Pushing people away is a well-documented trauma response in which the nervous system treats closeness as danger and activates protective distancing behaviors. Research shows that approximately 25 percent of adults demonstrate avoidant attachment patterns characterized by withdrawal from intimacy (Bakermans-Kranenburg and van IJzendoorn, 2009), while 50 to 66 percent of adults have experienced at least one adverse childhood experience linked to insecure attachment (Struck et al., 2023).
If you recognize yourself in this pattern—wanting connection but reflexively building walls—you are not dealing with a character flaw. Pushing people away is not one single behavior. It operates through at least five distinct mechanisms, each with different body sensations, triggers, and paths toward healing. What follows is a map for understanding which version of pushing away your nervous system has learned, and what you can do about it.
Key takeaway: Yes, pushing people away is a well-documented trauma response that operates through at least five distinct mechanisms, including nervous system shutdown, deactivating attachment strategies, and hyper-independence. Approximately 25 percent of adults use avoidant strategies, and 50 to 66 percent have experienced at least one adverse childhood experience. Understanding which mechanism drives your withdrawal is the first step toward reconnection.
What Does It Actually Mean to Push People Away?
Pushing people away refers to any pattern of behavior—conscious or unconscious—that creates emotional or physical distance when closeness becomes possible. It ranges from subtle emotional withdrawal like deflecting vulnerable conversations and "forgetting" to reply to messages, to overt distancing like picking fights before a relationship deepens, ghosting, or declaring "I don't need anyone."
What makes this pattern so confusing is that much of it is unconscious pushing away. You may not realize you are doing it until the person is already gone. Van der Kolk (2014) writes that "the terror and isolation at the core of trauma literally reshape both brain and body"—meaning the impulse to distance often lives below conscious awareness, operating through your nervous system rather than your rational mind.
The behavior itself is a protective strategy. At some point, your system learned that closeness carried risk—rejection, engulfment, unpredictability, or pain. Pulling away reduced that risk. The strategy worked. It kept you safe during a time when you had no other options. You can hold both truths—that the strategy protected you and that it may no longer serve you—without needing to resolve the tension right away.
The Distance Inventory (for all attachment styles) Check which of these you recognize in yourself:
- You change the subject when conversations get personal
- You find reasons to criticize partners when things feel close
- You feel the urge to leave or "need space" after moments of tenderness
- You keep backup plans so you never fully depend on one person
- You wait longer to reply to messages as a relationship deepens
- You emphasize independence and self-sufficiency to the point of refusing help
- You withdraw emotionally after conflict instead of repairing
- You feel safer being needed than being known
No score to calculate—just notice which ones land. Self-awareness is the foundation of every change that follows. If you recognized yourself in multiple items, explore whether you might have avoidant attachment patterns.
What Are the Five Ways Trauma Makes You Push People Away?
Trauma drives distancing behavior through at least five distinct mechanisms, each involving different nervous system states, body sensations, and emotional experiences. Recognizing which one (or which combination) applies to you determines what kind of support will actually help.
