Nervous system healing from attachment trauma refers to measurable changes in how your autonomic nervous system responds to relational cues — not just feeling calmer, but actual shifts in brain structure, stress hormones, and vagal tone. Approximately 44 percent of US adults have insecure attachment styles, each with a distinct nervous system signature: hyperactivation, deactivation, or rapid state-switching (WifiTalents, 2026).
If you've encountered phrases like "the body keeps the score" and wondered whether your nervous system can actually change — not just cope better — the answer from neuroscience is yes. Neuroplasticity is lifelong, and brain structural changes previously assumed irreversible from complex trauma show evidence of repair with appropriate intervention (Siegel, 2012). This article maps the science of how attachment trauma reshapes your nervous system and the evidence-based pathways that reverse those patterns.
Key takeaway: Yes, you can heal your nervous system from attachment trauma at any age. Attachment trauma encodes as chronic defensive states in your autonomic nervous system, but body-based therapies, safe relationships, and consistent practice produce measurable changes in brain structure, stress hormones, and vagal tone within weeks to months of targeted intervention.
How Does Attachment Trauma Get Stored in the Nervous System?
Attachment trauma doesn't just live in memory — it encodes directly in your autonomic nervous system through altered brain structures, dysregulated stress hormones, and persistent survival responses. Your body learned to protect you long before you had words for what was happening, and those protective patterns became wired into the way your nervous system reads the world.
Porges' Polyvagal Theory describes neuroception — your nervous system's unconscious scanning for safety or danger (Porges, 2011). When early attachment relationships were unpredictable or frightening, neuroception calibrated toward threat detection. Your amygdala became hyperactive. Your HPA axis — the stress hormone system connecting your hypothalamus, pituitary gland, and adrenal glands — began producing cortisol at levels that harm hippocampal function and synaptic plasticity over time (Feldman, 2017).
Feldman's research revealed something fundamental: attachment is a nervous system phenomenon, operating through biobehavioral synchrony — the temporal alignment of brain activity, peripheral physiology, and endocrine responses between attachment partners (Feldman, 2017). When that synchrony was disrupted in childhood, the oxytocin-dopamine crosstalk that normally supports bonding never developed its full architecture.
Van der Kolk's research shows trauma reshapes both brain and body, encoding in persistent autonomic nervous system activation, stress hormone pathways, and sensory-motor circuits (Van der Kolk, 2014). This is why you can logically know you're safe while your body screams otherwise. In one study of pediatric neurology patients, 88 percent of those with multiple medically unexplained symptoms reported at least one adverse childhood experience, compared to 33 percent in controls (Palomba et al., 2017). The body keeps the score — literally.
For a deeper look at how each attachment style shapes your nervous system, see How Does Attachment Style Affect Your Nervous System?.
Body State Check-In (for all attachment styles — builds interoceptive awareness)
- Pause wherever you are and close your eyes if that feels safe
- Scan from head to feet — notice where you feel tension, heaviness, buzzing, or numbness
- Name the sensation without interpreting it (say "tight chest," not "I'm anxious")
- Place one hand on the area that speaks loudest
- Take three slow breaths, directing each exhale toward that spot
This builds interoceptive awareness — your ability to read your body's internal signals. Interoception is foundational to nervous system healing because you cannot regulate what you cannot feel. Start with 30 seconds. That's enough.
What Does a Dysregulated Nervous System Feel Like for Each Attachment Style?
Each insecure attachment style maps to a specific nervous system state, not just a set of thoughts or behaviors. Mikulincer and Shaver's research demonstrates that anxious attachment operates through hyperactivation — chronic intensification of emotion — while avoidant attachment operates through deactivation — suppression of emotional experience (Mikulincer and Shaver, 2024). These are nervous system patterns, not personality flaws.
