Attachment style affects your nervous system by programming your autonomic threat-detection defaults — shaping how your body responds to stress, safety, and connection before conscious thought enters the picture. fMRI research shows that amygdala activation correlates with attachment insecurity at an R-squared of 0.72 (Lemche et al., 2005), meaning your attachment pattern explains approximately 72 percent of the variance in your brain's threat response during stress.
If you have ever wondered why you cannot "just calm down" during conflict, or why you shut down emotionally even when you want to engage, the answer likely lives in your nervous system — not your willpower. Your nervous system learned these responses for good reason. They kept you safe. And now, with the right tools, you can teach it something new. This article maps exactly how each attachment style creates distinct neurobiological signatures, and what you can do about it.
Key takeaway: Your attachment style literally wires your nervous system's threat-detection defaults. Anxious attachment keeps your fight-or-flight on high alert with elevated cortisol and amygdala hyperactivation. Avoidant attachment triggers shutdown while masking distress from conscious awareness. Secure attachment enables flexible nervous system regulation. The good news is that these patterns can be rewired through co-regulation, somatic practices, and expanding your window of tolerance.
What Does Your Nervous System Have to Do with Attachment?
Your nervous system and your attachment style are deeply intertwined because early caregiving experiences wire the autonomic nervous system's default responses to safety and threat. According to Stephen Porges' Polyvagal Theory (2011), the mammalian nervous system operates through three hierarchical states that map directly onto attachment patterns.
The first state is the ventral vagal pathway — the social engagement system. When this pathway is active, you feel safe, connected, and able to engage with others. Your breathing is easy, your muscles are relaxed, and your voice has natural prosody. Secure attachment develops this state as the default.
The second state is sympathetic activation — the fight-or-flight response. Your heart races, your muscles tense, and your body prepares for action. Anxious attachment tends to get stuck here, with the threat detector turned up too high.
The third state is dorsal vagal shutdown — the freeze or collapse response. Your body goes heavy, your mind goes blank, and you disconnect. Avoidant attachment patterns often engage this state as a protective strategy.
What makes this connection so powerful is a concept Porges (2022) calls neuroception — your nervous system's unconscious evaluation of safety or danger that happens below conscious awareness. Your attachment history calibrates this system. Insecure attachment tunes neuroception toward threat detection, triggering defensive autonomic states more easily. This is why telling yourself to "just relax" does not work — your nervous system decides before you do.
Three-State Body Scan
- Pause and notice your body right now
- Check for ventral vagal signs: relaxed jaw, easy breathing, openness to social contact
- Check for sympathetic signs: tight chest, racing heart, scanning for threat
- Check for dorsal vagal signs: heaviness, numbness, desire to disappear
- Name your state without judgment: "My nervous system is in ___"
How Does Anxious Attachment Affect the Nervous System?
Anxious attachment keeps the sympathetic nervous system locked in a state of sympathetic hyperactivation — fight-or-flight that is essentially stuck in the "on" position. Research by Kidd et al. (2011) found that anxious attachment predicts enhanced cortisol reactivity to psychosocial stress, meaning the body produces more stress hormones and takes longer to recover from relational threats.
At the brain level, fMRI research by Vrtička et al. (2008) shows that anxious attachment correlates with heightened amygdala and insula activation — the brain regions responsible for emotional threat detection and interoceptive awareness. Anxious attachment creates a nervous system that is exquisitely tuned to relational danger signals. This hypervigilance is not a character flaw. It is your nervous system doing exactly what it learned to do.
The hormonal picture reinforces this pattern. Pierrehumbert et al. (2012) found that insecurely attached individuals show lower oxytocin levels alongside dysregulated cortisol, creating a neurochemical environment where safety is harder to feel and stress is harder to recover from. Pietromonaco and Powers (2015) found that anxious attachment is even associated with fewer T-cells under high cortisol conditions, linking attachment anxiety to compromised immune function.
5 Nervous System Signs of Anxious Attachment
- Racing heart before checking your phone for a response from your partner
- Difficulty sleeping after unresolved conflict — your body will not let you rest
- Stomach tension or nausea when your partner seems emotionally distant
- Rapid emotional escalation — going from calm to overwhelmed in seconds
- Difficulty "coming down" after stress, even when the situation is resolved
If these nervous system patterns sound familiar, explore the 12 signs of anxious attachment to understand the full picture of how this pattern shows up.