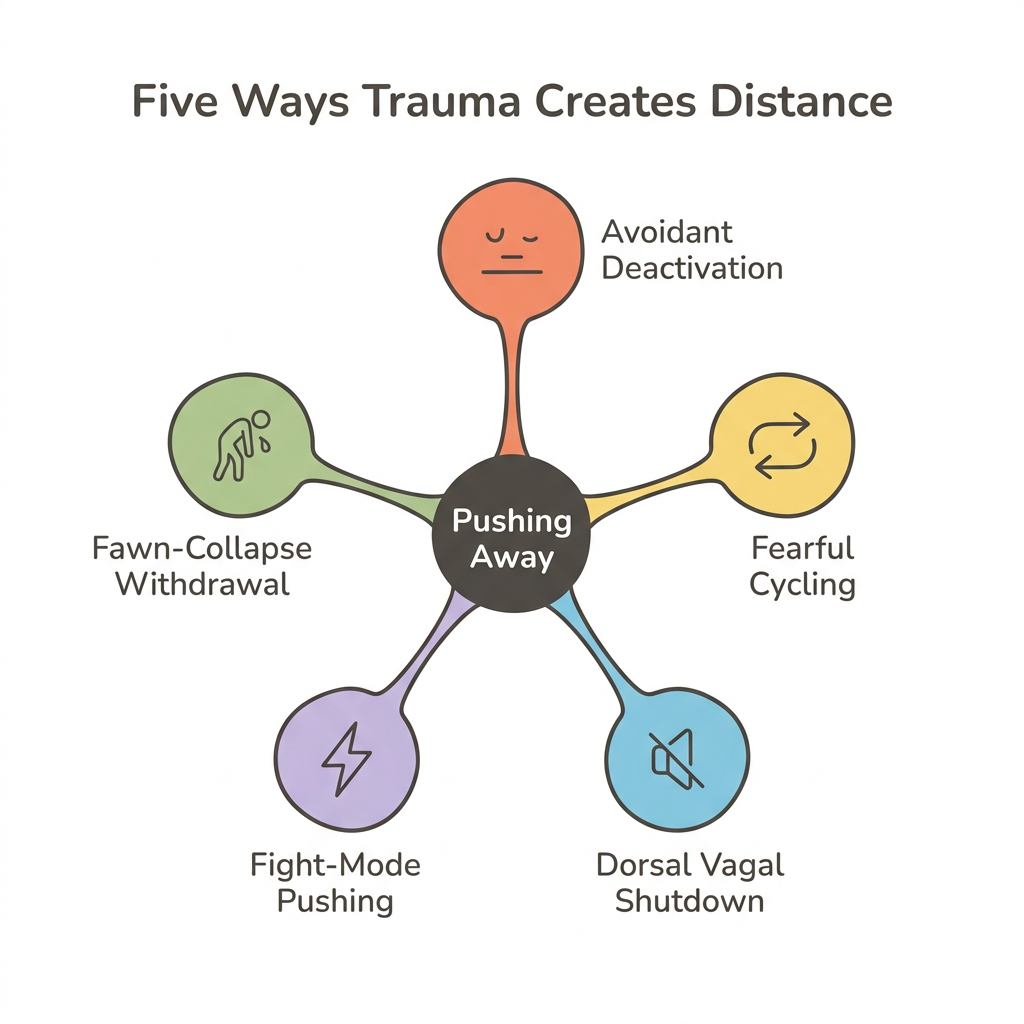
1. Avoidant Deactivation
When caregivers were consistently unresponsive to attachment needs, the child's nervous system learns to suppress those needs entirely. Mikulincer and Shaver (2003) describe these deactivating strategies as cognitive and emotional maneuvers that keep the attachment system turned down—minimizing distress, avoiding closeness, and maintaining compulsive self-reliance.
The experience is deceptively quiet. You feel calm, maybe genuinely indifferent to closeness, and might tell yourself "I'm fine" with full sincerity. Meanwhile your chest stays numb, your breathing runs shallow, and an emotional flatness settles over everything—your body holding the stress your mind refuses to register.
2. Fearful-Avoidant Approach-Avoidance Cycling
Disorganized attachment creates an approach-avoidance conflict where you simultaneously crave and fear intimacy. Research describes this as "the desire of closeness but at the same time the terror and control of it" (Scognamiglio et al., 2024). You pull someone close, then panic and push them away when closeness activates trauma-based fear. If this pattern feels familiar, you may recognize it more deeply in why you push people away when you want them close.
It feels like whiplash between longing and terror—wanting someone desperately one hour and needing to escape the next. Your heart races, then suddenly shifts into numbness or shutdown, the body toggling between two states it cannot reconcile.
3. Dorsal Vagal Shutdown
You are sitting across from someone who cares about you, and your mind goes completely blank. You cannot find words. You cannot feel anything. It is as if someone pulled the plug. Polyvagal theory (Porges, 2011) describes how severe trauma can lock the nervous system into dorsal vagal shutdown—a state of immobilization characterized by dissociation, numbness, and social withdrawal. In this state, you literally cannot access the ventral vagal social engagement system. Pushing people away is not a choice—it is a neurobiological state. Your nervous system's response patterns shape how you experience closeness at a fundamental level. The body feels heavy, fogged, collapsed—limbs like lead, the world muffled behind glass.
