Self-soothing in the context of anxious attachment is the ability to calm your own nervous system without depending on another person's reassurance. Anxious attachment affects roughly 11 to 20 percent of adults (Hazan and Shaver, 1987; Diehl et al., 2015), and research shows these individuals use hyperactivating strategies that chronically intensify emotions rather than regulate them (Mikulincer and Shaver, 2019).
Here is the paradox you may recognize: for anxiously attached people, self-soothing can feel like abandoning the very strategy—connection-seeking—that kept you safe as a child. This article does not ask you to stop needing people. It gives you 10 research-backed techniques to calm your nervous system first, so you can connect from choice rather than panic. Six are "in the moment" crisis tools. Four are longer-term practices that build your capacity over time. If you are not sure whether anxious attachment applies to you, these 12 signs are a good starting point.
Key takeaway: Anxious attachment makes self-soothing difficult because your nervous system learned to seek external regulation through hyperactivating strategies. These ten evidence-based techniques, from vagal toning and security priming to self-compassion pauses and parts check-ins, work with your attachment wiring rather than against it to build an internal secure base over time.
Why Is Self-Soothing So Hard When You Have Anxious Attachment?
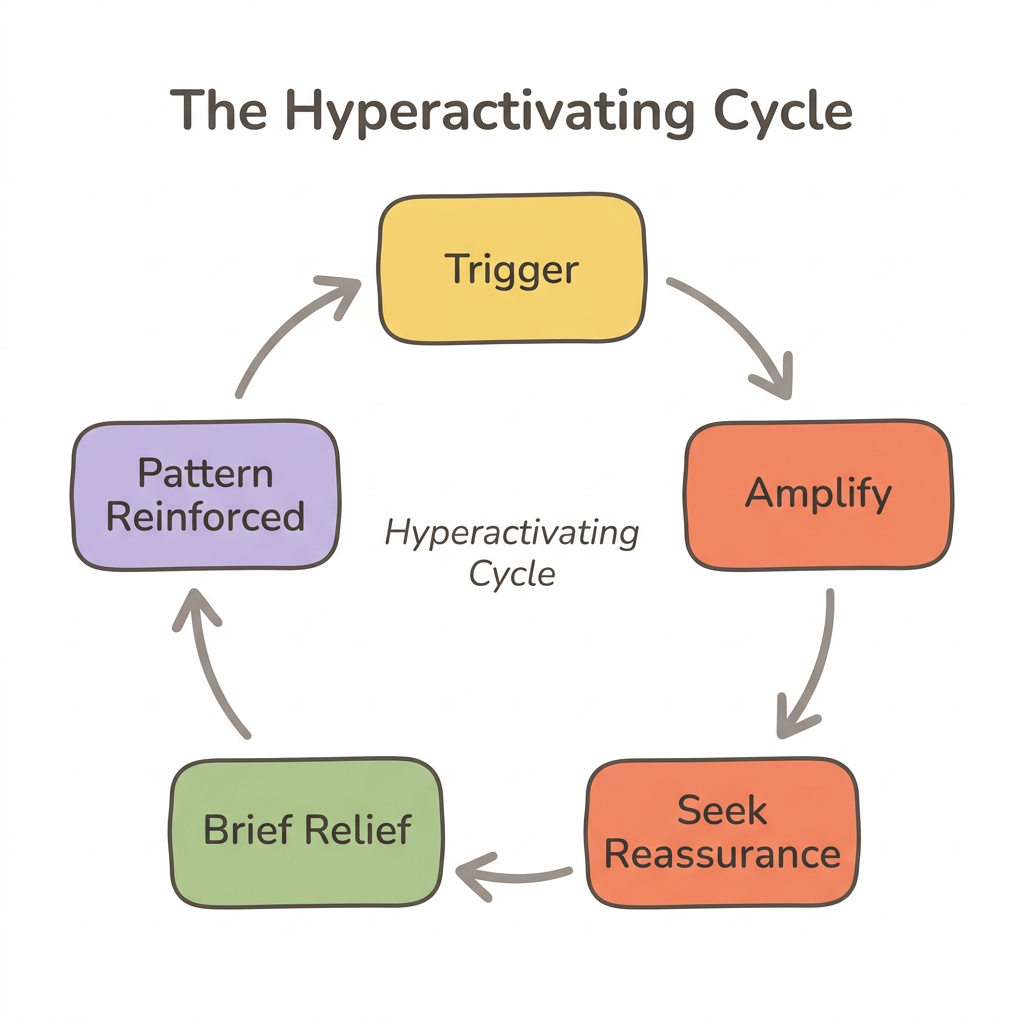
Self-soothing is hard for anxiously attached people because their nervous system learned the opposite skill: amplifying distress to get caregiving, not quieting it. Mikulincer and Shaver (2019) call these hyperactivating strategies—chronically intensifying emotions like jealousy, fear, and sadness to demand attention and care.