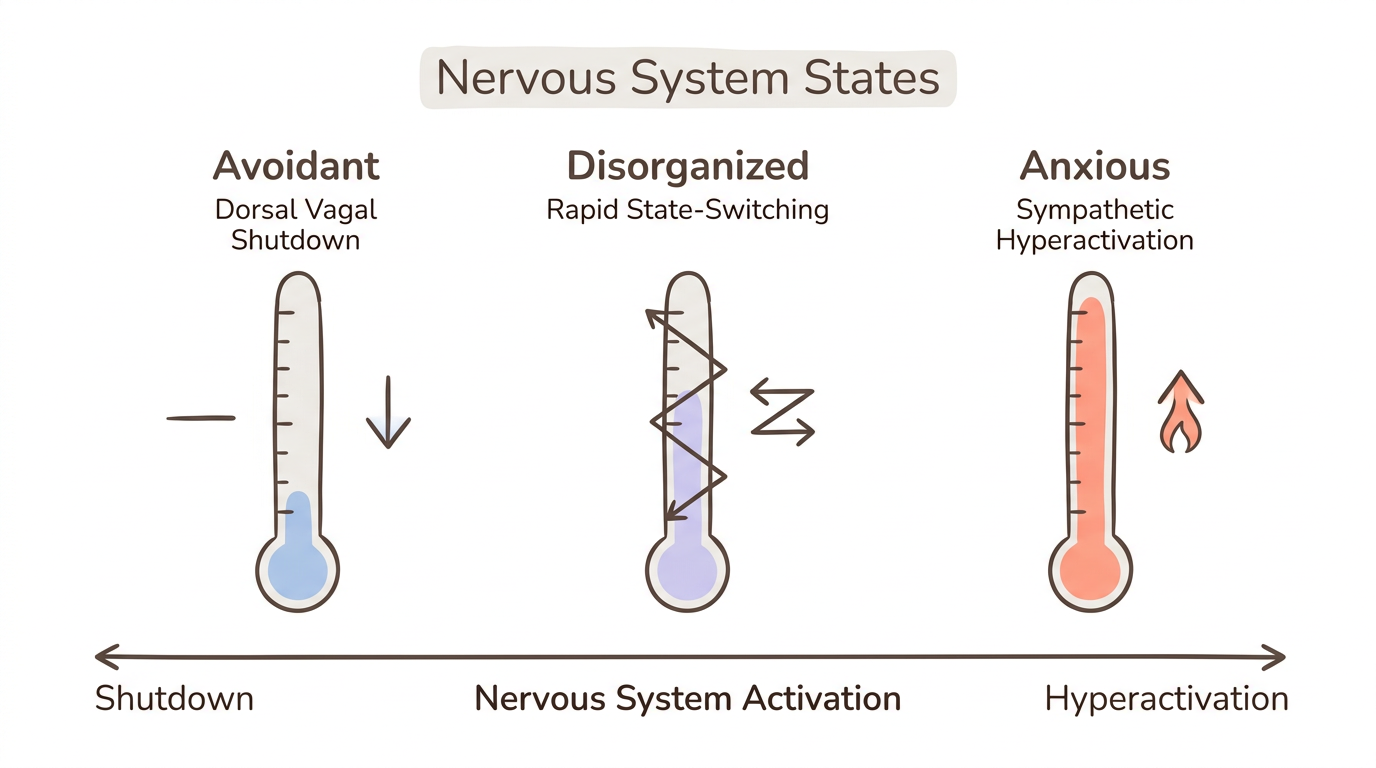
Anxious Attachment: Sympathetic Hyperactivation
Your nervous system stays locked in sympathetic fight-or-flight mode. Racing heart during a partner's silence, hypervigilance for signs of withdrawal, difficulty calming down after conflict — these reflect a system that learned to amplify distress because muted signals went unnoticed in childhood. Your window of tolerance is narrow at the top, meaning you tip into hyperarousal quickly but rarely drop into shutdown. Self-soothing techniques for anxious attachment work because they directly target this sympathetic overdrive.
Avoidant Attachment: Dorsal Vagal Shutdown
Where anxious attachment turns the volume up, avoidant attachment turns it off. Dorsal vagal shutdown manifests as emotional numbness, disconnection from your body, flatness under stress, and a sense of watching your life from behind glass. Your system learned that expressing needs led to rejection, so it automated suppression. You might not feel anxious in relationships — you might not feel much at all. This isn't calm. It's a different kind of dysregulation. Pushing people away often reflects this dorsal vagal pattern rather than genuine preference for distance.
Disorganized Attachment: Rapid State-Switching
The nervous system signature of disorganized attachment is the most destabilizing: rapid oscillation between sympathetic activation and dorsal vagal collapse. fMRI studies show enhanced amygdala activation in unresolved attachment, without the compensatory prefrontal regulation that securely attached individuals develop (Neuroscience Insights, 2023). Intimacy itself becomes the trigger — the person you need for safety is neurologically linked to danger. Your body wants to approach and flee simultaneously, producing freeze states, dissociation, and the fawn response.