4. Fight-Mode Pushing
Sometimes the distance-maker is anger. When closeness triggers a sympathetic nervous system response, irritability and criticism become the wall that keeps people out. The fight-mode pushing pattern creates conflict as a way to restore the sense of control and autonomy that vulnerability threatens. Your jaw clenches, heat rises in your chest, muscles tighten—and before you know it, you have said something sharp enough to guarantee space. The irritation seems to come from nowhere, but it carries a clear message: get away from me.
5. Fawn-Collapse Withdrawal
This mechanism connects directly to people-pleasing as a trauma response. After extended periods of over-giving and self-abandonment, the nervous system collapses into fawn-collapse withdrawal—a state of resentment, depletion, and total retreat. You gave everything, received little, and now your system has nothing left. The path out of people-pleasing often involves learning to set boundaries before the collapse happens.
Feels like: Resentment, exhaustion, "I give and give and no one cares." Body: Bone-deep fatigue, heaviness, wanting to disappear.
Is It Trauma or Is It Attachment—Does the Difference Matter?
Pushing people away can be a direct trauma response, a learned attachment pattern, or—most commonly—both. The distinction matters because it shapes what kind of healing will be most effective. Pushing people away can stem from abuse, neglect, or overwhelming experiences. It can also be a learned attachment pattern from sub-traumatic caregiving—parents who were not abusive but were emotionally unavailable, unpredictable, or dismissive of emotional needs.
Research on adverse childhood experiences shows that 50 to 66 percent of adults have experienced at least one ACE (Struck et al., 2023), and attachment researchers describe a spectrum from "attachment-informed relational patterns" to full "attachment trauma" (Scognamiglio et al., 2024). The line between them is not always clear, and both are valid reasons for pushing people away.
Why does this matter practically? Pure attachment patterns—learned through consistent but non-traumatic caregiving—often respond well to new relational experiences: a secure partner, a close friendship, a therapeutic relationship that offers what was missing. Trauma-based patterns frequently need body-level processing in addition to relational repair, because the trauma lives in the nervous system, not just in relational expectations.
Your nervous system learned to protect you based on the information it had. Whether that information came from a traumatic event or years of emotional absence, the protective response was intelligent. You do not need to decide if your experience was "bad enough" to count.
"Tracing the Origin" Journal Exercise (for all attachment styles)
Your nervous system learned to push people away somewhere. This reflection builds the self-understanding that research links to earned security. Sit with these three prompts for five minutes each:
- "When did I first learn that needing people was unsafe?"
- "What happened when I showed vulnerability as a child—was it met, ignored, or punished?"
- "Does my pushing away feel more like a habit I barely notice (attachment pattern) or an alarm that takes over my body (trauma response)?"
There is no wrong answer. The point is not to diagnose yourself but to build reflective awareness—the capacity to observe your own patterns with curiosity rather than judgment. This reflective functioning is one of the strongest predictors of attachment security shifting over time.
What Happens in Your Body When You Push Someone Away?
Your body responds to closeness as a threat when early experiences wired your nervous system to associate intimacy with danger. This is not metaphorical—it is measurable in brain scans, stress hormones, and autonomic nervous system activity.
The window of tolerance (Siegel, 1999) describes the zone of arousal where you can engage with emotions and other people without becoming overwhelmed or shutting down. Trauma narrows this window. Intimacy that would feel manageable for someone with a wider window pushes you into hyperarousal (panic, anxiety, fight) or hypoarousal (numbness, dissociation, collapse). Pulling away is your nervous system's attempt to get back inside the window.
One of the most revealing findings in attachment neuroscience is the cortisol-subjective dissociation found in avoidant attachment. fMRI studies show that avoidantly attached individuals demonstrate increased prefrontal cortex activation and blunted amygdala reactivity to social-emotional stimuli (DeWall et al., 2012). In plain terms: your body is stressed even when your mind says "I'm fine." The prefrontal cortex is working overtime to suppress the amygdala's distress signals, which shows up as cortisol elevation even while the person reports feeling calm (Ditzen et al., 2008).