Your body is doing exactly what it was trained to do. When caregiving was inconsistent in childhood, louder emotional signals meant a better chance of getting your needs met. That adaptation made sense then. It just does not serve you now.
The neuroscience confirms this pattern. Anxious attachment correlates with increased amygdala reactivity to social threat—your brain's alarm system fires faster and louder than average (Vrtička et al., 2008). At the same time, the connection between your amygdala and prefrontal cortex—the brain region responsible for calming that alarm—is weaker (Moutsiana et al., 2019). Anxiously attached individuals also show specific impairment in impulse control when emotionally activated (Pascuzzo et al., 2023).
One critical finding: suppression does not work for this population. A systematic review found that anxiously attached individuals struggle with expressive suppression—the "just calm down" approach—but can successfully use cognitive reappraisal to reduce distress (Viddal et al., 2023). This means the techniques that work for anxious attachment are not about stuffing emotions down. They are about working with your nervous system.
The Activation Audit (for anxious attachment)
- Write down your last 3 attachment activations
- For each one, note: What triggered it? What did your body do? What did you reach for—your phone, reassurance, rumination?
- Name the hyperactivating pattern without judgment: "I notice I called three times, then spiraled into worst-case scenarios"
- Look for the common thread across all three
This works for anxious attachment because externalizing the pattern on paper interrupts automatic escalation. You cannot change a cycle you cannot see. Building this self-awareness is the first step toward choosing a different response.
What Is the Difference Between Self-Soothing and Co-Regulation?
Self-soothing is internal regulation—calming your nervous system on your own. Co-regulation is nervous system calming through attunement with another person—a warm voice, a steady presence, physical touch. Porges (2011) describes co-regulation as a function of the ventral vagal social engagement system: your nervous system literally borrows calm from someone else's.
Anxious attachment overrelies on co-regulation because that is what was intermittently available in childhood. Your nervous system learned that safety comes from outside, not inside. The goal is not to eliminate your need for co-regulation—that is avoidance, not security. The goal is to build flexible access to both.
Secure attachment means you can self-soothe when your partner is unavailable and reach for co-regulation when you need closeness. Healthy interdependence means having the capacity for both, and choosing between them based on the situation rather than compulsion (Mikulincer and Shaver, 2003). For a deeper look at how attachment shapes your nervous system responses, see how attachment style affects your nervous system.
One more distinction worth making: self-soothing is not the same as self-care. Self-soothing is in-the-moment nervous system regulation during emotional activation. Self-care is ongoing wellbeing practices—sleep, nutrition, boundaries. You need both, but they serve different functions.
How Do You Self-Soothe Anxious Attachment in the Moment?
The following six techniques are designed for acute activation—the minutes when you want to send the fifth text, call again, or spiral into worst-case scenarios. Each one takes five minutes or less.
Technique 1: Name the Activation Out Loud (Affect Labeling)
Your nervous system learned to feel first and think later—for good reason. When emotions flood in and your chest tightens, the simplest intervention is also the fastest: say what is happening out loud.
Saying "I'm feeling activated right now—this is my anxious attachment, not an emergency" reduces amygdala reactivity by engaging the prefrontal cortex. Neuroscience research on affect labeling shows that putting feelings into words literally dampens the brain's threat response (Lieberman et al., 2007). No tools required. No preparation. Just words.
The Three-Sentence Label (for anxious attachment)
- Say out loud: "I notice I'm feeling [emotion]"
- "My anxious attachment is telling me [the story or fear]"
- "What is actually happening right now is [facts only]"
Example: "I notice I'm feeling panicky. My anxious attachment is telling me he's losing interest because he hasn't texted in three hours. What is actually happening is that he said he had a busy afternoon at work."
Naming the emotion as an attachment response—rather than reality—creates cognitive distance from the hyperactivating story. The prefrontal cortex engages and downregulates the amygdala's alarm.