| Anxious Attachment | Avoidant Attachment | Disorganized Attachment | |
|---|---|---|---|
| Dominant ANS state | Sympathetic hyperactivation | Dorsal vagal shutdown | Rapid oscillation between states |
| What it feels like | Racing heart, hypervigilance, can't calm down | Emotional numbness, disconnection, flatness | Simultaneous urge to approach and flee, freeze |
| Core nervous system pattern | Hyperactivation — amplifies distress signals | Deactivation — suppresses distress signals | Both — contradictory activation and deactivation |
| Triggered by | Perceived distance or unavailability | Perceived demands for closeness or emotion | Intimacy itself (approach equals danger) |
| Healing focus | Calming sympathetic activation, building self-regulation | Thawing dorsal vagal shutdown, reconnecting to sensation | Stabilizing state-switching, building coherent sense of safety |
| Best-fit body-based approach | Physiological sigh, grounding, slow exhale emphasis | Gentle movement, interoceptive awareness, gradual sensation tolerance | Pendulation (Somatic Experiencing), titrated exposure to body sensation |
Can a Dysregulated Nervous System Actually Be Healed?
Yes — and the evidence goes beyond symptom management to demonstrate actual neural rewiring. Neuroplasticity — the brain's ability to form new connections throughout life — means the structural changes caused by attachment trauma are not permanent sentences (Siegel, 2012). White matter damage, hippocampal volume loss, and amygdala hyperactivation all show evidence of corrective change with targeted intervention.
The distinction matters: regulating in the moment is necessary but not sufficient for lasting change. A breathing exercise calms your sympathetic activation right now. That's valuable. But it doesn't update the implicit memory system that fires your alarm in the first place. Genuine nervous system healing requires three channels working together:
None of these channels had a fair chance to develop when your early environment didn't support them.
- Bottom-up processing — body-based regulation that directly shifts autonomic states. Trauma-sensitive yoga produced PTSD remission in 52 percent of participants versus 21 percent in the control group (Van der Kolk et al., 2014).
- Top-down processing — narrative integration and meaning-making that strengthen prefrontal regulation over limbic reactivity. This is where therapy changes your attachment style.
- New relational experiences — safe relationships that update implicit memory by providing repeated evidence that closeness does not equal danger.
Neurofeedback research demonstrates how concrete this rewiring can be: a meta-analysis found a 79.3 percent PTSD remission rate by directly restoring excitatory-inhibitory balance in the prefrontal cortex, hippocampus, and amygdala (PMC, 2023). The brain doesn't just adapt around trauma — it can structurally reorganize.
Your nervous system learned its current patterns for good reason. Those patterns kept you safe in an environment where they were the best available option. And now, neuroplasticity gives you the capacity to teach it something new — not by overriding those protective responses, but by gradually expanding what your system can tolerate.
Three-Channel Check (self-assessment for all attachment styles) Rate yourself 1–10 in each channel:
- Body regulation — "Can I notice and name what I feel physically right now?"
- Narrative coherence — "Can I tell the story of my childhood without flooding or going blank?"
- Relational safety — "Is there at least one person I can be vulnerable with without bracing for rejection?"
Your lowest score points toward the healing channel that needs the most attention. Avoidant types often score lowest on body regulation — years of deactivation create a disconnect from physical sensation. Anxious types frequently score lowest on relational safety — hyperactivation makes every vulnerability feel like a risk. Disorganized types may score low across all three, which is information, not a verdict.
Why Does Nervous System Healing Require Safe Relationships?
Your nervous system learned its patterns in relationship, and it heals in relationship. This isn't a metaphor — Feldman's research shows that social synchrony interventions directly reduce cortisol and elevate oxytocin, demonstrating that relational experiences alter stress hormones at a biological level (Feldman Lab, 2021). Co-regulation — the process of one nervous system calming another — is the mechanism through which humans first learn to regulate at all.
Think about how infants develop. A baby cannot calm itself. It borrows regulation from a caregiver whose voice, touch, and predictable presence activate the baby's parasympathetic system. Over thousands of repetitions, those externally provided patterns internalize — the baby's brain literally wires itself around the caregiver's regulatory capacity. When early caregiving was inconsistent or frightening, that wiring developed gaps.
Relationships change the brain by providing the same regulatory input that was missing in childhood (Schwartz, 2021). Consistent signals — gentle tone, kind eyes, predictable behavior — activate your parasympathetic system. Over time, your nervous system "borrows" regulation from caring others until those patterns become internalized. This is the co-regulation to self-regulation pathway.
Vagal tone, measured through heart rate variability, serves as a biomarker of this process. Higher vagal tone correlates with better emotion regulation, social engagement, and stress recovery — and attachment security predicts higher vagal tone (Frontiers in Psychology, 2017). As you accumulate co-regulating experiences, your vagal tone measurably improves.
Research also reveals the cost of this pathway being disrupted: adverse childhood experiences lead to insecure attachment, which produces emotion dysregulation strategies, which increase vulnerability to depression (PMC, 2023). The chain runs through the nervous system at every link. Healing that chain means rebuilding what the nervous system missed — and that requires another human being's secure base.