Research also reveals that avoidant attachment correlates with reduced striatum and VTA activation in response to social rewards like smiling faces (Vrticka et al., 2008). Social connection is literally less rewarding neurally for people with avoidant patterns—not because they do not want it, but because their brain's reward circuitry has been dampened by years of suppression.
There is reason for hope in this neuroscience. Studies show that oxytocin specifically reduces avoidant attachment patterns (Verhees et al., 2024), suggesting the system can shift. Your neural wiring is not permanent—it is a learned configuration that can be updated through new experiences of safe connection.
"Body Map of Withdrawal" (somatic exercise for avoidant and disorganized attachment)
Your body knows you are pulling away before your mind does. This exercise builds interoceptive awareness—the ability to notice internal states that deactivating strategies suppress. It works for avoidant attachment because it interrupts the automatic suppression cycle that disconnects you from your own felt experience.
- When you notice yourself pulling away from someone, pause before acting on it
- Scan your body: Where do you feel the withdrawal? Common areas include chest, throat, stomach, and limbs
- Name the quality of the sensation: tight, numb, hot, heavy, buzzing, hollow
- Ask the sensation: "What does this feeling want to do?" Notice if it wants to collapse, run, fight, or freeze
- Stay with the sensation for just 10 seconds without acting on the urge to distance
- Place one hand on the area where you feel it most and take three slow breaths
You are not trying to change the sensation or override the urge. You are building the capacity to notice the activation before it makes the decision for you. Ten seconds of noticing is enough to begin.
How Does Each Attachment Style Push People Away Differently?
Each attachment style pushes people away through a different mechanism, driven by different fears and different nervous system states. Mikulincer and Shaver (2003) distinguish between deactivating strategies (avoidant) and hyperactivating strategies (anxious)—but both can result in distance, just through opposite routes.
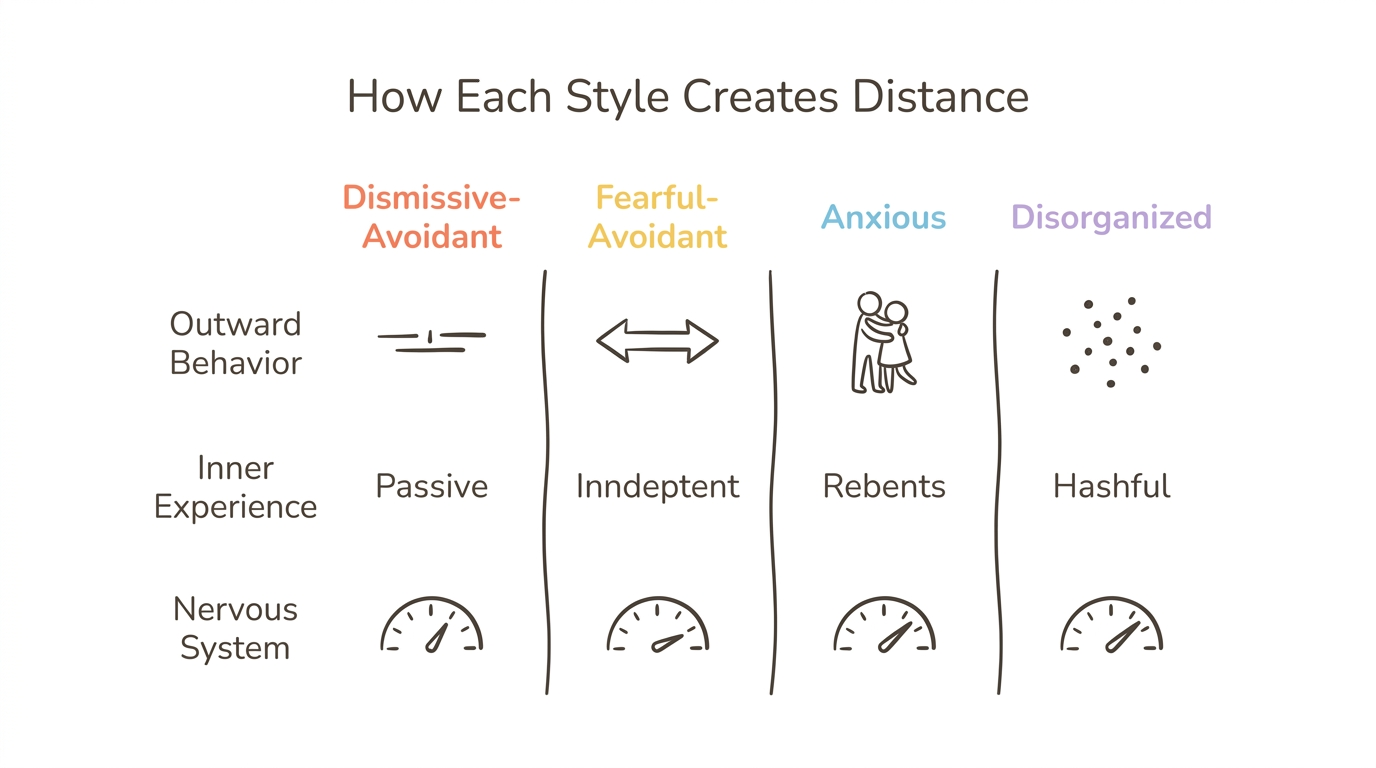
The dismissive-avoidant style creates distance through deactivation—emotional suppression, withdrawal into self-sufficiency, and minimizing the importance of relationships. The fearful-avoidant style generates a more chaotic pattern: hot-cold cycling, testing behaviors, and the exhausting "come here, go away" dynamic. Research shows that approximately 23.5 percent of children demonstrate disorganized attachment patterns (Bernier and Meins, 2023)—the style most directly linked to pushing away while desperately wanting closeness.
