Anxious attachment is a relational pattern characterized by a negative self-model and a hyperactivated attachment system that drives reassurance-seeking, fear of abandonment, and difficulty self-soothing. Bartholomew and Horowitz (1991) defined it as a combination of negative self-image and positive other-image — creating emotional dependency and hypervigilance to relationship threats. Approximately 19 percent of adults report anxious-preoccupied attachment (Hazan and Shaver, 1987), making it one of the most common insecure attachment styles.
If you have ever checked your phone obsessively after sending a text, felt a wave of panic when a partner pulled away, or struggled to believe that someone truly loves you — your attachment system may be running the show. Anxious attachment is not a character flaw. It is a neurobiological adaptation your nervous system developed in response to early relational experiences. This guide covers where anxious attachment comes from, what it looks like in relationships, what happens in your brain when it activates, and concrete steps you can take toward earned security.
Key takeaway: Anxious attachment affects approximately 19 percent of adults and is driven by a hyperactivated threat-detection system rooted in inconsistent early caregiving. It shows up as reassurance-seeking, protest behaviors, and difficulty self-soothing. Through nervous system regulation, secure relationship experiences, and therapeutic approaches like Emotionally Focused Therapy, anxiously attached individuals can develop earned security over time.
What Is Anxious Attachment and Where Does It Come From?
Anxious attachment is a relational pattern that develops when early caregiving is inconsistent — sometimes warm and responsive, sometimes emotionally unavailable. This unpredictability teaches a child that love is real but unreliable, wiring their nervous system to stay on high alert for signs of disconnection.
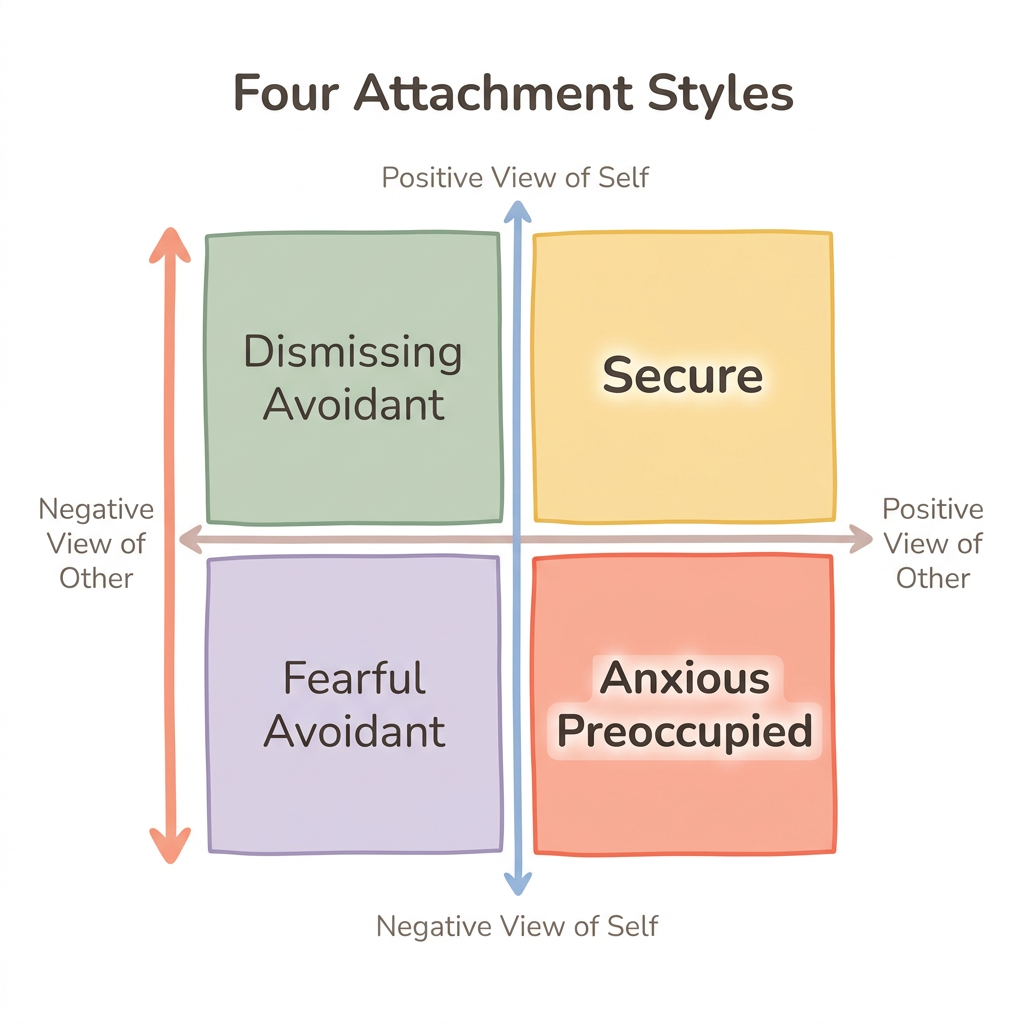
Bowlby described this through the lens of internal working models — mental templates formed in childhood that shape how you see yourself and others. In anxious attachment, the self-model is negative ("I'm not worthy of love") while the other-model is positive but uncertain ("Others can give love, but they might leave"). This combination drives a lifelong pursuit of approval and reassurance.