The Physiological Sigh
- Notice when your heart rate spikes in a relational moment
- Take a double inhale through your nose — two short inhales, one on top of the other
- Follow with one long, slow exhale through your mouth
- Repeat 3 times
- Place a hand on your chest and notice the shift
The physiological sigh activates the parasympathetic brake and is research-backed to reduce sympathetic arousal faster than standard deep breathing. Try it for 30 seconds next time you feel your fight-or-flight stuck on.
Does Avoidant Attachment Cause Nervous System Shutdown?
Avoidant attachment does activate the dorsal vagal shutdown pathway, but with a fascinating and often overlooked twist: the body still registers the threat even when the mind does not. Pietromonaco and Powers (2015) found that avoidant individuals show greater physiological arousal — elevated skin conductance, elevated pre-conflict cortisol — while simultaneously reporting lower subjective distress. This is a measurable body-mind disconnect, and it is one of the most important findings in attachment neuroscience.
Avoidant attachment does not eliminate stress. It eliminates your awareness of stress. Your nervous system is reacting, but your deactivating strategies — emotional withdrawal, intellectualization, self-reliance — operate as cognitive suppression at the neural level. Vrtička (2012) found that avoidant attachment correlates with increased dorsolateral prefrontal cortex activation during emotional processing, the brain region responsible for overriding emotional experience with cognitive control.
This disconnect has real health consequences. Pietromonaco and Powers (2015) found that avoidant attachment is associated with heightened IL-6 inflammatory response during marital conflict — the body's stress shows up as inflammation even when the mind insists everything is fine. Bryant and Hutanamon (2018) found that imagining a safe attachment figure enhanced heart rate variability (parasympathetic recovery) for most people, but physiological arousal without awareness meant highly avoidant individuals showed no benefit from this intervention at all.
If you recognize this pattern of feeling fine while your body tells a different story, learn more about recognizing avoidant attachment patterns.
Interoception Check-In
- Set a timer for 60 seconds
- Without checking your pulse, estimate your heart rate
- Now check your actual heart rate (two fingers on your wrist or neck, count for 15 seconds and multiply by 4)
- Notice the gap — avoidant patterns often create a disconnect between felt experience and physiological reality
- Practice asking yourself once a day: "What is my body actually doing right now?"
Building interoceptive awareness is the antidote to the avoidant body-mind gap. Start with 30 seconds of noticing. That is enough.
What Is the Window of Tolerance and How Does Attachment Shape It?
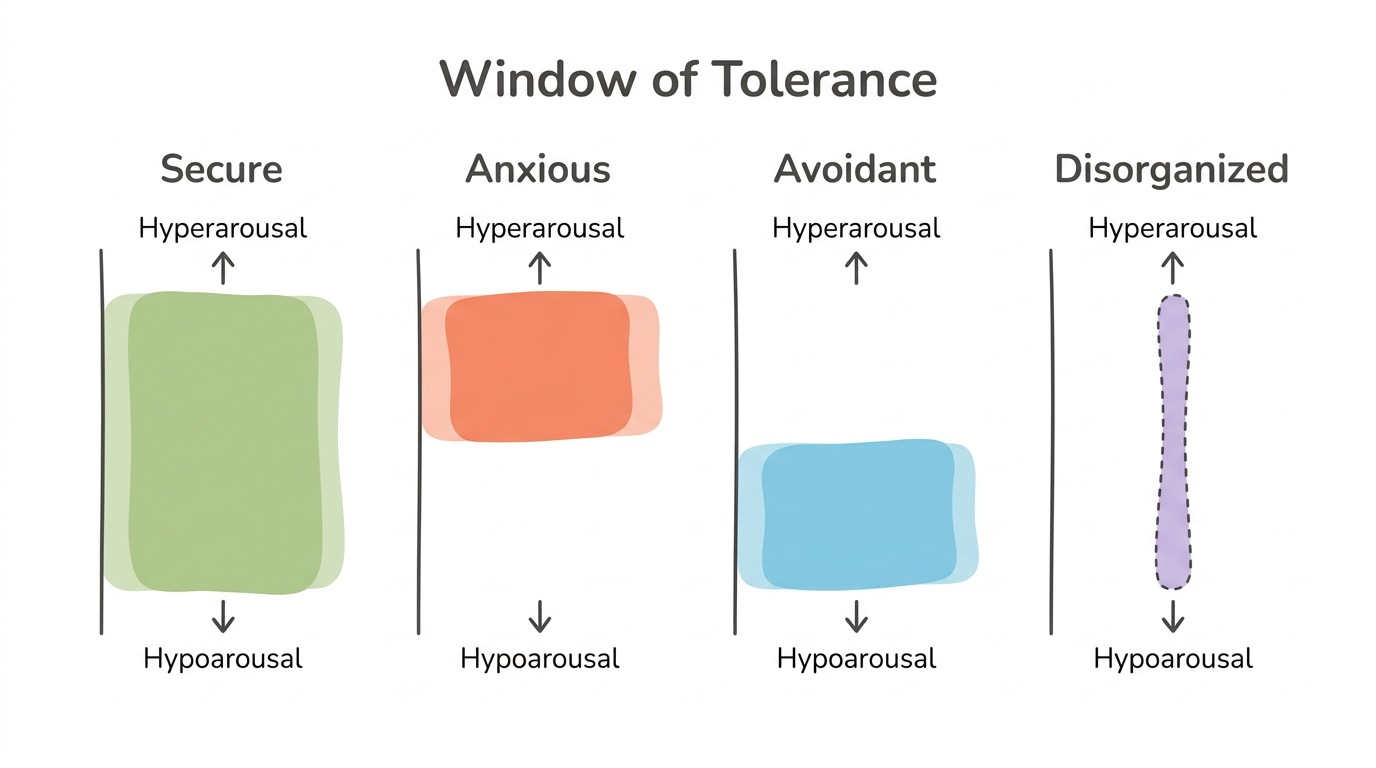