What surprises many people is that anxious attachment also pushes people away—through protest behaviors that paradoxically create the rejection they fear. Excessive reassurance-seeking, accusations, and emotional intensity can overwhelm partners into withdrawing, confirming the anxious person's belief that they are "too much." If you recognize this pattern, self-soothing techniques for anxious attachment can interrupt the cycle before protest behaviors escalate.
| Dismissive-Avoidant | Fearful-Avoidant | Anxious | Disorganized | |
|---|---|---|---|---|
| How it looks | Emotional flatness, "I need space" | Hot-cold cycling, come here then go away | Protest behaviors, clinginess that overwhelms | Unpredictable oscillation, dissociative shutdown |
| What it feels like inside | "I'm fine, I don't need anyone" | "I want you close but I'm terrified" | "Why don't you love me enough?" | Confusion, fragmentation, blankness |
| Body sensation | Numbness, chest tightness | Rapid heartbeat shifting to shutdown | Racing heart, stomach knots | Alternating freeze and flood |
| Underlying fear | Engulfment, loss of autonomy | Both abandonment and engulfment | Abandonment, being unlovable | Closeness equals danger because the caregiver was the threat |
| Nervous system state | Dorsal vagal dissociation | Oscillating between sympathetic and dorsal vagal | Sympathetic hyperactivation | Collapsed disorganization |
| Key healing approach | Graduated closeness, EFT | Stabilization and IFS parts work | Self-soothing, differentiation | Start with trauma processing (SE, EMDR) before relational work |
An Internal Family Systems (IFS) lens offers something useful here: each attachment style has a protector part doing its job. The part of you that pushes people away is not your enemy. It developed during a time when distance was the smartest strategy available. Healing does not mean destroying that part—it means helping it update its information.
"Name Your Protector" (IFS-informed exercise for all styles, especially avoidant and disorganized)
This exercise reduces shame by externalizing the pushing-away impulse. Instead of "I'm broken," you shift to "a part of me is trying to protect me"—creating space between the impulse and the action. IFS research shows this separation is one of the mechanisms that helps people with complex trauma reduce reactive patterns.
- Notice when you are about to push someone away—the urge to cancel plans, start a fight, go cold, or shut down
- Instead of acting, say internally: "I notice a part of me wants to create distance right now"
- Ask that part with genuine curiosity: "What are you afraid will happen if I stay close?"
