Fearful-avoidant attachment is a relational pattern defined by a negative model of both self and others—the only attachment style where both dimensions are negative (Bartholomew and Horowitz, 1991). Research estimates that approximately 7 percent of the general adult population identifies with this style, though self-report studies in younger adults show rates as high as 25 percent. Fearful-avoidant attachment is distinct from being "just anxious" or "just avoidant"—it combines both strategies into a single, contradictory pattern.
If you recognize yourself in this description, you already know the experience: wanting connection desperately, then feeling terrified the moment it arrives. Main and Hesse (1990) described this as an "irresolvable paradox"—the same person who represents safety also represents danger. Your nervous system learned to reach for closeness and pull away from it simultaneously, and that adaptation made sense given what you faced. What follows covers where fearful-avoidant attachment comes from, how it shows up in your body and relationships, and how healing works.
Key takeaway: Fearful-avoidant attachment, also called disorganized attachment, develops when a caregiver is both the source of safety and fear, creating a push-pull pattern in adult relationships. Affecting approximately seven percent of adults, it involves simultaneously craving and fearing intimacy. Unlike other insecure styles, fearful-avoidant combines both anxious and avoidant strategies. With the right support, earned security is achievable.
How Is Fearful-Avoidant Attachment Different from Other Insecure Styles?
Fearful-avoidant attachment is the only style built on a negative model of both self and others, which is what creates the distinctive push-pull pattern that separates it from anxious or dismissive-avoidant attachment. Bartholomew and Horowitz (1991) mapped attachment styles along two dimensions—how you see yourself and how you see others—producing four categories.
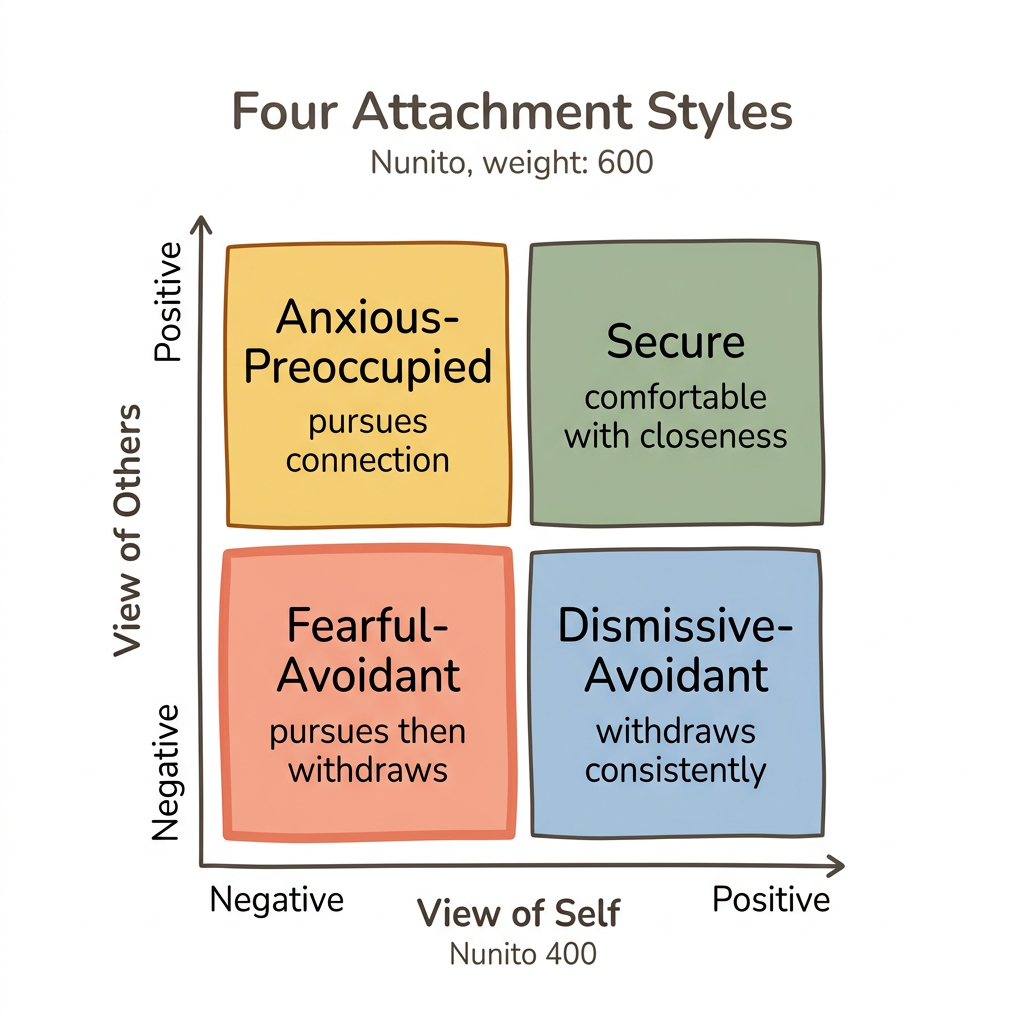
Anxious-preoccupied attachment involves a negative self-model but a positive model of others. The result is pursuit: you believe others can meet your needs, but you doubt your own worthiness. Dismissive-avoidant attachment involves a positive self-model but a negative model of others. The result is withdrawal: you trust yourself but not other people.