Hazan and Shaver (1987) translated these infant attachment patterns into adult romantic love and found roughly the same prevalence distribution. Their original research identified approximately 56 percent of adults as secure, 25 percent as avoidant, and 19 percent as anxious-ambivalent. Bartholomew and Horowitz (1991) later refined this into a four-category model, placing anxious attachment in the "preoccupied" quadrant — characterized by emotional dependency, low self-esteem, and a hyperactivation strategy designed to keep attachment figures close.
You are not alone in this pattern — and the prevalence data reflects that. Women show anxious attachment at a rate of 24 percent compared to 19 percent in men. Among young adults aged 18 to 25, approximately 18 percent display preoccupied attachment, while rates drop to 11 percent in adults over 60. Secure attachment among US college students has declined from 49 percent to 42 percent between 1988 and 2011, suggesting insecure attachment styles are becoming more prevalent.
Mikulincer and Shaver describe hyperactivation as the core strategy of anxious attachment: a chronic intensification of negative emotions — jealousy, anger, sadness, shame — designed to attract the attachment figure's attention. Your nervous system learned this response because, at some point, amplifying distress was the most effective way to get a caregiver to respond.
Origin Story Reflection (for anxious attachment)
- Write down 3 early memories of needing comfort from a caregiver
- For each memory, ask: Was the response consistent? Did you get comfort sometimes but not others?
- Notice how unpredictability felt in your body — was there tension, urgency, a pit in your stomach?
- Write one sentence connecting that early experience to a pattern you notice today
- Read it back without judgment — just notice
This exercise targets anxious attachment by connecting current relational patterns to early templates. Building this reflective awareness is what researchers identify as key to developing earned security — you cannot revise a story you have not yet read.
What Does Anxious Attachment Look Like in Relationships?
Anxious attachment shows up as protest behaviors — indirect attempts to reestablish connection when the attachment system perceives a threat. These behaviors shift depending on the relationship stage, but they share a common root: your nervous system has detected danger and is mobilizing every strategy it knows to restore closeness.
In early dating, anxious attachment often looks like intensity. You may fall fast, feel consumed by a new connection, and read deeply into every text, pause, or glance. What others experience as casual interest, your nervous system registers as a life-or-death question: Will this person stay?
Committed relationships bring a different flavor. The hyperactivated attachment system shifts toward reassurance-seeking and monitoring. You might need your partner to say "I love you" more often, feel unsettled by their friendships, or keep a mental scoreboard of who initiates contact more. Levine and Heller describe these as protest behaviors — not manipulation, but a nervous system in alarm mode trying to resolve a perceived attachment disruption.