- Listen without judgment. Common answers include: "They'll see the real me," "They'll leave anyway," "I'll lose myself," "It will hurt too much"
- Thank the part for trying to protect you. It learned this role when you needed it
You do not need to override the protector. Just naming it changes the dynamic. You move from being the pattern to observing the pattern—and in that gap, choice becomes possible.
Can You Heal From Pushing People Away?
Yes—and the evidence is specific. Healing from pushing people away does not mean never wanting space again. It means choosing distance vs. being hijacked into it. Several evidence-based approaches directly target withdrawal patterns, and research supports their effectiveness.
Your nervous system learned to treat closeness as danger for reasons that made sense at the time. That learning is real, and it deserves respect. And it can be updated—not through willpower or forcing yourself to be vulnerable, but through graduated exposure to safe connection that teaches your system a new pattern.
Emotionally Focused Therapy (EFT) directly addresses withdrawal as a core pattern. Johnson's model includes a specific change event called withdrawer re-engagement, where avoidant partners learn to express attachment needs instead of shutting down. EFT research demonstrates a 64.5 percent reliable improvement and recovery rate, with attachment avoidance decreasing significantly over the course of treatment. If you are wondering whether avoidant attachment can be healed, the research says yes.
Internal Family Systems (IFS) frames pushing away as a protector part that developed during trauma. Somatic IFS (McConnell) specifically works with the body-level patterns—habitual postures and gestures of pushing away—that maintain distance even when the conscious mind wants closeness.
For the freeze and shutdown responses that underlie social withdrawal, Somatic Experiencing (developed by Peter Levine) works with completing interrupted defensive responses stored in the body. EMDR processes the specific attachment trauma memories that drive avoidant patterns, and the two modalities are often combined when withdrawal has both somatic and memory-based roots.
DBT distress tolerance and interpersonal effectiveness skills build capacity for tolerating the discomfort that closeness brings. Chain analysis can help unpack the sequence of internal events that leads from feeling close to pulling away.
Therapy can change your attachment style—but the therapeutic relationship itself is often the most potent mechanism. You do not rewire attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often.
"Micro-Dose of Closeness" (graduated exposure for avoidant attachment)
Avoidant patterns persist partly because the nervous system never gets the chance to learn that closeness can be safe. This exercise works by providing small, manageable doses of vulnerability—staying slightly past your comfort edge so your system can update its predictions without becoming overwhelmed.
- Identify your current "closeness edge"—the point in interactions where you start wanting to withdraw, check your phone, change the subject, or leave
- This week, choose one interaction and stay 10 percent past that edge. Share one more sentence than feels comfortable. Hold eye contact two seconds longer. Ask one follow-up question instead of redirecting
- Notice what happens in your body as you stay past the edge. Use the Body Map exercise to track the sensations
- After the interaction, place one hand on your chest and take three slow exhales. Tell your nervous system: "I stayed, and I survived"
- Repeat once this week. Not daily—once. Gradual means gradual
You are not trying to become a different person. You are teaching your nervous system that closeness does not always lead to the outcome it expects. One micro-dose at a time is enough.
When Should You Seek Professional Help for Pushing People Away?
Professional support becomes especially important when pushing people away involves dissociation during conflict, an inability to maintain any close relationship over time, or distancing accompanied by flashbacks, nightmares, or chronic emotional numbness that extends beyond relationships. These patterns often indicate C-PTSD—complex trauma from ongoing childhood experiences—which benefits from specialized trauma-informed treatment.
Your nervous system developed these protective strategies when connection was genuinely unsafe. Seeking help is not a sign that you failed at healing on your own. It is recognizing that attachment wounds happened in relationship, and they often heal best in relationship—including the therapeutic one. Van der Kolk (2014) writes: "Being able to feel safe with other people is probably the single most important aspect of mental health." The therapeutic relationship itself is the medicine—a consistent, safe connection where your nervous system can learn that closeness does not have to mean danger.