This is why solo breathwork alone doesn't complete the picture. Breathing exercises regulate your state in the moment. Relationships regulate the system that sets your state. Both matter, but they serve different functions. Developing secure attachment as an adult is fundamentally about finding and building these co-regulating connections.
Co-Regulation Inventory (for all attachment styles)
- Identify two to three people whose presence genuinely calms your nervous system — not just people you enjoy, but people your body relaxes around
- Notice what they do that creates safety: their tone, pacing, eye contact, predictability
- Increase your exposure to at least one co-regulating relationship this week — a phone call, a walk, a meal
- Track what you notice in your body before and after contact
For anxious attachment: notice whether you're seeking reassurance (hyperactivation trying to get the other person to regulate your anxiety) versus genuine co-regulation (your system settling in their presence). For avoidant attachment: notice the resistance to letting someone else's calm affect you — that resistance is your deactivation strategy at work, not evidence that you don't need people.
What Are the Most Effective Therapies for Nervous System Healing?
The therapies with the strongest evidence for nervous system healing combine body-based processing with relational safety — addressing both the autonomic patterns encoded by trauma and the relational context in which they formed. Here are the approaches with the most robust research, matched to the attachment-style patterns they best address.
1. Somatic Experiencing (SE)
Developed by Peter Levine, SE uses bottom-up processing to complete the incomplete defensive responses stored in your body. Rather than talking about trauma, SE works with interoceptive and proprioceptive sensations — the felt sense of fight, flight, or freeze that never discharged. A scoping review found large effect sizes for PTSD symptoms (Cohen's d = 0.94–1.26) and depression (d = 0.7–1.08) in RCTs (Brom et al., 2017). Best fit: disorganized attachment, where rapid state-switching requires careful titration between activation and settling. Also effective for avoidant patterns where reconnecting to body sensation is the primary task.
2. EMDR (Eye Movement Desensitization and Reprocessing)
Best fit: anxious attachment, where hyperactivated threat memories drive relational anxiety, and disorganized attachment with clear traumatic origins. WHO, APA, and VA/DoD-recommended as a first-line PTSD treatment, EMDR processes traumatic memory networks through bilateral stimulation. A meta-analysis found an effect size of g = 0.93 for PTSD versus control conditions (Psicothema). Notably, Attachment-Based EMDR shows enhanced outcomes over standard EMDR specifically for attachment-related trauma — greater reductions in both trauma and anxiety symptoms (ScienceDirect, 2025).
3. Internal Family Systems (IFS)
What makes IFS distinctive is how it engages prefrontal cortex regulation over limbic activation through what founder Richard Schwartz calls "Self-energy." A pilot study found 92 percent of completers no longer met PTSD criteria after 16 weeks (N=17; Hodgdon et al., 2021). IFS also enhances interoceptive awareness, which is foundational for tolerating trauma-related sensations. Particularly valuable for disorganized attachment where internal contradictions — protector parts in conflict — mirror the approach-avoid nervous system pattern. Useful across all insecure styles.
4. Trauma-Sensitive Yoga
Avoidant attachment responds especially well to this approach, because gentle, self-directed body movement rebuilds the interoceptive connection that deactivation severed. Van der Kolk's RCT demonstrated that 52 percent of yoga participants no longer met PTSD criteria versus 21 percent of controls after 10 weeks (N=64 women with chronic, treatment-resistant PTSD; Van der Kolk et al., 2014). The mechanisms include improved autonomic regulation (increased HRV, reduced startle), reduced HPA axis activation, and decreased inflammation.
5. Neurofeedback
A meta-analysis found a 79.3 percent PTSD remission rate versus 24.4 percent in control conditions (PMC, 2023). Neurofeedback directly targets prefrontal cortex, hippocampus, and amygdala functioning — restoring the excitatory-inhibitory brain balance that trauma disrupts. Promising specifically for developmental trauma and attachment disruption. Best fit: disorganized attachment with significant dissociative features, where top-down verbal processing may be limited.
6. Polyvagal-Informed Approaches
Vagal toning exercises directly stimulate the ventral vagal social engagement system: the physiological sigh (double inhale through the nose, slow exhale through the mouth), humming or chanting (vibrates the vagus nerve), and co-regulation practices (Porges, 2011). These are complementary rather than standalone — best used daily alongside formal therapy.
What Does Nervous System Healing Look Like Day to Day?
Nervous system healing is not a single breakthrough — it unfolds in three overlapping phases, each with measurable markers that research helps us estimate. Competitors say "it takes time" without specifics. Here is what the evidence actually shows.