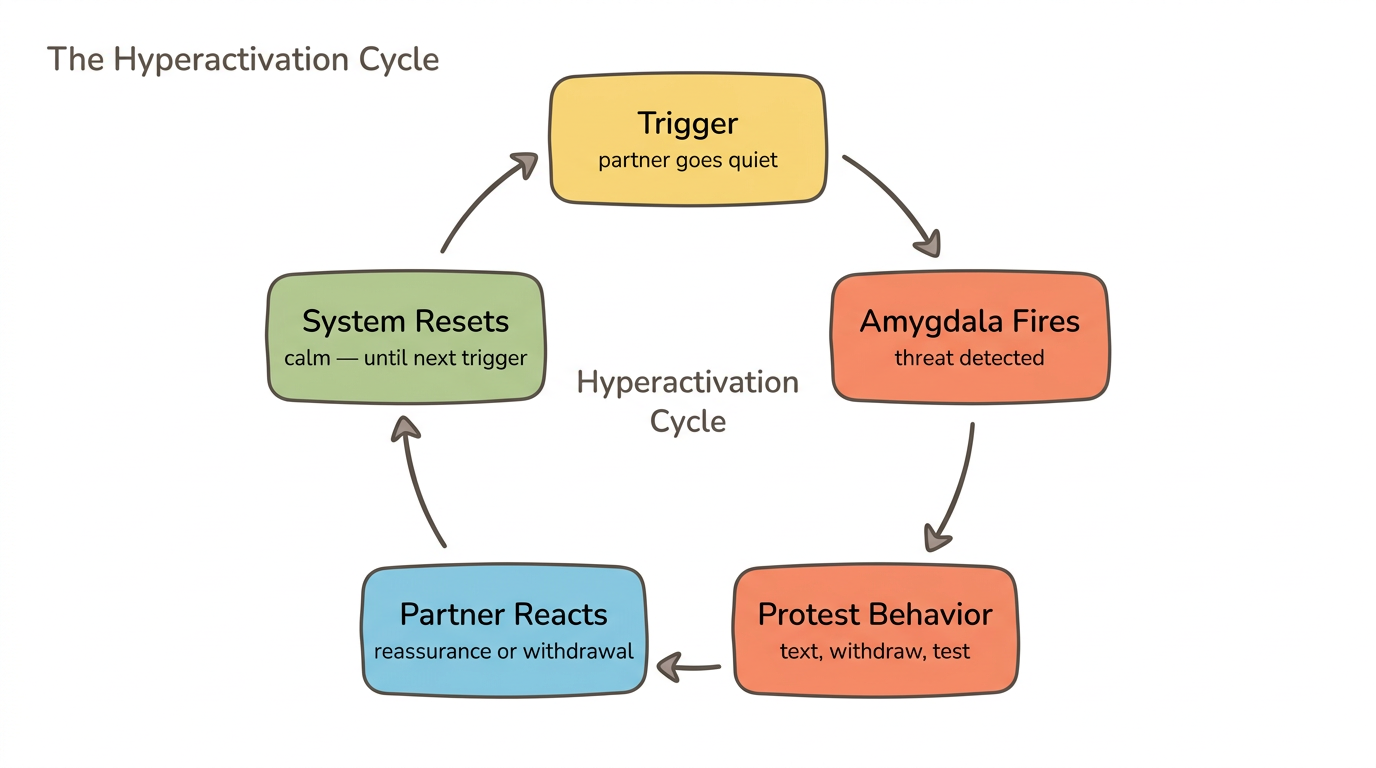
Here are the most common protest behaviors in anxious attachment:
- Excessive calling or texting — reaching out repeatedly when a partner does not respond, driven by escalating activation rather than genuine new information to share
- When your partner goes quiet, you might pull back or go silent yourself — not because you want distance, but to test whether they will pursue you
- Keeping score — tracking who said "I love you" last, who initiated plans, who texted first, building a case file for whether you are valued
- You snap, get short, or pick a fight. The real feeling underneath is fear of disconnection, but what comes out looks like hostility
- Threatening to leave — using the ultimate protest to force reassurance, even when leaving is the last thing you want
- Checking a partner's likes, follows, and online activity becomes a compulsion — you are searching for evidence, building or dismantling a case about their loyalty
- Seeking reassurance from friends — asking others to interpret your partner's behavior, looking for external confirmation that you are loved
People-pleasing is often an anxious attachment strategy — prioritizing your partner's needs to secure connection rather than expressing your own. If texting silence sends you spiraling, that response makes more sense when you understand it as attachment activation rather than overreaction.
Meta-analytic research paints a clear picture of the impact. Li and Chan (2012) analyzed 73 studies with 21,602 participants and found that both anxiety and avoidance negatively predict relationship quality across cognitive, emotional, and behavioral dimensions. Anxiously attached individuals report 2.5 times higher breakup rates and 3 times greater jealousy compared to securely attached individuals. Candel and Turliuc (2019) found that both the anxious person's own insecurity and their partner's insecurity independently contribute to lower satisfaction.