Research shows that approximately 70.4 percent of people experience trauma in their lifetime, while 3.9 percent develop PTSD (WHO estimates, via PTSD UK). C-PTSD from ongoing relational trauma is not yet a separate DSM diagnosis but is widely recognized clinically and responds to modalities like IFS, Somatic Experiencing, EMDR, and EFT.
Consider reaching out to a trauma-informed therapist if you notice:
- You dissociate, go blank, or cannot remember parts of arguments
- Every close relationship follows the same pattern of distance or destruction
- Physical symptoms like chronic tension, exhaustion, or illness worsen during periods of closeness
- You use substances, overwork, or other numbing behaviors to manage the discomfort of relationships
- You want to change the pattern but feel unable to, even when you understand it intellectually
Developing secure attachment as an adult is possible at any age. The brain remains plastic throughout life, and the attachment system continues to update based on new relational experiences.
Frequently Asked Questions
Is pushing people away a sign of PTSD?
Pushing people away can be a PTSD symptom. The DSM-5 lists emotional numbing, detachment, and social withdrawal under Criterion D. However, it can also stem from insecure attachment without meeting PTSD criteria. If distancing follows flashbacks or nightmares, seek a trauma-informed assessment.
What attachment style pushes people away the most?
Dismissive-avoidant and fearful-avoidant styles both push people away but differently. Dismissive-avoidants withdraw through emotional suppression. Fearful-avoidants cycle between pulling close and pushing away. Anxious attachment can also push people away through protest behaviors that overwhelm partners.
Is isolating yourself a trauma response?
Yes. Isolation can be a dorsal vagal shutdown response where the nervous system enters freeze or collapse mode, making social engagement feel impossible. It can also reflect hyper-independence, where early experiences taught that relying on others leads to harm. Both are protective adaptations to unsafe environments.
Is hyper-independence a trauma response?
Hyper-independence often develops when relying on caregivers led to disappointment, neglect, or harm. The brain learns that self-reliance equals safety. While it looks like strength, it is often a deactivating attachment strategy that prevents the vulnerability required for genuine closeness and co-regulation.
Why do avoidants push you away then come back?
This push-pull pattern reflects the fearful-avoidant style specifically. Distance reduces attachment anxiety, making connection feel safe again, so they return. But closeness reactivates trauma-based fear, triggering another withdrawal. It is not manipulation—it is a nervous system oscillating between craving safety and perceiving danger. Understanding the anxious-avoidant trap can help both partners recognize the cycle.
Can you heal from pushing people away?
Yes. Emotionally Focused Therapy shows a 64.5 percent recovery rate and specifically targets withdrawal patterns. Healing involves building nervous system tolerance for closeness through graduated exposure, processing underlying attachment trauma, and learning to recognize protective parts without being controlled by them.
What to do when someone with PTSD pushes you away?
Do not chase or demand closeness, as this confirms their nervous system's threat detection. Communicate consistent availability without pressure: "I'm here when you're ready." Regulate your own nervous system first. Learn their specific withdrawal pattern—shutdown versus anger versus cycling—so you can respond rather than react.
Why do I shut down emotionally in relationships?
Emotional shutdown is typically a dorsal vagal response. Your nervous system moves into freeze mode when intimacy exceeds your window of tolerance. This is common in avoidant and disorganized attachment, where early experiences taught that emotional openness leads to rejection, punishment, or overwhelm.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Foundational Works
-
Bowlby, J. (1969). Attachment and Loss: Vol. 1. Attachment. Basic Books.
-
Mikulincer, M. & Shaver, P. R. (2003). The attachment behavioral system in adulthood: Activation, psychodynamics, and interpersonal processes. Advances in Experimental Social Psychology, 35, 53–152.
-
Van der Kolk, B. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Viking.
-
Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. W. W. Norton.
-
Siegel, D. J. (1999). The Developing Mind: How Relationships and the Brain Interact to Shape Who We Are. Guilford Press.