Fearful-avoidant attachment holds both models negative. You doubt your own worthiness AND you doubt others' trustworthiness. The result is the pursue-then-withdraw cycle: you reach for connection because you need it, then retreat because you expect it to hurt.
That oscillation is the clearest way to distinguish fearful-avoidant from anxious attachment. Anxious people pursue. They text again, seek reassurance again, protest again. Fearful-avoidant people pursue—then go cold. The withdrawal shocks both the partner and the person doing it.
"Which Voice Is Loudest?" Journal Prompt (for fearful-avoidant self-recognition)
- List 3 recent relationship moments that felt emotionally charged
- For each one, write down your first impulse—did you want to move closer or pull away?
- Note what happened next—did the impulse flip?
- Identify the fear underneath each impulse (rejection? engulfment? being seen?)
- Look for a pattern: if your impulse consistently reversed direction, this points toward the dual-strategy fearful-avoidant pattern rather than a single-strategy style
This exercise works for fearful-avoidant attachment because it makes the oscillation visible. Anxious and avoidant styles show a consistent direction under stress. Fearful-avoidant shows the flip.
What Causes Fearful-Avoidant Attachment?
Fearful-avoidant attachment develops when a caregiver is simultaneously the source of safety and the source of fear—what Main and Hesse (1990) called "frightened or frightening caregiver behavior." The pattern typically takes root in the first 18 months of life, during the window when attachment systems are forming.
Main and Solomon (1986) were the first to identify disorganized attachment as a distinct infant category, observing babies who displayed contradictory behaviors upon reunion with their caregivers—reaching toward a parent while turning their head away, freezing mid-approach, or collapsing to the floor.
The caregiver patterns that produce this response vary. Some involve overt abuse or neglect. Others are subtler: a parent who dissociates during caregiving, a caregiver whose unresolved grief makes them intermittently frightening, a parent who is warm one hour and rageful the next. The common thread is unpredictability in the person who is supposed to be the safe base.
Your nervous system had to solve an impossible problem. The person you needed to run to for safety was the same person your body told you to run from. There was no coherent strategy—no reliable approach or avoidance that worked consistently. So your system learned both, cycling between them.
This framing matters: fearful-avoidant attachment is not a flaw in your character. It is your nervous system's adaptive solution to an irresolvable paradox. And the caregivers who created these conditions were often responding to their own unresolved trauma—not acting out of malice.
"Mapping the Paradox" Reflection (for fearful-avoidant origin understanding)
- Draw two columns on a piece of paper
- Label the left column "Ways my caregiver(s) were a source of safety"
- Label the right column "Ways my caregiver(s) were a source of fear"
- Fill in whatever comes to mind—memories, feelings, body sensations
- Notice if the same person appears in both columns
- Sit with what you notice for 30 seconds without needing to fix or resolve it
This exercise targets fearful-avoidant attachment specifically because it externalizes the paradox that created the pattern. Seeing both realities on paper can reduce the confusion of holding contradictory feelings toward the same person—a confusion your nervous system has been carrying since before you had words for it.
What Does Fearful-Avoidant Attachment Look Like in Relationships?
Fearful-avoidant attachment creates a recurring cycle in relationships: attraction builds, intimacy deepens, fear activates, withdrawal or sabotage follows, then guilt and longing pull you back. This pursue-then-withdraw cycle can repeat for months or years, leaving both partners confused and exhausted.