The window of tolerance, a concept developed by Daniel Siegel (1999), is the optimal arousal zone where your nervous system can process stress, engage with emotions, and function effectively. Inside your window, you can think clearly, feel your feelings, and stay connected to others. Outside it, you tip into either hyperarousal (panic, reactivity, emotional flooding) or hypoarousal (numbness, dissociation, shutdown).
Attachment history directly shapes how wide or narrow your window is. Secure attachment creates a wide, flexible window — you can tolerate more stress before tipping out. Anxious attachment creates a narrow window biased toward hyperarousal. Small relational cues — an unanswered text, a shift in tone — push you above your window into fight-or-flight. Avoidant attachment creates a narrow window biased toward hypoarousal. Emotional intensity pushes you below your window into numbness and disconnection. Disorganized attachment creates an extremely narrow window that collapses in both directions — the nervous system oscillates rapidly between hyperarousal and hypoarousal with little middle ground.
| Attachment Style | Window Width | Direction of Collapse | Typical Experience |
|---|---|---|---|
| Secure | Wide, flexible | Rarely collapses; recovers quickly | "I can handle this" |
| Anxious | Narrow | Upward — hyperarousal | "I can't calm down" |
| Avoidant | Narrow | Downward — hypoarousal | "I'm fine" (body disagrees) |
| Disorganized | Extremely narrow | Both directions rapidly | "I don't know what I feel" |
Window of Tolerance Self-Map
- Draw a horizontal band on paper and label it "My Window"
- Above it, write your hyperarousal signs (anxiety, racing thoughts, anger, restlessness)
- Below it, write your hypoarousal signs (numbness, zoning out, fatigue, brain fog)
- Identify which direction you tend to leave your window — this reveals your attachment pattern's nervous system signature
- List 3 things that widen your window (a safe person, time in nature, movement, music)
How Does Secure Attachment Regulate the Nervous System?
Secure attachment regulates the nervous system by enabling ventral vagal flexibility — the capacity to move fluidly between states of activation and rest without getting stuck. Secure attachment is not the absence of stress. It is the nervous system's ability to respond to stress and then recover, shifting back toward safety with relative ease.
The physiology of secure attachment is distinct and measurable. Pierrehumbert et al. (2012) found that securely attached individuals show moderate, adaptive cortisol responses — the stress system activates when needed and quiets when the threat passes — alongside higher oxytocin levels, the neurochemical of bonding and safety. Mikulincer and Shaver (2003) describe secure attachment as enabling flexible emotion regulation, drawing on both cognitive reappraisal and support-seeking depending on the situation.