Research Studies
-
Bakermans-Kranenburg, M. J. & van IJzendoorn, M. H. (2009). Associations between attachment and mental health care utilization in a large US sample. Journal of Clinical Psychology. PubMed. https://pubmed.ncbi.nlm.nih.gov/26213376/
-
Bernier, A. & Meins, E. (2023). How many children are securely attached to their parents? Psychology Today. https://www.psychologytoday.com/us/blog/the-asymmetric-brain/202306/how-many-children-are-securely-attached-to-their-parents
-
DeWall, C. N. et al. (2012). Neural responses to rejection and attachment style. Social Cognitive and Affective Neuroscience, 7(2), 184–192. https://academic.oup.com/scan/article/7/2/184/1625374
-
Ditzen, B. et al. (2008). Adult attachment and social support. University of Zurich. https://www.zora.uzh.ch/
-
Struck, N. et al. (2023). ACEs and insecure attachment: Prevalence and associations. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC10099002/
-
Verhees, M. W. F. T. et al. (2024). Neurobiological roots of attachment. Nature Communications Psychology. https://www.nature.com/articles/s44271-024-00147-9
-
Vrticka, P. et al. (2008). Individual attachment style modulates amygdala and striatum activation. PLOS ONE. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0002868
Trauma and C-PTSD
-
Scognamiglio, C. et al. (2024). Toward a definition of attachment trauma. ScienceDirect. https://www.sciencedirect.com/science/article/pii/S2468749924000401
-
Quirke, M. G. (n.d.). Why people with C-PTSD may push others away. Michael G. Quirke, MFT. https://michaelgquirke.com/why-people-with-c-ptsd-may-push-others-away/
-
PACEsConnection. (n.d.). Three CPTSD behaviors that push people away. https://www.pacesconnection.com/blog/three-cptsd-behaviors-that-push-people-away
-
PsychCentral. (n.d.). Hyper-independence and trauma. https://psychcentral.com/health/hyper-independence-trauma
-
PTSD UK. (n.d.). Trauma and PTSD statistics. https://www.ptsduk.org/
Polyvagal and Somatic
-
Porges, S. W. (2022). Polyvagal theory: A science of safety. Frontiers in Integrative Neuroscience. https://pmc.ncbi.nlm.nih.gov/articles/PMC9131189/
-
Kolacz, J. et al. (2024). Polyvagal theory: Current status and clinical applications. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC12302812/
-
International Psychotraumatology (iptrauma.org). Understanding the window of tolerance. https://iptrauma.org/docs/body-of-knowledge-of-psychotraumatology/understanding-the-window-of-tolerance-in-trauma-theory/
Therapeutic Approaches
-
Johnson, S. M. (n.d.). Emotionally Focused Therapy. Wikipedia. https://en.wikipedia.org/wiki/Emotionally_focused_therapy
-
Jorgensen, R. (n.d.). Adapting EFT to partners' attachment styles. https://drrebeccajorgensen.com/
-
IFS Institute. (n.d.). Somatic IFS with Susan McConnell. https://ifs-institute.com/store/304
-
Live Consciously PLLC. (n.d.). Healing complex PTSD with Internal Family Systems. https://www.liveconsciouslypllc.com/healing-complex-ptsd-with-internal-family-system-ifs
-
Palo Alto University. (n.d.). DBT chain analysis for emotional avoidance. https://paloaltou.edu/resources/business-of-practice-blog/how-a-behavioral-therapist-can-adapt-dbt-using-chain-analysis-to-disrupt-emotional-avoidance
-
EMDRIA. (n.d.). EMDR, IFS, and Somatic Experiencing. https://www.emdria.org/magazine/emdr-internal-family-systems-and-somatic-experiencing-the-therapy-team-you-didnt-know-you-needed/
Attachment Strategies
-
ScienceDirect. (n.d.). Deactivating strategy overview. https://www.sciencedirect.com/topics/psychology/deactivating-strategy
-
Psychobiology of attachment and trauma. (2019). PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC6920243/
This article is for educational purposes only and is not a substitute for professional mental health care. If you are experiencing trauma symptoms, dissociation, or persistent difficulty maintaining relationships, please consult a licensed therapist who specializes in trauma and attachment. Crisis support is available through the 988 Suicide and Crisis Lifeline (call or text 988).