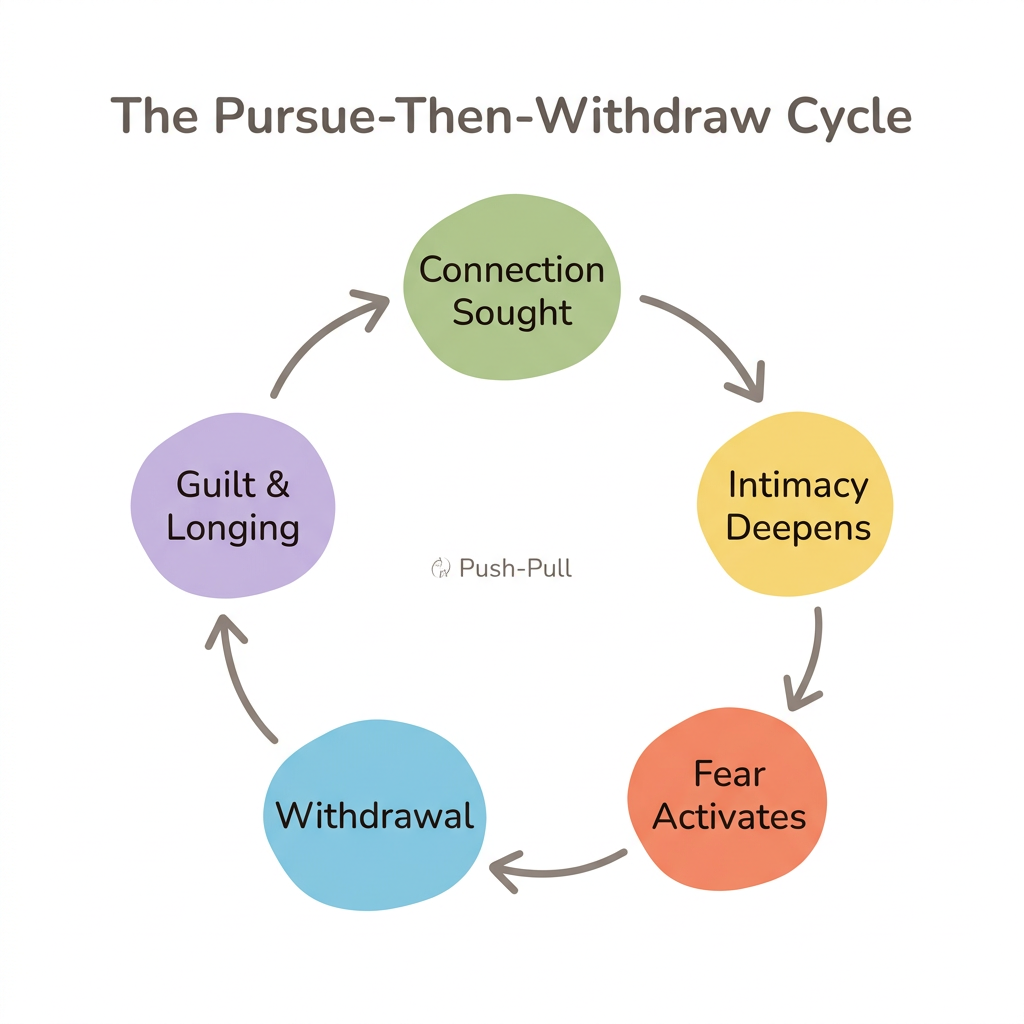
Research from Levy and colleagues (2015) reveals that fearful-avoidant attachment is not one single pattern. Their latent class analysis (N=272) identified two distinct subtypes:
- Disorganized-oscillating: marked by high-affect contradictions—intense emotional swings, dramatic push-pull, preoccupied traits. This subtype scored highest on BPD dimensional measures (M=8.29 versus 0.18–2.5 in other groups).
- Disorganized-impoverished: marked by low-affect flatness—emotional vagueness, difficulty accessing feelings, dismissive traits. This subtype scored highest on avoidant and schizoid measures.
Both are fearful-avoidant. One looks like emotional chaos. The other looks like emotional absence. Recognizing which pattern fits you matters for understanding your specific healing path.