Technique 2: Extended Exhale Breathing (Vagal Toning)
A four-count inhale followed by a six-count exhale activates the vagus nerve's parasympathetic brake, shifting your nervous system from sympathetic overdrive toward a calm-and-connected state (Porges, 2011). Anxious attachment correlates with reduced ventral vagal access—your nervous system gets stuck in fight-or-flight. The extended exhale mechanically reverses this.
That tightness in your chest, the racing heart, the urge to do something right now—your body is trying to protect you. It learned that stillness was dangerous. And you can gently teach it otherwise, one breath at a time.
The 4-6 Reset (for anxious attachment)
The extended exhale works for anxious attachment because it mechanically stimulates the vagus nerve to shift from sympathetic activation—the urgency to reach out, to fix, to know—toward ventral vagal engagement, the state where you feel calm enough to choose your next move.
- Place one hand on your chest and one on your belly
- Inhale through your nose for 4 counts
- Exhale slowly through your mouth for 6 counts
- Aim for your belly hand to move more than your chest hand
- Repeat for 6 cycles—about 1 minute total
- Notice the shift in your body before you take any action
Technique 3: TIPP — Cold Water Dive Reflex
The mammalian dive reflex is the fastest physiological reset available without medication. When cold water contacts your face—particularly the forehead and area around the eyes—your heart rate drops within seconds. This is a DBT distress tolerance technique designed for moments when cognitive strategies cannot break through the activation.
Sometimes activation hits so hard that breathing exercises feel impossible—hands shaking, thoughts racing too fast to name. That is exactly when this technique earns its place.
The 30-Second Reset (for anxious attachment)
- Fill a bowl with cold water and ice (or grab a bag of frozen peas)
- Hold your breath and submerge your face for 15 to 30 seconds (or press the frozen peas to your forehead and eye area)
- Notice the immediate shift—your heart rate will drop
- Follow with 3 rounds of 4-6 breathing from Technique 2
- Then reassess: do you still need to send that message, or was it the activation talking?
This works for anxious attachment because during acute activation, cortisol and adrenaline flood your body, making cognitive strategies nearly impossible. The dive reflex bypasses the thinking brain entirely and forces a parasympathetic shift—giving you a window to choose a different response.
Technique 4: 5-4-3-2-1 Sensory Grounding
Sensory grounding interrupts rumination by forcing attention into the present moment and engaging the prefrontal cortex. Rumination—replaying conversations, analyzing tone, catastrophizing silence—is the cognitive engine of hyperactivation. If you have ever spent forty minutes dissecting a two-word text, you know this loop. For a closer look at that specific pattern, see why you panic when your partner does not text back.
Realizing you have been spiraling for the last hour does not mean something is wrong with you. Your brain is running a pattern it learned was necessary. Grounding gives it something else to do.
The 5-4-3-2-1 Grounding Walk-Through (for anxious attachment)
- Name 5 things you can see — say them out loud if possible
- Name 4 things you can hear — including background sounds you usually filter out
- Name 3 things you can physically feel — the chair beneath you, the texture of your sleeve, air on your skin
- Name 2 things you can smell — or walk toward a scent (coffee, soap, fresh air)
- Name 1 thing you can taste — take a sip of water, notice the temperature
This works for anxious attachment because prefrontal cortex engagement during sensory grounding directly competes with amygdala-driven rumination. You cannot catastrophize and count ceiling tiles at the same time. Breaking the rumination loop interrupts the hyperactivating cycle before it escalates into protest behavior.
Technique 5: Self-Compassion Pause
The voice that says "I'm too much," "I'm driving them away," "no one could love someone this needy"—that is the anxious attachment talking, not the truth. Your nervous system learned to turn pain inward when connection felt uncertain. It kept you from being "too much." And now you can offer yourself what you have been desperately seeking from others.
Self-compassion mediates the pathway between attachment anxiety and psychological distress (Thimm, 2017). A meta-analysis found a large effect size (r = −0.54) for the association between higher self-compassion and lower psychopathology (MacBeth and Gumley, 2012). Kristin Neff's three components—self-kindness, common humanity, and mindfulness—directly target the self-criticism that fuels anxious spirals (Neff and McGehee, 2010).