When an anxiously attached person partners with someone avoidant, a painful cycle often emerges — the anxious person's pursuit triggers the avoidant person's withdrawal, which intensifies the pursuit. Even good news can trigger the anxious system — when things are going well, the anxious mind starts scanning for the inevitable loss.
Protest Behavior Inventory (for anxious attachment)
- Over the next week, notice when you feel an urgent pull to act — text again, check their location, withdraw to test them, ask "are we okay?" for the third time today
- Each time, pause and log four things: the trigger (what happened), the urge (what you want to do), the underlying need (what you actually need — reassurance, closeness, safety), and what you actually did
- At the end of the week, review your log for patterns — do certain triggers repeat? Do certain needs keep going unmet?
- Choose one recurring need and brainstorm one direct, non-protest way to express it
This exercise targets anxious attachment by building awareness of the gap between activated attachment system and actual relational need. When you can name the need underneath the urge, you gain the capacity to meet it differently — this is the first step in interrupting the hyperactivation cycle.
For a deeper dive into recognizing these patterns, see 12 signs of anxious attachment.
What Happens in Your Brain When Anxious Attachment Activates?
Anxious attachment is not just a feeling — it is a measurable neurobiological event. When your attachment system activates, your brain shifts into a threat-detection mode that overwhelms rational processing and floods your body with stress hormones.
Amygdala Hyperreactivity
fMRI studies reveal that anxious attachment correlates with increased left amygdala response to angry faces and social punishment cues. Your brain's threat-detection center fires harder and faster than it does in securely attached individuals. Anxiously attached people detect changes in facial expression earlier than others — a form of hypervigilant emotional processing that served a protective function in childhood but creates suffering in adult relationships.
When social rejection or abandonment cues appear, brain imaging shows increased amygdala activation paired with decreased prefrontal cortex activity. The alarm system overwhelms the regulation system. That feeling of your rational mind going offline during a fight with your partner? There is a neurological basis for it.
The Cortisol Cascade
Your stress response system — the HPA axis — operates differently when you carry anxious attachment. Research shows anxious attachment predicts enhanced cortisol reactivity to psychosocial stress. Even more striking, participants higher in attachment anxiety produced more cortisol over the two days following a stressful lab visit. Anxious attachment functions as a chronic social stressor with ongoing endocrine and immune consequences.
Early adverse experiences can recalibrate the HPA axis itself, altering how the stress system operates into adulthood. The hyperactivating emotional style was forged during inconsistent early caregiving — your body learned to stay in alarm mode because the next disruption could come at any time.
The Oxytocin Deficit
Early life stress may inhibit oxytocin formation, creating a hyperactive, oxytocin-deprived amygdala with poor connection to the prefrontal cortex. Oxytocin normally acts as a brake on the amygdala — it inhibits fear responses, weakens HPA axis activity, and reduces cortisol secretion. In anxious attachment, this regulatory circuit is compromised.
Research confirms that adult attachment representations predict both cortisol and oxytocin responses to stress. Resting-state fMRI studies have identified attachment-related neural signatures even outside of active social tasks — the anxious brain is differently wired at baseline.
The mental health correlates reflect this chronic activation: 2 times the depression risk and 50 percent higher social anxiety scores compared to securely attached individuals. For a full guide to how attachment wires your nervous system, see how attachment style affects your nervous system.
Living in a body wired for chronic threat detection is exhausting — and it makes sense that it is. The crucial takeaway: neuroplasticity means these circuits can change. Your brain built these patterns through repeated experience, and it can rebuild them the same way.
Vagal Brake Reset (somatic technique for anxious activation)
- Notice the moment of attachment activation — racing heart, chest tightness, the urge to check your phone, a knot in your stomach
- Place one hand on your chest, one on your belly
- Exhale slowly for 6 to 8 counts through pursed lips — the longer exhale is what activates the vagus nerve
- On the inhale, breathe into your belly for 4 counts
- Repeat for 5 cycles
- After the final exhale, ask yourself: has the urgency shifted even slightly?