5 Common Fearful-Avoidant Relationship Patterns
- Idealizing partners early, then finding fatal flaws—the initial intensity feels like proof of connection, but as real intimacy approaches, your threat system activates and the flaws become all you can see
- You mistake intensity for intimacy. High-conflict, on-off dynamics feel familiar to your nervous system, while stable relationships can feel "boring" or suspicious precisely because your system doesn't recognize calm as safe
- There's a quiet test running underneath many of your interactions: will they leave if I push hard enough? Pushing away the people you want closest confirms the belief that abandonment is inevitable, even as it breaks your heart
- The morning after a deep conversation. The day after meeting their family. The week after saying "I love you." These moments of genuine vulnerability are often followed by withdrawal—not because the closeness was wrong, but because it activated your threat system
- When a relationship ends, two contradictory feelings arrive at once: relief because the threat is gone, grief because the need for connection remains
"The Push-Pull Timeline" (for fearful-avoidant pattern recognition)
- Think of your last significant relationship (romantic, close friendship, or family)
- Draw a horizontal timeline from beginning to end
- Mark moments you moved toward the person with an upward arrow (vulnerable texts, making plans, expressing affection)
- Mark moments you pulled away with a downward arrow (canceling, going cold, picking a fight, disappearing)
- Look at the sequence: did withdrawal tend to follow closeness?
This exercise addresses fearful-avoidant attachment by making the oscillation pattern concrete and visual. When you can see the cycle on paper, you begin to recognize it as a pattern rather than a series of unrelated events—and pattern recognition is the first step toward choosing differently.
What Happens in Your Nervous System with Fearful-Avoidant Attachment?
Fearful-avoidant attachment produces a unique neurobiological signature: simultaneous fight/flight and freeze activation. Your sympathetic nervous system revs up (racing heart, tight chest, urge to act) while your dorsal vagal system shuts down (numbness, dissociation, collapse)—at the same time. Porges' polyvagal theory describes this as a "blended state" that maps precisely to the subjective experience of wanting to run toward someone and away from them simultaneously.
The Cortisol Paradox
One of the most striking findings in fearful-avoidant research is the cortisol paradox. Kidd and colleagues (2011) measured cortisol output across attachment styles in a sample of 498 adults and found that fearful-avoidant individuals had the lowest cortisol output (409.9 nmol/l) compared to secure (473.0) and dismissive (492.3)—despite reporting the highest subjective stress.
Your body stopped sounding the alarm. Not because you became safe, but because the alarm had been ringing for so long that your HPA axis downregulated—a well-documented response to chronic stress. Separate research found that fearful-avoidant women showed a flattened circadian cortisol rhythm, with no significant difference between morning and evening levels. A healthy pattern shows high morning cortisol dropping to low evening cortisol. A flat pattern signals chronic stress exposure.
Meanwhile, neuroimaging research from Vrtička and colleagues (2012) showed that attachment insecurity alters amygdala reactivity to social cues. Avoidant individuals show increased amygdala activation to negative social scenes; anxious individuals show heightened response to social punishment. Fearful-avoidant individuals—high on both dimensions—may experience both activation patterns simultaneously.
The result is a nervous system that runs on contradictory signals. Your body says danger and your body says freeze. Your mind says reach out and your mind says protect yourself. This is activation, not weakness. Your nervous system is doing exactly what it was trained to do.
"The Pendulation Practice" (somatic exercise for fearful-avoidant nervous system regulation)
- Bring to mind a mild relational stressor—something at a 3 or 4 out of 10, not the most intense thing you can think of
- Notice where you feel it in your body (chest tightness, throat constriction, stomach clenching, numbness)
- Rate the sensation's intensity from 1 to 10
- Now shift your attention to a neutral or pleasant body area—your feet on the floor, your hands resting in your lap, the weight of your back against the chair
- Stay with that neutral sensation for 3 slow breaths
- Gently return your attention to the stress sensation and notice if anything shifted—even slightly
- Repeat this back-and-forth 3 to 4 times
Pendulation specifically addresses the fearful-avoidant nervous system pattern by building your capacity to tolerate activation without dissociating. The simultaneous fight/flight and freeze response makes your system "all or nothing"—you are either overwhelmed or shut down. Pendulation teaches your nervous system that there is a middle ground, gradually widening your window of tolerance.
How Do You Differentiate Fearful-Avoidant from Anxious Attachment?
The clearest differentiator between fearful-avoidant and anxious attachment is what happens after the initial distress: anxious people consistently pursue reassurance, while fearful-avoidant people oscillate between protest and shutdown. Mikulincer and Shaver describe this as using both hyperactivating (anxious) and deactivating (avoidant) emotion regulation strategies, often switching between them unpredictably.