The Self-Compassion Pause (for anxious attachment)
- Place one hand on your heart
- Say: "This is a moment of suffering." (Mindfulness—acknowledging without over-identifying)
- Say: "Other people with anxious attachment feel this same fear right now." (Common humanity—you are not alone in this)
- Say: "May I give myself the compassion I'm seeking from someone else." (Self-kindness—turning warmth inward)
- Stay with the warmth of your hand on your chest for 30 seconds
Harsh self-criticism ("I'm too needy") intensifies the activation spiral—you feel bad about feeling bad, which drives more desperate reaching. Self-compassion interrupts this by providing internal warmth, the very thing the anxious system is seeking externally.
Technique 6: Secure Base Visualization (Security Priming)
Security priming—guided imagery of a secure attachment figure—is the strongest attachment-specific self-soothing intervention in the research literature. A systematic review found that security priming effects are especially strong for anxiously attached individuals (Gillath and Karantzas, 2019). Repeated priming shows cumulative benefits over time (Carnelley and Rowe, 2020), and fMRI studies demonstrate that it alters amygdala reactivity patterns (Tang et al., 2017). It has also been shown to diminish conflict-based anger and anxiety (Boykin et al., 2016) and improve working memory performance in anxiously attached individuals specifically (Bai et al., 2018).
The Secure Base Visualization (for anxious attachment)
- Close your eyes and take three slow breaths
- Picture someone who has made you feel genuinely safe—a grandparent, therapist, friend, partner, even a fictional character
- Visualize their face in detail
- Recall a specific moment they made you feel accepted exactly as you are
- Imagine them saying: "You are safe. You are enough. I'm not going anywhere."
- Stay with that feeling for 2 minutes
- Practice daily—research shows the effects compound with repetition
Security priming temporarily activates the neural signature of secure attachment, building a new template that competes with the anxious one. Your brain cannot distinguish between vividly imagined and actual secure base experiences at the neural level—so you are essentially rehearsing what security feels like. Over time, this creates what researchers call earned secure attachment.
What Are Long-Term Self-Soothing Practices for Anxious Attachment?
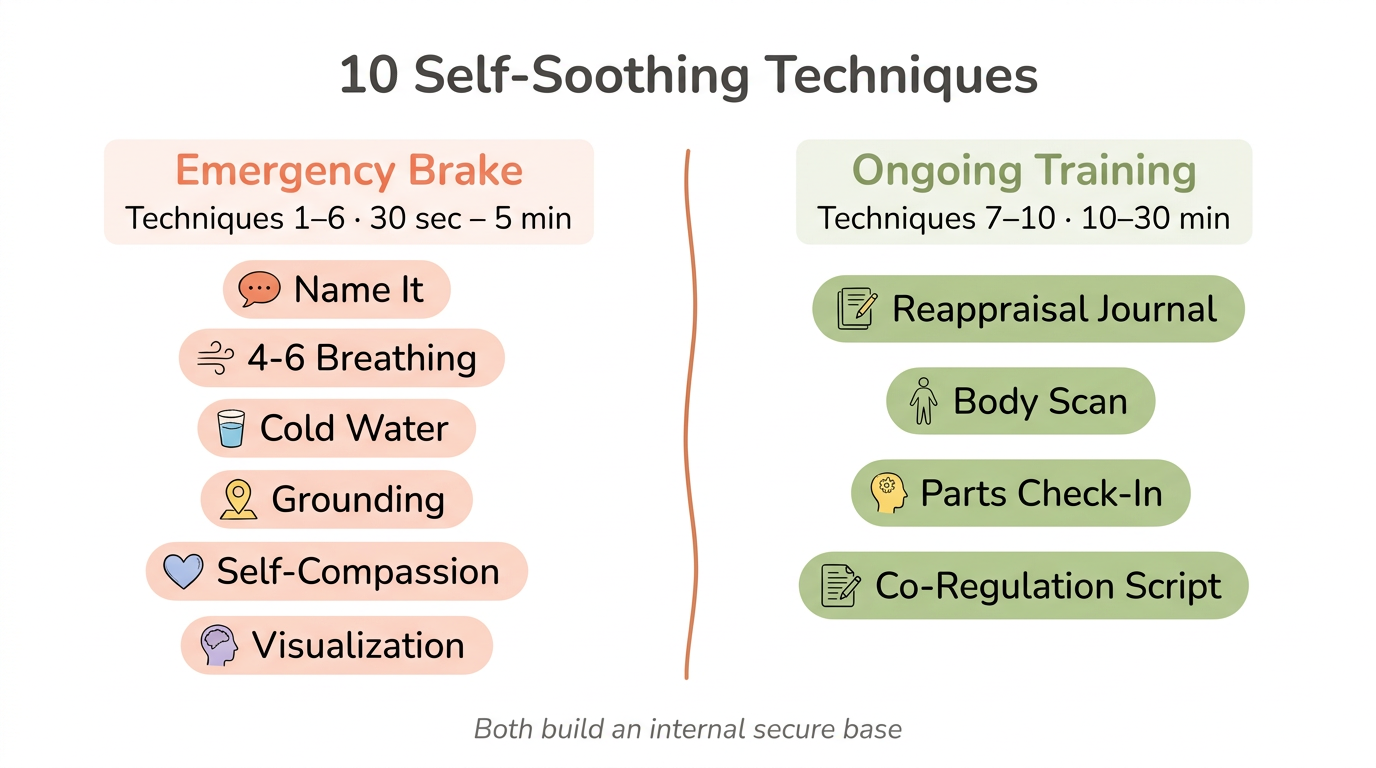
Long-term self-soothing practices for anxious attachment include cognitive reappraisal journaling, body scans for somatic tracking, IFS-informed parts check-ins, and co-regulation request scripts. Think of techniques 1 through 6 as the emergency brake. Techniques 7 through 10 are the ongoing training that makes the brake more responsive.
Technique 7: Cognitive Reappraisal Journaling
Combining expressive writing with cognitive reappraisal creates a two-pronged intervention uniquely suited to anxious attachment. A meta-analysis of expressive writing found an average 9 percent reduction in anxiety symptoms (Sohal et al., 2022), and a positive affect journaling RCT showed reduced mental distress and greater resilience (Smyth et al., 2018). The key insight: anxiously attached individuals can use cognitive reappraisal effectively—unlike suppression, which backfires (Viddal et al., 2023).
