to a relationship conflict. Psychoneuroendocrinology, 31(4), 479–494.
- Schneiderman, I., Zagoory-Sharon, O., Leckman, J. F., & Feldman, R. (2012). Oxytocin during the initial stages of romantic attachment: Relations to couples' interactive reciprocity. Psychoneuroendocrinology, 37(8), 1277–1285.
- Diamond, L. M., Hicks, A. M., & Otter-Henderson, K. D. (2008). Every time you go away: Changes in affect, behavior, and physiology associated with travel-related separations from romantic partners. Personality and Social Psychology Bulletin, 34(4), 536–548.
- Doron, G., Derby, D. S., Szepsenwol, O., Nahaloni, E., & Moulding, R. (2016). Relationship obsessive-compulsive disorder: Interference, symptoms, and maladaptive beliefs. Frontiers in Psychiatry, 7, 58.
Neuroscience and Polyvagal Theory
- Porges, S. W. (2022). Polyvagal theory: A science of safety. Frontiers in Integrative Neuroscience, 16, 871227.
- McConnell, S., & Schwartz, R. C. Somatic Internal Family Systems Therapy. IFS Institute Publications.
Clinical and Applied Sources
- Johnson, S. M. (2019). The practice of emotionally focused couple therapy: Creating connection. Routledge.
- International OCD Foundation. (n.d.). Relationship OCD. IOCDF Expert Opinions.
Epidemiology
- National Institute of Mental Health. (n.d.). Any anxiety disorder. NIMH Statistics.
- Centers for Disease Control and Prevention. (2024). Symptoms of anxiety or depressive disorder among adults: United States, 2019–2022. NCHS Health Stats Report, No. 213.
- Thriveworks. (2023). Research: Widespread relationship anxiety. Thriveworks Research.
This article is for educational purposes only and is not a substitute for professional mental health advice, diagnosis, or treatment. If you are experiencing persistent relationship anxiety that interferes with daily functioning, please consult a licensed mental health professional.