Three key distinctions separate these patterns:
Model of others. Anxious attachment holds a positive model of others—you believe your partner can meet your needs if only you can get them to stay. Fearful-avoidant attachment holds a negative model of both self and others—you doubt your worthiness AND you doubt their trustworthiness.
After conflict. When a fight ends, anxious attachment drives you to seek reassurance—texting, talking, needing to know things are okay. Fearful-avoidant attachment may drive you to dissociate or go cold, then circle back hours or days later carrying guilt and confusion.
Emotional clarity. Mikulincer and Shaver found that fearful-avoidant individuals experience greater "emotional confusion"—difficulty attending to and recognizing their own emotions. Anxious individuals feel their emotions intensely and can usually name them (fear, longing, anger). Fearful-avoidant individuals often cannot tell what they are feeling, or feel contradictory emotions simultaneously.
| Dimension | Fearful-Avoidant | Anxious-Preoccupied | Dismissive-Avoidant |
|---|---|---|---|
| Self-model | Negative | Negative | Positive |
| Other-model | Negative | Positive | Negative |
| Core fear | Both abandonment AND engulfment | Abandonment | Loss of independence |
| Under stress | Oscillates between pursuit and withdrawal | Pursues and protests | Withdraws and deactivates |
| After conflict | May dissociate or go cold, then feel guilt | Seeks reassurance | Distances further |
| Emotion regulation | Both hyperactivating AND deactivating | Hyperactivating | Deactivating |
| Nervous system | Simultaneous fight/flight and freeze | Sympathetic activation | Dorsal vagal shutdown |
| Relationship pattern | Push-pull cycle | Clinging and protest behavior | Emotional distancing |
Can Fearful-Avoidant Attachment Be Healed?
Yes—fearful-avoidant attachment can shift toward what researchers call "earned security": developing a secure attachment orientation despite insecure origins. Your nervous system learned these protective patterns for good reason. They kept you safe when safety was unpredictable. And now, with support, you can teach your system something new.
Healing does not mean erasing the pattern. It means building enough awareness and regulation capacity to catch the cycle earlier and choose differently—10 percent more often, 10 percent sooner. You don't rewire attachment in a single insight. You rewire it by noticing, pausing, and responding differently, repeatedly, over time.
Several therapeutic approaches are particularly effective for fearful-avoidant attachment:
In Emotionally Focused Therapy (EFT), couples learn to see the push-pull cycle not as a character flaw but as a protective strategy driven by unmet attachment needs. The therapist maps the negative interaction cycle, helping both partners locate the fear underneath the behavior—and respond to the fear rather than the defense.
Internal Family Systems (IFS) works with the "parts" system—the protector part that shuts down, the exile carrying childhood pain, the firefighter that acts impulsively. IFS is particularly suited for fearful-avoidant attachment because it validates the internal contradiction. Parts wanting opposite things is not pathology in the IFS framework—it is the expected result of growing up with contradictory caregiving.
The body often knows what happened before the mind can narrate it. Somatic approaches—including somatic experiencing (Peter Levine) and sensorimotor psychotherapy (Janina Fisher)—work directly with that stored experience. Van der Kolk's research emphasizes that trauma is "stored as sensory experience, not as a story." These methods help you notice the chest tightening or throat closing that precedes withdrawal, creating a gap between sensation and reaction.
What does it feel like when your nervous system starts to trust someone? Polyvagal-informed therapy builds toward answering that question by strengthening ventral vagal capacity—your social engagement system—through co-regulation and titrated exposure to relational safety. For fearful-avoidant patterns, this means practicing small doses of connection that your nervous system can tolerate, gradually expanding what feels safe.
The path from fearful-avoidant to earned security involves learning to tolerate the paradox rather than resolving it prematurely. Both the longing and the fear are real. Both make sense given your history. Healing means holding both without either one hijacking your behavior.
"The Approach-Pause-Check" (for fearful-avoidant deactivation interruption)
- Notice when you feel the urge to withdraw from someone you care about—canceling plans, not returning a text, going emotionally flat
- Pause physically: place both feet flat on the floor and feel the contact
- Name the sensation driving the withdrawal—is it fear? Shame? Numbness? Tightness somewhere?
- Ask yourself: "Am I responding to this person, or to an old pattern?"