Your tendency to assume the worst about ambiguous situations is not a character flaw. Anxious attachment exaggerates negative appraisals because your nervous system was trained to scan for threats to connection (Mikulincer and Shaver, 2003). Journaling gives you a structured way to interrupt that pattern using the one regulation strategy your brain responds to well.
The Reappraisal Journal (for anxious attachment)
- Write what happened—facts only, 2 to 3 sentences
- Write the story your anxious attachment told: "They're pulling away, they don't love me anymore"
- Write 3 alternative explanations that are equally or more plausible
- Write what you would tell a close friend in this exact situation
- Do this within 24 hours of the activation
This works for anxious attachment because it combines affect labeling (which downregulates the amygdala) with cognitive reappraisal (the one emotion regulation strategy this population can use effectively). Writing the anxious story alongside alternatives makes the distortion visible—and once you can see it, it loosens its grip.
Technique 8: Body Scan for Somatic Tracking
That chest tightness, the knot in your stomach, the constriction in your throat—those are not just metaphors. Your body is holding activation that your mind cannot think its way out of. Anxious attachment keeps you "in your head"—ruminating, analyzing, seeking answers cognitively.
Somatic tracking redirects attention from those spinning thoughts to the physical sensations where the activation actually lives. Bottom-up processing through the body builds the interoceptive awareness that is foundational to self-regulation.
The Somatic Tracking Scan (for anxious attachment)
- Lie down or sit comfortably. Close your eyes.
- Starting at the crown of your head, slowly scan downward through your body
- When you find tension, heat, tightness, or buzzing, pause there
- Name it: "There's a knot in my solar plexus"
- Describe it: size, shape, temperature, texture
- Breathe into that area for 3 slow breaths
- Ask: "What does this sensation need?"
- Notice if it shifts, moves, or releases. Do not force change—just witness.
Hyperactivation keeps you locked in cognitive loops—analyzing texts, rehearsing conversations, catastrophizing. Somatic tracking breaks the loop by redirecting attention to where the activation actually lives. Over time, this builds body literacy: the ability to notice activation in your body before it hijacks your behavior.
Technique 9: Parts Check-In (IFS-Informed)
Your anxious part is a protector, not a problem. Internal Family Systems therapy frames anxious hyperactivation as a young protective part stuck in an old strategy. That part learned to scream because inconsistent caregiving meant louder signals were more likely to get needs met. The Self—the calm, curious, compassionate center of you—can become an internal secure base for this part.