One of the most compelling findings comes from Bryant and Hutanamon (2018): simply imagining a safe attachment figure measurably enhances heart rate variability — your nervous system's flexibility marker. Heart rate variability reflects autonomic flexibility, the ability to adapt to changing demands. Securely attached individuals show enhanced HRV and greater parasympathetic recovery. Recent fMRI research (2024) shows that secure participants also activate reward network circuitry more readily, experiencing both distress and comfort through a lens of connection rather than threat.
The concept of earned security means this nervous system flexibility is not reserved for people who had perfect childhoods. It can be developed. Co-regulation — the experience of being calmed by another regulated nervous system — gradually rewires autonomic defaults. Every time your nervous system experiences safety in the presence of another person, it learns that connection is not dangerous.
Safe Person HRV Boost
- Bring to mind someone who makes you feel genuinely safe — a partner, friend, therapist, or mentor
- Visualize their face, the sound of their voice, or a specific warm memory with them
- Notice what happens in your body: chest softening, breath deepening, jaw releasing
- Stay with this felt sense for 2 minutes
Research shows this practice measurably enhances heart rate variability (Bryant and Hutanamon, 2018). For avoidant-leaning readers: if imagining a person feels uncomfortable, start with a pet, a place in nature, or even a fictional character. The nervous system responds to felt safety regardless of the source.
How Each Attachment Style Affects Your Nervous System
| Dimension | Anxious | Avoidant | Disorganized | Secure |
|---|---|---|---|---|
| Dominant nervous system state | Sympathetic (fight or flight) | Dorsal vagal (freeze or shutdown) | Oscillates between all three | Ventral vagal (social engagement) |
| Cortisol pattern | Elevated reactivity, slow recovery | Elevated baseline, rapid suppression | Unpredictable spikes | Moderate, adaptive curve |
| Brain signature | Amygdala and insula hyperactivation | Dorsolateral PFC overactivation | Rapid switching between regions | Reward network activation |
| Oxytocin levels | Lower than secure | Lower than secure | Disrupted | Higher baseline |
| Heart rate variability | Reduced | Reduced, no benefit from attachment priming | Most disrupted | Enhanced, responsive to safe cues |
| Window of tolerance | Narrow, biased toward hyperarousal | Narrow, biased toward hypoarousal | Extremely narrow, collapses both directions | Wide and flexible |
| Subjective experience | "I can't calm down" | "I'm fine" (body disagrees) | "I don't know what I feel" | "I can handle this" |
| Immune impact | Fewer T-cells under stress | Higher IL-6 inflammation | Combined effects | Balanced immune function |
Can You Heal Your Nervous System from Attachment Trauma?
Yes — neuroplasticity allows nervous system patterns shaped by attachment to change throughout life. The brain and autonomic nervous system are not fixed by childhood experience. They are shaped by it, and they can be reshaped by new experience. The key is that rewiring happens through the body and through relationship, not through insight alone.
The strongest evidence comes from Emotionally Focused Therapy. EFT has the largest effect size (d=1.3) of any couples intervention (Johnson et al., 1999), and fMRI studies show it changes how partner contact mediates brain responses to threat. Somatic Experiencing, developed by Peter Levine, directly addresses nervous system dysregulation through techniques like titration — approaching activation gradually — and pendulation — moving attention between areas of activation and areas of calm in the body (Payne et al., 2015).
Understanding the oxytocin feedback loop helps explain both why healing takes time and how it works. Insecure attachment produces lower oxytocin levels, which makes it harder to feel safe, which reinforces insecure attachment — a self-perpetuating cycle. Co-regulation breaks this cycle. Every experience of being calmed by a safe, regulated person stimulates oxytocin, gradually rebuilding the neurochemical foundation for trust (Pierrehumbert et al., 2012).
6 Evidence-Informed Practices for Nervous System Healing
- Co-regulation with safe people — spend time with regulated nervous systems; safety is contagious
- Vagal toning — humming, cold water on the face, and extended-exhale breathing directly activate the ventral vagal pathway
- Somatic tracking — notice body sensations without trying to fix them; observation itself begins to shift the pattern
- Titrated exposure to relational triggers — approach difficult relational territory in small, manageable doses
- Therapy modalities — EFT, Somatic Experiencing, and Sensorimotor Psychotherapy each target the nervous system directly
- Consistent, predictable relational patterns — reliability rewires the threat-detection system more than grand gestures
You do not rewire attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often. Earned secure attachment is built through repetition, not willpower.