- Choose one small action toward connection—a brief text, 10 seconds of eye contact, staying in the room for 2 more minutes
This exercise interrupts the automatic deactivation sequence that defines the fearful-avoidant withdraw phase. By inserting a conscious pause between the urge and the action, you build ventral vagal capacity—your nervous system's ability to stay engaged with another person even when activation rises. Over time, these micro-choices teach your system that closeness does not have to mean danger.
When Should You Seek Professional Help for Fearful-Avoidant Attachment?
If you have been reading this article and recognizing yourself in pattern after pattern, you already know how exhausting this cycle is. The push-pull does not just affect your relationships—it affects your relationship with yourself. Living with contradictory impulses day after day takes a toll that is hard to explain to people who have not experienced it.
Self-help builds awareness, but disorganized attachment involves nervous system wiring that often benefits from the co-regulation a trained therapist provides. Your protective patterns developed before you had language. They live in your body, not just your thoughts. A therapist trained in attachment can offer something self-help cannot: a consistent, safe relationship that your nervous system can practice trusting.
Consider seeking help if you recognize several of the following:
- Relationships consistently follow the same push-pull cycle despite your awareness of it—you can see the pattern clearly and still cannot stop it from running
- You experience dissociative episodes during relational stress—going blank, feeling unreal, losing time—and these moments are becoming more frequent or harder to recover from
- Depression, chronic anxiety, PTSD responses, or emotional dysregulation have started interfering with your daily life. Research bears this out: Zhang and colleagues' meta-analysis (2022) of 224 studies and 79,722 participants found that higher attachment anxiety and avoidance were positively correlated with depression, anxiety, and loneliness
- You notice physical symptoms with no clear medical cause—chronic pain, tension, or fatigue that doctors cannot fully explain. Research has linked fearful-avoidant attachment to double the presence of chronic pain compared to secure attachment
- The intensity of your emotional swings feels beyond what you can manage alone. Levy and colleagues (2015) found that the disorganized-oscillating subtype showed the highest association with BPD traits, and fearful-avoidant attachment shows the strongest link to PTSD symptoms among all attachment styles
When looking for a therapist, seek someone trained in EFT, IFS, somatic experiencing, EMDR, or schema therapy—ideally with explicit attachment specialization. Ask potential therapists whether they work with attachment patterns and how they approach disorganized attachment specifically.
This is not a life sentence. Attachment patterns can and do change. The concept of earned security is well-documented in the research literature. The same nervous system that learned to fear closeness can learn—gradually, with support—that connection does not require the same cost it once did.
Frequently Asked Questions
Is fearful-avoidant the same as disorganized attachment?
Fearful-avoidant and disorganized attachment describe the same core pattern at different life stages. "Disorganized" is the infant classification identified by Main and Solomon (1986), observed as contradictory approach-avoidance behaviors. "Fearful-avoidant" is the adult term from Bartholomew and Horowitz (1991), describing the same push-pull dynamic in adult relationships and self-concept.
What is the difference between fearful-avoidant and dismissive-avoidant?
Dismissive-avoidant attachment involves a positive self-image paired with a negative view of others—producing consistent withdrawal as a strategy. Fearful-avoidant attachment involves a negative view of both self and others, producing the oscillation between craving closeness and pushing it away. The key behavioral difference: dismissive-avoidant people withdraw reliably, while fearful-avoidant people pursue then withdraw unpredictably.
What causes fearful-avoidant attachment?
Fearful-avoidant attachment typically develops in the first 18 months of life when a caregiver is simultaneously the source of safety and fear (Main and Hesse, 1990). The infant faces an irresolvable paradox—needing to approach the very person their body tells them to avoid—and develops contradictory strategies as a result.
Can fearful-avoidant attachment be healed?
Research on earned security confirms that attachment patterns can change through therapeutic relationships and consistent practice. Emotionally focused therapy, internal family systems, and somatic approaches show particular effectiveness for fearful-avoidant patterns. Healing is gradual and non-linear—it involves learning to recognize protective patterns and tolerating the discomfort of intimacy in small doses.
What does fearful-avoidant attachment look like in relationships?
Fearful-avoidant attachment creates a recurring push-pull cycle: pursuing connection, then withdrawing when intimacy deepens. Common patterns include idealizing partners early and finding fatal flaws later, testing loyalty through withdrawal, pulling away after moments of genuine vulnerability, and feeling simultaneous relief and grief when relationships end.