Rather than fighting the anxiety (which only triggers more activation), parts work invites you to relate to it the way a secure caregiver would: with curiosity and warmth. Over time, the anxious part updates its strategy because it no longer needs to scream to be heard.
The Parts Check-In (for anxious attachment)
Instead of fighting the anxiety—which your nervous system interprets as another threat—this exercise builds a Self-to-part relationship that mirrors the secure attachment bond you are developing internally. You relate to the anxious part the way a secure caregiver would.
- Notice the anxious feeling without trying to fix it
- Say internally: "I see you. I know you're trying to protect me."
- Ask: "What are you afraid will happen?"
- Listen without arguing or rationalizing
- Respond: "Thank you for trying to keep me safe. I'm here now. We're okay."
- Ask: "What do you need from me right now?"
- Offer what it needs—sometimes just your attention is enough
Technique 10: Co-Regulation Request Script
When self-soothing is not enough, asking for co-regulation is healthy—not a failure. The difference between healthy interdependence and anxious dependency is how you ask. Protest behavior—passive aggression, withdrawing to get a reaction, testing your partner—is the hyperactivating system's default request. A direct, non-blaming request is the secure alternative. For more on making these requests effectively, see how to communicate your needs without triggering your partner.
Your need for connection is not the problem. The way anxious attachment packages that need—through urgency, testing, and indirect signals—is what creates the anxious-avoidant trap. You can learn to ask clearly.
The Co-Regulation Script (for anxious attachment)
- Self-soothe first: use techniques 1 through 6 for at least 5 minutes
- Name what you are feeling: "I'm feeling anxious and disconnected right now"
- Name what you need: "Could you hold my hand for a few minutes?" or "Could you tell me we're okay?"
- Accept their response without interpreting it through your anxious lens
- If they cannot co-regulate right now, return to self-soothing—their unavailability in this moment is not rejection
Security does not mean never needing others—that is avoidance. Security means asking for support directly rather than through hyperactivating protest behaviors. This technique bridges self-soothing and co-regulation, building the flexible access to both that defines secure attachment.
In-the-Moment vs. Long-Term Techniques: A Comparison
| In-the-Moment (Techniques 1–6) | Long-Term Practice (Techniques 7–10) | |
|---|---|---|
| When to use | During an activation or trigger | Daily or weekly as ongoing practice |
| Time required | 30 seconds to 5 minutes | 10 to 30 minutes per session |
| Primary mechanism | Nervous system downregulation | Neural pathway rewiring |
| Examples | Affect labeling, 4-6 breathing, TIPP, grounding, self-compassion pause, secure base visualization | Reappraisal journaling, body scan, parts check-in, co-regulation scripts |
| What it builds | Distress tolerance | Earned security over time |
| Works best when | You catch the activation early | Practiced consistently, even on calm days |
| Attachment-specific benefit | Interrupts the hyperactivating cycle | Builds an internal secure base |
What Does the Neuroscience Say About Self-Soothing and Attachment?
Neuroscience research shows anxious attachment involves amygdala hyperreactivity to social threat and weaker amygdala-prefrontal cortex connectivity—and these self-soothing techniques target both pathways to produce measurable neural changes. Anxious attachment correlates with amygdala hyperreactivity—your brain's threat detection center fires more intensely and more quickly in response to social cues like angry facial expressions (Vrtička et al., 2008). At the same time, the amygdala-PFC connectivity that allows for top-down regulation is weaker in insecurely attached individuals (Moutsiana et al., 2019).
Resting-state fMRI research shows that attachment anxiety is associated with distinct patterns of neural activity in the amygdala, insula, and anterior cingulate cortex—brain regions involved in emotional processing and threat monitoring (Li et al., 2021). Oxytocin, the neurochemical of bonding, has been shown to reduce amygdala reactivity to social threat and enhance amygdala-PFC connectivity (Dodhia et al., 2014).
Each technique category targets a different part of this neural circuit:
- Affect labeling (Technique 1) engages the prefrontal cortex, which directly downregulates amygdala activation (Lieberman et al., 2007)
- Extended exhale breathing (Technique 2) stimulates the vagus nerve, activating the parasympathetic nervous system and shifting from sympathetic overdrive (Porges, 2011)
- Security priming (Technique 6) alters amygdala reactivity patterns to emotional faces—literally retraining your brain's social threat response (Tang et al., 2017)
- Cognitive reappraisal (Technique 7) recruits prefrontal regions to reinterpret threatening stimuli
- Somatic tracking (Technique 8) builds interoceptive awareness, strengthening the insula's capacity to process body signals before they escalate
You are not just calming yourself down. You are gradually building the neural architecture that consistent early caregiving would have built. That is the science behind earned secure attachment.