Vagal Toning Sequence
- Hum at a comfortable pitch for 30 seconds — the vibration stimulates the vagus nerve through the throat
- Splash cold water on your face or hold a cold cloth to your forehead for 15 seconds — this activates the dive reflex, slowing heart rate
- Take 5 breaths with your exhale twice as long as your inhale (4 counts in, 8 counts out)
- Notice the shift in your body
This sequence directly activates the ventral vagal pathway. Try it when you notice yourself leaving your window of tolerance in either direction.
When Should You Seek Professional Help for Nervous System Dysregulation?
Self-help practices are valuable, but trauma-informed therapy becomes essential when nervous system dysregulation significantly disrupts your daily functioning or relationships. Seek professional support if you experience frequent dissociation — feeling detached from your body, losing time, or "watching yourself from outside" — that you cannot bring yourself back from on your own.
Other signs that professional help is needed include flashbacks or intrusive memories tied to relational experiences, an inability to feel safe with anyone despite wanting connection, chronic dysregulation that persists for weeks at a time, panic attacks that escalate in frequency or intensity, emotional numbness that does not lift, and chronic health issues such as autoimmune conditions, persistent inflammation, or frequent illness that may be connected to attachment-related stress.
When seeking a therapist, look for practitioners trained in somatic or body-based approaches — Somatic Experiencing, Sensorimotor Psychotherapy, EMDR, or Emotionally Focused Therapy. Therapy for attachment-related nervous system patterns is not just "talking about feelings." It is co-regulation. A skilled therapist provides the regulated nervous system presence that helps yours learn a new default. The therapeutic relationship itself becomes the vehicle for rewiring — your nervous system learns safety through repeated experience, not through explanation.
Frequently Asked Questions
How does anxious attachment affect the nervous system?
Anxious attachment keeps the sympathetic nervous system on high alert, producing elevated cortisol, amygdala hyperactivation, and a narrowed window of tolerance biased toward hyperarousal. Research by Kidd et al. (2011) shows anxious attachment predicts enhanced cortisol reactivity to psychosocial stress. Vrtička et al. (2008) found heightened amygdala and insula activation in fMRI studies, confirming that the anxious brain is wired for relational threat detection.
What is the connection between polyvagal theory and attachment?
Polyvagal Theory identifies three nervous system states — ventral vagal (safety and social engagement), sympathetic (fight or flight), and dorsal vagal (freeze and shutdown) — that map directly onto attachment patterns. Secure attachment develops ventral vagal flexibility, while insecure attachment biases the nervous system toward defensive states. Porges (2011) demonstrated that mammalian attachment is fundamentally linked to vagal tone and the capacity for social engagement.
Can you heal your nervous system from attachment trauma?
Yes. Neuroplasticity allows nervous system patterns to change through consistent co-regulation, somatic practices, and therapy. Emotionally Focused Therapy shows the largest effect size (d=1.3) of any couples intervention for building secure attachment (Johnson et al., 1999). Vagal toning exercises, Somatic Experiencing, and safe relational experiences gradually rewire autonomic defaults toward flexibility and safety.
What does nervous system dysregulation feel like?
Nervous system dysregulation manifests as either hyperarousal (racing heart, anxiety, inability to calm down, hypervigilance) or hypoarousal (emotional numbness, brain fog, heaviness, desire to withdraw). Many people oscillate between both states. These experiences feel involuntary because they are driven by autonomic processes below conscious awareness — your nervous system responds before your thinking mind can intervene.
Does avoidant attachment cause nervous system shutdown?
Avoidant attachment activates the dorsal vagal shutdown pathway, but with a key twist: the body still shows elevated physiological arousal (skin conductance, cortisol) even while the person reports feeling fine. Pietromonaco and Powers (2015) documented this measurable body-mind disconnect. Avoidant individuals experience stress physiologically without conscious awareness of it, which can contribute to inflammation and immune dysfunction over time.
What is the window of tolerance and how does it relate to attachment?
The window of tolerance, developed by Daniel Siegel (1999), is the optimal zone of nervous system arousal where you can function effectively. Secure attachment creates a wide, flexible window. Anxious attachment narrows the window with a bias toward hyperarousal — tipping into panic and reactivity. Avoidant attachment narrows it toward hypoarousal — tipping into numbness and disconnection. Disorganized attachment collapses the window in both directions.
What is neuroception and how does it relate to attachment?