This targets anxious attachment by directly engaging the ventral vagal system that chronic hyperactivation has suppressed. Porges's polyvagal theory identifies the vagus nerve as the physiological pathway between social engagement and felt safety — extended-exhale breathing is one of the fastest ways to access it. You are not thinking your way to calm. You are breathing your way there.
What Are the Hidden Strengths of Anxious Attachment?
Your hypervigilance comes at a cost — but it also built a sensitive emotional radar, a capacity for deep empathy, relational attunement, and responsiveness that securely attached individuals sometimes lack.
Your attachment system made you an expert at reading other people. You notice shifts in tone before anyone else in the room. You pick up on a friend's sadness when everyone else misses it. Anxiously attached individuals are 25 percent more responsive to partner bids — those small moments of reaching out for connection that relationship researcher John Gottman identified as the building blocks of intimacy.
Li and Chan's (2012) meta-analysis found something worth sitting with: anxious individuals can still deeply appreciate their relationships when they feel valued by their partner. Unlike avoidant attachment, which suppresses emotional experience entirely, anxious attachment keeps the channel wide open. When the relationship feels secure, that openness becomes a gift — you feel love intensely, connect deeply, and show up fully.
The reframe is not about pretending the pain does not exist. It is about recognizing that your emotional attunement is a superpower when regulated. The goal is not to eliminate your sensitivity but to pair it with the self-regulation skills that let you use it intentionally rather than being overwhelmed by it.
When you can notice a shift in your partner's mood without immediately spiraling into "they're going to leave me," your emotional radar becomes one of the most valuable relational tools there is.
Strengths Reframe Journal (for anxious attachment)
- At the end of each day for one week, list 3 moments when your sensitivity served you well — you noticed a friend was struggling before anyone else, anticipated a partner's need, felt deeply moved by music or connection
- For each moment, complete this sentence: "My attachment system gave me this gift: ___"
- At the end of the week, read all 21 entries together
- Notice what emerges: the depth you carry is not separate from the difficulty — they share a root
This exercise targets anxious attachment by directly counteracting the negative self-model at its core. Bartholomew and Horowitz (1991) identified negative self-image as the defining feature of preoccupied attachment — this journal builds concrete evidence against that model, one entry at a time.
How Does Anxious Attachment Differ From an Anxiety Disorder?
Anxious attachment is a relational pattern triggered by attachment-specific threats, while generalized anxiety disorder and panic disorder are clinical conditions with broader, more pervasive triggers. They can co-occur, but they are fundamentally different in their origins, expression, and treatment.
Here are the key differences:
| Dimension | Anxious Attachment | Anxiety Disorder (GAD/Panic) |
|---|---|---|
| Trigger | Attachment-specific: perceived rejection, abandonment, partner distance | Broad: health, work, finances, safety, social evaluation |
| Context | Primarily activated in close relationships | Present across multiple life domains |
| Onset | Relational — activates when attachment system is threatened | Can be situational or chronic without a relational trigger |
| Treatment | EFT, attachment-focused therapy, relational repair | CBT, medication, exposure therapy |
| Diagnostic status | Not a clinical diagnosis — a personality/relational pattern | DSM-5 clinical diagnosis with specific criteria |
The overlap is real. Anxious attachment correlates with 2 times the depression risk, 2.8 times higher suicidal ideation, and 50 percent higher social anxiety scores. Research on CBT and attachment moderation shows that attachment anxiety often improves during successful anxiety treatment — suggesting the two share underlying mechanisms even when they differ in scope.
A practical way to distinguish them: if your anxiety spikes specifically when your partner goes quiet, when a friend cancels plans, or when you sense emotional distance — but you feel relatively calm at work or during solo activities — you are likely experiencing attachment activation, not generalized anxiety. If anxiety pervades most areas of your life regardless of relational context, a clinical evaluation may be warranted.
Recognizing this distinction matters because the treatment paths differ. If you also recognize both anxious and avoidant patterns in yourself, you may be dealing with disorganized attachment — a pattern that alternates between hyperactivation and shutdown.
What Therapy Works Best for Anxious Attachment?
Emotionally Focused Therapy (EFT) has the strongest evidence base for treating attachment-related relationship distress, with meta-analytic effect sizes that surpass any other couples intervention. Anxiously attached individuals also tend to respond well to individual therapy — and they are more likely to seek it.