When Should You Seek Professional Help for Anxious Attachment?
Self-soothing techniques are a starting point, not a replacement for therapy. They work best as a complement to professional support—not a substitute for it.
Consider seeking an attachment-informed therapist if:
- These techniques do not reduce your activation after several weeks of consistent practice
- Anxiety interferes with your ability to function at work, in friendships, or in daily life
- Relationship patterns keep repeating despite your growing awareness of them
- You have a history of trauma—particularly early relational trauma—that underlies the anxious attachment
- You find yourself in a recurring anxious-avoidant dynamic that neither partner can break alone
Attachment-informed therapy modalities include Emotionally Focused Therapy (EFT), which has a 70 to 75 percent recovery rate for couples across more than 20 outcome studies (ICEEFT), as well as EMDR, somatic experiencing, and Internal Family Systems therapy. Individual EFT specifically addresses self-soothing at the "anxious dependence" stage of treatment. If your relationship anxiety surfaces even when things are going well, that pattern is particularly worth exploring with a professional.
You do not rewire attachment in a single insight. You rewire it by noticing the pattern a little earlier each time and responding a little differently. Each time you do, the new wiring strengthens. These techniques give you the starting tools. A therapist helps you go deeper.
Frequently Asked Questions
What does self-soothing mean in attachment theory?
Self-soothing is the ability to calm your nervous system independently when emotionally activated. Securely attached children develop this skill through consistent caregiving. Anxiously attached individuals often missed this developmental window and can build it through intentional practice as adults.
Why is it so hard for anxiously attached people to self-soothe?
Anxious attachment uses hyperactivating strategies—intensifying emotions to demand care from others. Your brain learned that louder distress meant more likely to get needs met, making quiet internal regulation feel counterintuitive and unsafe. Self-soothing requires the opposite skill set.
Can you learn to self-soothe if you never learned it as a child?
Yes. Neuroplasticity means your brain can build new regulatory pathways at any age. Research on security priming shows anxiously attached adults can develop secure base representations through repeated practice, with cumulative benefits over time (Carnelley and Rowe, 2020). This is the foundation of earned secure attachment.
How long does it take to change your attachment style?
Meaningful shifts in attachment security can occur within months of consistent practice, though deep change typically unfolds over one to three years. Security priming studies show measurable neural changes after just weeks of daily practice. Therapy accelerates the process significantly. Learn more about how attachment styles change over time.
Can meditation help with anxious attachment?
Yes. An RCT found that adults with moderate-to-high attachment anxiety experienced significantly larger improvements in positive emotions and reductions in negative emotions after 10 weeks of mindfulness or loving-kindness meditation compared to securely attached participants (Rowe et al., 2022). A separate RCT found MBSR reduced both somatization and attachment anxiety (Ahmadi et al., 2024).
What is the difference between self-soothing and self-care?
Self-soothing is real-time nervous system regulation during emotional activation—techniques you use in the moment of distress. Self-care refers to ongoing practices that support general wellbeing, like sleep, nutrition, exercise, and boundaries. Self-soothing is an emergency brake; self-care is routine maintenance.
How do I stop seeking reassurance from my partner?
Rather than eliminating the need entirely—which leads to avoidance, not security—practice self-soothing first. Use techniques like affect labeling, breathing, or the self-compassion pause for at least five minutes. If you still need connection, make a direct co-regulation request rather than using indirect protest behaviors or people-pleasing.
Is anxious attachment the same as an anxiety disorder?
No. Anxious attachment is a relational pattern that activates primarily in the context of close relationships and perceived threats to connection. Anxiety disorders involve pervasive worry across multiple life domains. However, they frequently co-occur, and anxious attachment can amplify generalized anxiety symptoms.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Attachment Theory and Emotion Regulation
- Mikulincer, M., & Shaver, P. R. (2019). Attachment orientations and emotion regulation. Current Opinion in Psychology, 25, 6–10.
- Mikulincer, M., & Shaver, P. R. (2003). The attachment behavioral system in adulthood: Activation, psychodynamics, and interpersonal processes. Motivation and Emotion, 27(2), 77–102.