Neuroception is the nervous system's unconscious evaluation of safety or danger, a concept coined by Stephen Porges (2022). Attachment history calibrates your neuroception — insecure attachment tunes the system toward threat detection, triggering defensive autonomic states more easily. Neuroception explains why telling yourself to "just relax" rarely works: the safety-or-danger assessment happens before conscious thought.
How does childhood attachment affect the brain?
Childhood attachment shapes the developing brain's stress-response architecture in measurable ways. Insecure attachment correlates with heightened amygdala reactivity (Lemche et al., 2005), altered cortisol patterns, lower oxytocin levels (Pierrehumbert et al., 2012), reduced heart rate variability, and immune function changes — including fewer T-cells and elevated inflammatory markers — that persist into adulthood (Pietromonaco and Powers, 2015).
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Polyvagal Theory and Neuroception
- Porges, S. W. (2011). The polyvagal theory: Neurophysiological foundations of emotions, attachment, communication, and self-regulation. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC3490536/
- Porges, S. W. (2022). Polyvagal Theory: A science of safety. Frontiers in Integrative Neuroscience. https://pmc.ncbi.nlm.nih.gov/articles/PMC9131189/
Neuroimaging and Biomarkers
- Lemche, E., et al. (2005). Human attachment security is mediated by the amygdala: Evidence from combined fMRI and psychophysiological measures. Human Brain Mapping. https://pmc.ncbi.nlm.nih.gov/articles/PMC6871466/
- Vrtička, P., et al. (2008). Individual attachment style modulates human amygdala and striatum activation during social appraisal. PLOS ONE. https://journals.plos.org/plosone/article/file?id=10.1371/journal.pone.0002868&type=printable
- Vrtička, P. (2012). The social neuroscience of attachment. Social Neuroscience. Université de Genève. https://www.unige.ch/fapse/e3lab/files/2415/5501/7183/Vrticka_2012_SocialNeuroscience.pdf
Stress Hormones and Physiology
- Kidd, T., et al. (2011). Attachment style and cortisol responses to psychosocial stress. Psychoneuroendocrinology. https://pmc.ncbi.nlm.nih.gov/articles/PMC3114075/
- Pierrehumbert, B., et al. (2012). Attachment and oxytocin response to stress in adult women. Biological Psychology. https://pubmed.ncbi.nlm.nih.gov/22856618/
- Pietromonaco, P. R., & Powers, S. I. (2015). Attachment and health-related physiological stress processes. Current Opinion in Psychology, 1, 34–39. https://pmc.ncbi.nlm.nih.gov/articles/PMC4341899/
- Bryant, R. A., & Hutanamon, T. (2018). Activating attachments enhances heart rate variability. PLOS ONE. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0151747
Emotion Regulation and Theory
- Mikulincer, M., & Shaver, P. R. (2003). Attachment theory and affect regulation: The dynamics, development, and cognitive consequences of attachment-related strategies. Motivation and Emotion, 27(2), 77–102. https://adultattachment.faculty.ucdavis.edu/wp-content/uploads/sites/66/2015/09/Mikulincer_2003_Attachment-theory-and-affect-regulation.pdf
- Siegel, D. J. (1999). The Developing Mind: How Relationships and the Brain Interact to Shape Who We Are. Guilford Press. Window of tolerance concept: https://www.psychologytools.com/resource/window-of-tolerance
Therapeutic Approaches
- Johnson, S., et al. (1999). Emotionally Focused Therapy: Status and challenges. Clinical Psychology: Science and Practice. Meta-analysis: https://iceeft.com/eft-research-3/
- Payne, P., Levine, P. A., & Crane-Godreau, M. A. (2015). Somatic Experiencing: Using interoception and proprioception as core elements of trauma therapy. Frontiers in Psychology. https://pmc.ncbi.nlm.nih.gov/articles/PMC4316402/
- Somatic Experiencing scoping review. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8276649/
Epidemiology
- Mickelson, K. D., Kessler, R. C., & Shaver, P. R. (1997). Adult attachment in a nationally representative sample. Journal of Personality and Social Psychology, 73(5), 1092–1106. https://pubmed.ncbi.nlm.nih.gov/26213376/
This article is for educational purposes only and is not a substitute for professional mental health care. If you are experiencing significant distress related to attachment or nervous system dysregulation, please consult a licensed therapist or counselor who specializes in attachment-informed or somatic approaches.