Emotionally Focused Therapy
Johnson and colleagues' (1999) meta-analysis found EFT produced an effect size of d = 1.31 — larger than any other couple intervention measured at the time. Beasley and Ager's (2019) meta-analysis of 9 randomized controlled trials over 19 years found an even more striking Hedges's g of 2.09. EFT works by helping partners identify and express the vulnerable emotions underneath their protest behaviors — transforming "Why didn't you text me back?" into "I got scared that I don't matter to you."
Follow-up data shows that decreases in attachment avoidance during EFT are the strongest predictor of relationship satisfaction at follow-up. For anxiously attached individuals, EFT provides the experience of hyperactivation meeting co-regulation — your distress is received rather than dismissed.
Cognitive-Behavioral Therapy
Research shows that anxiously attached adults benefit significantly from CBT, with attachment anxiety tending to improve during successful anxiety treatment. Here is one of anxious attachment's hidden strengths in action: anxious individuals seek help more readily, admit distress more openly, and show stronger treatment compliance compared to avoidant individuals. The drive to pursue connection — the same impulse behind reassurance-seeking — also propels you toward the therapist's office. And that willingness matters.
Combined and Polyvagal Approaches
Combined Attachment-Based Family Therapy and CBT protocols (16 sessions) have shown improvements in both anxiety and family functioning. Polyvagal-informed approaches, drawing on Porges's three-tier nervous system model, help clients understand their symptoms as adaptive autonomic expressions rather than cognitive or emotional failures. Dana's clinical framework teaches anxiously attached individuals to recognize when they have shifted from ventral vagal (social engagement) into sympathetic activation (fight or flight) — and to use that recognition as a cue for co-regulation rather than protest.
Security Priming Visualization (for anxious attachment)
- Close your eyes and bring to mind someone who has consistently made you feel safe and accepted — a therapist, friend, grandparent, teacher, or even a fictional character
- Visualize their face in detail — notice the expression in their eyes, recall the sound of their voice
- Remember a specific moment of warmth with this person — where were you? What did they say or do?
- Notice what happens in your body — where does the tension soften? Does your breathing slow?
- Stay with this image for 2 minutes, returning to the specific sensory details whenever your mind wanders
This targets anxious attachment by activating the internal working model of a secure base. Research on security priming shows that mentally engaging with secure attachment representations reduces hyperactivation even in single sessions — your nervous system responds to imagined safety as well as real safety. Practice daily to gradually build a more accessible internal secure base.
For a full roadmap toward earned security, see how to develop secure attachment as an adult.
How Can You Move Toward Earned Security?
Earned security is the process of developing a secure attachment style through corrective emotional experiences — repeated moments where your nervous system learns a new story about relationships. It is real, evidence-based, and available to you regardless of where you started.
Your nervous system did not learn anxious attachment overnight, and it will not unlearn it overnight either. You do not rewire attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often. Change is gradual and nonlinear — there will be days when old patterns show up with full force, and that does not mean you have failed.
Three pathways support the shift toward earned security:
1. The therapeutic relationship. A consistent, attuned therapist provides what may have been missing in early caregiving — reliable responsiveness. Over time, this relationship becomes internalized as a new template. EFT follow-up data confirms that greater emotional processing during therapy predicts lasting symptom decreases.
Research confirms attachment styles can and do shift in the context of secure relationships — and a secure romantic partner is the second pathway. When a partner consistently responds to your bids for connection without defensiveness or withdrawal, your nervous system gradually recalibrates its threat assessment. The relationship itself becomes therapy.
3. Self-directed practice. Security priming, journaling, somatic regulation, and learning to express needs directly instead of through protest all contribute to the shift. These practices do not replace relational healing, but they build the internal resources that make secure relating possible.
What therapists call earned secure attachment does not mean you will never feel anxious again. It means you will recognize activation faster, soothe yourself more effectively, and choose your response rather than being hijacked by it.
The Pause Protocol (adapted from Levine and Heller, for anxious attachment)
- When you feel the urge to engage in a protest behavior — text again, check their social media, withdraw to test them — name it aloud or internally: "My attachment system just activated"
- Set a timer for 10 minutes
- During the pause, do 5 cycles of extended-exhale breathing (4 counts in, 6 to 8 counts out)
- When the timer goes off, ask yourself: "What do I actually need right now?"