- Pascuzzo, K., Bhatt, M., & Bhatt, P. (2023). Emotion regulation and attachment: A review of the literature. Frontiers in Behavioral Neuroscience, 17, 1141607.
- Viddal, K. R., et al. (2023). Attachment and emotion regulation: A systematic review. PMC.
- Hazan, C., & Shaver, P. (1987). Romantic love conceptualized as an attachment process. Journal of Personality and Social Psychology, 52(3), 511–524.
Security Priming
- Gillath, O., & Karantzas, G. (2019). Attachment security priming: A systematic review. Current Opinion in Psychology, 25, 86–95.
- Carnelley, K. B., & Rowe, A. C. (2020). Repeated priming of attachment security influences later views of self and relationships. Personal Relationships, 14(2), 307–320.
- Tang, N., et al. (2017). Secure attachment priming alters emotional face processing bias in anxiously attached individuals: An fMRI study. Frontiers in Psychology, 8, 624.
- Tang, N., et al. (2022). Security priming delays negative information-related attentional disengagement in anxiously attached individuals. Frontiers in Psychology, 13, 913805.
- Boykin, D. M., et al. (2016). Secure base priming diminishes conflict-based anger and anxiety. PLOS ONE, 11(9), e0162374.
- Bai, L., et al. (2018). Attachment anxiety benefits from security priming on working memory performance. PLOS ONE, 13(3), e0193645.
Self-Compassion
- Neff, K. D., & McGehee, P. (2010). Self-compassion and psychological resilience among adolescents and young adults. Self and Identity, 9(3), 225–240.
- MacBeth, A., & Gumley, A. (2012). Exploring compassion: A meta-analysis of the association between self-compassion and psychopathology. Clinical Psychology Review, 32(6), 545–552.
- Thimm, J. C. (2017). Relationships between early maladaptive schemas, mindfulness, self-compassion, and psychological distress. International Journal of Psychology and Psychological Therapy, 17(1), 3–17.
Mindfulness and Meditation
- Rowe, A. C., et al. (2022). Mindfulness and loving-kindness meditation for attachment insecurity: A randomized controlled trial. PMC.
- Hoge, E. A., et al. (2013). Randomized controlled trial of mindfulness meditation for generalized anxiety disorder: Effects on anxiety and stress reactivity. Journal of Clinical Psychiatry, 74(8), 786–792.
- Ahmadi, S., et al. (2024). Efficacy of mindfulness-based stress reduction on reducing somatization and attachment anxiety: A randomized controlled trial. ResearchGate.
Journaling and Expressive Writing
- Sohal, M., et al. (2022). Efficacy of journaling in the management of mental illness: A systematic review and meta-analysis. Family Medicine and Community Health, 10(1).
- Smyth, J. M., et al. (2018). Online positive affect journaling in the improvement of mental distress and well-being in general medical patients with elevated anxiety symptoms: A preliminary randomized controlled trial. JMIR Mental Health, 5(4), e11290.
Neuroscience
- Vrtička, P., et al. (2008). Individual attachment style modulates human amygdala and striatum activation during social appraisal. PLOS ONE, 3(8), e2868.
- Moutsiana, C., et al. (2019). Insecure attachment during infancy predicts greater amygdala volumes in early adulthood. PMC.
- Li, X., et al. (2021). Neural basis of attachment anxiety: A resting-state fMRI study. BMC Neuroscience, 22, 617.
- Lieberman, M. D., et al. (2007). Putting feelings into words: Affect labeling disrupts amygdala activity in response to affective stimuli. Psychological Science, 18(5), 421–428.
- Dodhia, S., et al. (2014). Modulation of resting-state amygdala-frontal functional connectivity by oxytocin in generalized social anxiety disorder. Neuropsychopharmacology, 39(9), 2061–2069.
- Porges, S. W. (2011). The polyvagal theory: Neurophysiological foundations of emotions, attachment, communication, and self-regulation. Norton.
Therapy Outcomes and Prevalence
- ICEEFT. EFT research: Over 20 outcome studies showing 70–75% recovery rate for couples.
- Diehl, M., et al. (2015). Change in attachment security in adulthood: The role of personality and health. Psychology and Aging, 30(3), 462–478.
This article is for educational purposes only and is not a substitute for professional mental health treatment. If you are experiencing significant distress related to your attachment patterns, please consult a licensed therapist who specializes in attachment-informed approaches. Meadow provides guided exercises and psychoeducation but is not a therapy service.