How do you know if you're fearful-avoidant or just anxious?
The distinguishing pattern is the flip. Anxious attachment drives consistent pursuit—you seek reassurance and protest distance. Fearful-avoidant attachment drives pursuit followed by sudden withdrawal, going cold or dissociating. If your strategy reverses direction under stress rather than intensifying in one direction, fearful-avoidant is the more likely pattern.
Is fearful-avoidant attachment linked to BPD?
Levy and colleagues (2015) found significant overlap between the disorganized-oscillating subtype of fearful-avoidant attachment and BPD features, with that group scoring highest on BPD dimensional measures (M=8.29 compared to 0.18–2.5 in other attachment groups). However, fearful-avoidant attachment is a relational pattern, not a clinical diagnosis, and many people with this style do not meet criteria for BPD.
What triggers a fearful-avoidant person?
Both too much closeness and too much distance can trigger a fearful-avoidant response. Specific triggers include moments of vulnerability, unreciprocated emotional bids, perceived rejection, unexpected kindness or warmth, and relationship milestones that signal deepening commitment—anything that raises the stakes around intimacy or abandonment.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Foundational Attachment Theory
- Bartholomew, K., & Horowitz, L. M. (1991). Attachment styles among young adults: A test of a four-category model. Journal of Personality and Social Psychology, 61(2), 226–244.
- Main, M., & Solomon, J. (1986). Discovery of an insecure-disorganized/disoriented attachment pattern. In T. B. Brazelton & M. W. Yogman (Eds.), Affective development in infancy (pp. 95–124). Ablex Publishing.
- Main, M., & Hesse, E. (1990). Parents' unresolved traumatic experiences are related to infant disorganized attachment status. In M. T. Greenberg, D. Cicchetti, & E. M. Cummings (Eds.), Attachment in the preschool years (pp. 161–182). University of Chicago Press.
Subtypes and Personality
- Levy, K. N., Johnson, B. N., Clouthier, T. L., Scala, J. W., & Temes, C. M. (2015). An attachment theoretical framework for personality disorders. Canadian Psychology, 56(2), 197–207.
- Mikulincer, M., & Shaver, P. R. (2007). Attachment in adulthood: Structure, dynamics, and change. Guilford Press.
Neuroscience and Physiology
- Kidd, T., Hamer, M., & Steptoe, A. (2011). Examining the association between adult attachment style and cortisol responses to acute stress. Psychoneuroendocrinology, 36(6), 771–779.
- Vrtička, P., Bondolfi, G., Sander, D., & Vuilleumier, P. (2012). The neural substrates of social emotion perception and regulation are modulated by adult attachment style. Social Neuroscience, 7(5), 473–493.
- Pierrehumbert, B., Torrisi, R., Laufer, D., Halfon, O., Ansermet, F., & Beck Popovic, M. (2010). Adult attachment representations predict cortisol and oxytocin responses to stress. Attachment & Human Development, 12(6), 587–601.
- Porges, S. W. (2011). The polyvagal theory: Neurophysiological foundations of emotions, attachment, communication, and self-regulation. W. W. Norton.
Mental Health Associations
- Zhang, T., Fu, H., & Bhatt, G. (2022). Attachment insecurity and mental health: A meta-analysis of 224 studies. Journal of Affective Disorders, 319, 188–199.
Therapeutic Approaches
- Jorgensen, R. (n.d.). Made to measure: Attachment styles in couples therapy. Adapting EFT to attachment styles.
- Van der Kolk, B. A. (2014). The body keeps the score: Brain, mind, and body in the healing of trauma. Viking.
- Fisher, J. (2017). Sensorimotor psychotherapy for attachment-related trauma. In Healing the fragmented selves of trauma survivors (pp. 1–20). Routledge.
- Levy, K. N., Ellison, W. D., Scott, L. N., & Bernecker, S. L. (2011). Attachment style. In J. C. Norcross (Ed.), Psychotherapy relationships that work (2nd ed., pp. 377–401). Oxford University Press.
- Slade, A., & Holmes, J. (2019). Attachment and psychotherapy. American Journal of Psychotherapy, 70(3), 233–251.
This article is for educational purposes only and is not a substitute for professional mental health care. Fearful-avoidant attachment is not a clinical diagnosis. If you recognize these patterns in yourself and they are causing distress, consider working with a licensed therapist who specializes in attachment-informed approaches.