- Choose one direct, non-protest way to meet that need — send a vulnerable text ("I'm feeling disconnected and would love to hear from you"), call a friend, journal about the feeling, or simply acknowledge the need and let it be
This targets anxious attachment by inserting a gap between activation and action — the core mechanism of moving from reactive to reflective responding. The 10-minute window is not arbitrary: it allows the initial cortisol spike to begin subsiding while the breathing activates your vagal brake. Over time, this gap widens naturally.
For 10 specific self-soothing techniques designed for anxious activation, see how to self-soothe anxious attachment.
Anxious Attachment vs. Secure Attachment in Relationships
| Dimension | Anxious Attachment | Secure Attachment |
|---|---|---|
| Core belief | "I'm not enough; they might leave" | "I'm worthy; we can work through this" |
| Self-model | Negative | Positive |
| Response to conflict | Pursue, escalate, protest behaviors | Engage, repair, stay regulated |
| Response to distance | Panic, hyperactivate, seek reassurance | Tolerate, trust, self-soothe |
| Emotion regulation | Amplify negative emotions to signal need | Flexible regulation, express directly |
| Nervous system state | Chronic sympathetic activation | Ventral vagal access with flexible shifting |
| Strength | Deep empathy, emotional attunement | Balanced responsiveness |
| Growth edge | Learning to self-soothe before seeking | Staying attuned to partner's bids |
When Should You Seek Professional Help?
Self-help has real limits, and recognizing when you need support is not a weakness — for anxiously attached individuals, asking for help is actually one of your strengths. Your willingness to reach out, to name your distress, and to seek connection is the same quality that makes you more likely to benefit from therapy.
Seek professional support when:
- Attachment anxiety co-occurs with depression — anxious attachment carries a 2 times higher depression risk, and when both are present, they feed each other in ways that self-regulation alone cannot interrupt
- If you are experiencing suicidal ideation, connect with a professional immediately. Anxiously attached individuals show 2.8 times higher rates of suicidal thinking — this is not something to work through alone
- Protest behaviors are escalating — if checking, monitoring, and testing your partner are increasing rather than decreasing despite your awareness of them
- You understand the cycle intellectually but cannot stop it in the moment. That gap between knowing and doing often signals that your nervous system needs co-regulation from a trained professional, not just information
- Substance use or relationship violence is involved — these require specialized clinical intervention beyond attachment work alone
A therapist trained in EFT, attachment-focused therapy, or polyvagal-informed approaches can provide the consistent, attuned relationship that helps your nervous system learn a new template from the inside out.
Frequently Asked Questions
What is anxious attachment style?
Anxious attachment is a relational pattern where you crave closeness but fear abandonment. It develops from inconsistent early caregiving and shows up as reassurance-seeking, hypervigilance to rejection cues, and difficulty self-soothing when your partner is unavailable. About 19 percent of adults have this style (Hazan and Shaver, 1987).
What causes anxious attachment?
Anxious attachment typically develops from inconsistent caregiving in childhood — a caregiver who was sometimes warm and responsive, sometimes emotionally unavailable. This unpredictability teaches the child that love exists but is not reliable, creating a hyperactivated strategy to maintain closeness.
Can anxious attachment be healed?
Yes. Research on neuroplasticity and earned security shows attachment patterns can shift through therapy — especially Emotionally Focused Therapy, with effect sizes up to 2.09 (Beasley and Ager, 2019). Change is gradual. The attachment system recalibrates through repeated corrective emotional experiences, not a single breakthrough moment.
How does anxious attachment affect relationships?
Anxious attachment drives protest behaviors like excessive texting, reassurance-seeking, and withdrawing to test a partner's response. Both anxiety and avoidance negatively predict relationship quality. Anxiously attached individuals report three times greater jealousy and 2.5 times higher breakup rates compared to securely attached individuals.
Is anxious attachment the same as having an anxiety disorder?
Anxious attachment is a relational pattern triggered specifically by attachment threats like perceived rejection or abandonment. Anxiety disorders such as generalized anxiety disorder involve broader, more pervasive symptoms across multiple life domains. They can co-occur — anxious attachment correlates with 2 times higher depression risk — but they require different treatment approaches.
Do anxiously attached people always attract avoidant partners?
Not always, but the anxious-avoidant pairing is common because both styles' coping strategies reinforce each other. The anxious person's pursuit triggers the avoidant person's withdrawal, which intensifies the anxious person's pursuit. Awareness of this pursuit-withdrawal cycle is the first step toward choosing differently.
What therapy is best for anxious attachment?
Emotionally Focused Therapy has the strongest evidence, with meta-analytic effect sizes of d = 1.31 (Johnson and colleagues, 1999) to g = 2.09 (Beasley and Ager, 2019) for couples. Individual CBT also works well because anxiously attached individuals tend to engage readily in therapy and show strong treatment compliance compared to avoidant individuals.
How do I self-soothe when my anxious attachment activates?
Start with your body: extended-exhale breathing with a 6 to 8 count exhale engages the vagus nerve and shifts your nervous system from fight-or-flight toward calm. Name what is happening — "my attachment system activated" — and pause before acting. Security priming, visualizing someone who makes you feel safe, also reduces hyperactivation.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Foundational Theory
-
Hazan, C., & Shaver, P. (1987). Romantic love conceptualized as an attachment process. Journal of Personality and Social Psychology, 52(3), 511–524.
-
Bartholomew, K., & Horowitz, L. M. (1991). Attachment styles among young adults: A test of a four-category model. Journal of Personality and Social Psychology, 61(2), 226–244.
-
Bowlby, J. Internal working models of attachment. Simply Psychology.
-
Mikulincer, M., & Shaver, P. R. Hyperactivation strategies and emotion regulation in attachment contexts. PMC.
Meta-Analyses and Relationship Quality
-
Li, T., & Chan, D. K. S. (2012). How anxious and avoidant attachment affect romantic relationship quality differently: A meta-analytic review. European Journal of Social Psychology, 42(4), 406–419. (N = 21,602 across 73 studies)
-
Candel, O. S., & Turliuc, M. N. (2019). Insecure attachment and relationship satisfaction: A meta-analysis of actor and partner associations. Personality and Individual Differences, 147, 190–199.
-
Meta-analytic evidence on attachment insecurity and positive emotions. PMC, 2023.
Neuroscience
-
Vrtička, P., et al. (2008). Individual attachment style modulates human amygdala and striatum activation during social appraisal. PLOS ONE, 3(8), e2868.
-
Anxiety attachment and enhanced cortisol reactivity to psychosocial stress. PubMed, 2015.
-
Attachment anxiety as chronic social stressor: Cortisol and immune implications over two days post-stress. PMC, 2013.
-
HPA axis recalibration through early adverse experiences. PMC, 2011.
-
Early life stress, oxytocin formation, and amygdala regulation. Frontiers in Human Neuroscience, 2017.
-
Resting-state fMRI and attachment-related neural signatures. BMC Neuroscience, 2021.
-
Adult attachment representations predict cortisol and oxytocin responses to stress. Attachment & Human Development, 2012.
Therapeutic Approaches
-
Johnson, S. M., et al. (1999). Emotionally Focused Therapy: Status and challenges. Clinical Psychology: Science and Practice, 6(1), 67–79. (Effect size d = 1.31)
-
Beasley, C. C., & Ager, R. (2019). Emotionally Focused Therapy: A systematic review of its effectiveness with couples. Journal of Marital and Family Therapy, 45(4), 604–614. (Hedges's g = 2.09)
-
CBT and attachment style as moderator of treatment outcome. PMC, 2016.
-
Combined Attachment-Based Family Therapy and CBT for anxiety. Frontiers in Psychiatry, 2023.
-
Porges, S. W. (1994). Polyvagal theory and the autonomic nervous system hierarchy. PMC, 2022.
-
Dana, D. Polyvagal theory in clinical practice. Polyvagal Institute.
Statistics
- Attachment style statistics and prevalence data. WifiTalents, 2026.
Clinical and Applied Sources
-
Levine, A., & Heller, R. Protest behaviors and attachment. Attachment Project.
-
Anxious attachment and the sensitive emotional radar. Psychology Today, April 2025.
-
Digital-era attachment anxiety and electronic partner surveillance. PMC, 2025.
This article is for educational purposes only and is not a substitute for professional mental health treatment. If you are experiencing significant distress, suicidal thoughts, or relationship crises, please reach out to a licensed mental health professional or contact the 988 Suicide and Crisis Lifeline by calling or texting 988.