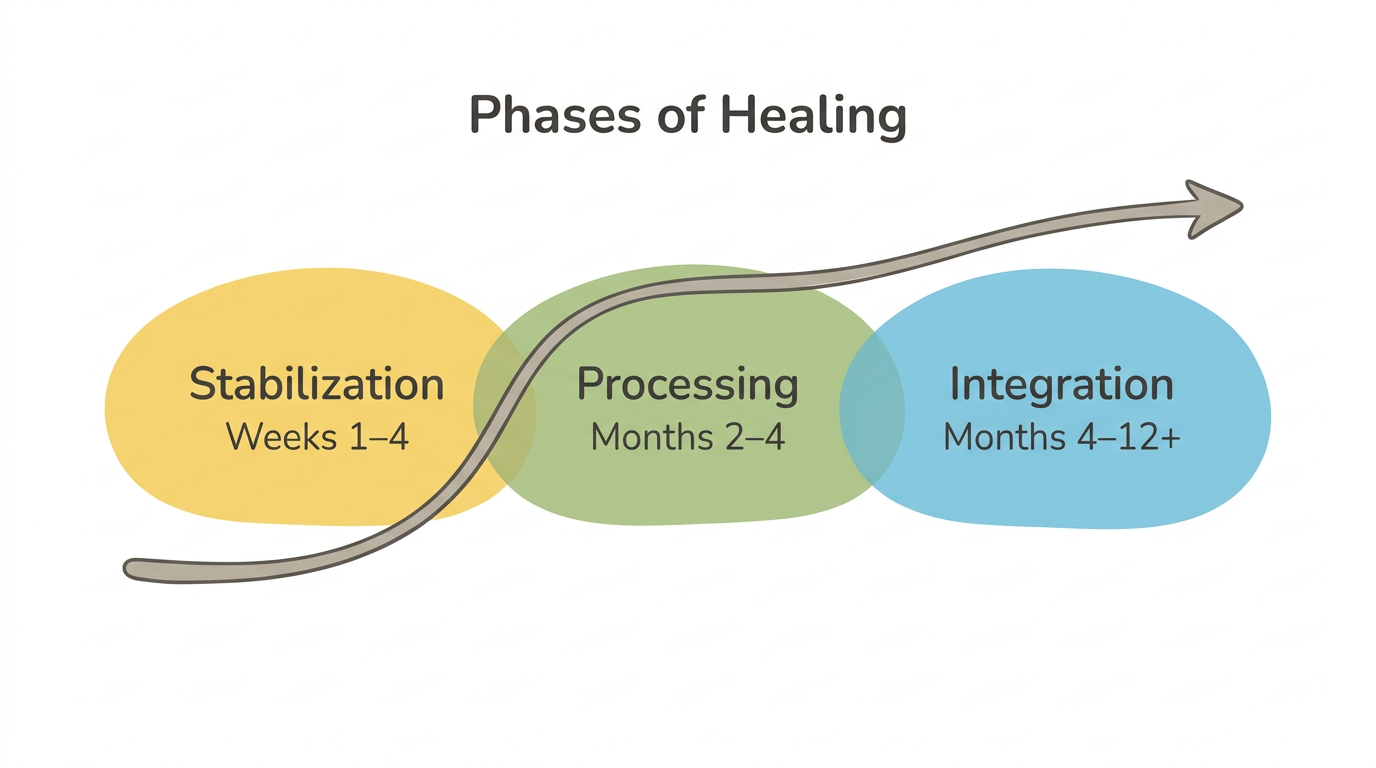
Phase 1: Stabilization (Weeks 1–4)
You learn to notice your nervous system states — recognizing when you've left your window of tolerance rather than realizing hours later. Basic regulation tools begin working: grounding techniques bring you back faster, and you start distinguishing between current danger and old activation. This phase feels effortful. You might notice more distress initially — not because things are getting worse, but because awareness precedes regulation. Your nervous system has been running these programs on autopilot. Noticing them is the first disruption.
Phase 2: Processing (Months 2–4)
The IFS pilot study showed PTSD remission within this timeframe (Hodgdon et al., 2021), and Van der Kolk's yoga RCT achieved 52 percent remission in 10 weeks — evidence that meaningful nervous system change happens in this window. With therapeutic support, traumatic material stored in the body begins to process. Your window of tolerance expands — you can sit with activation longer before tipping into hyperarousal or shutdown. Co-regulation experiences start feeling less threatening. You might notice your body relaxing around safe people without consciously trying to make that happen.
Phase 3: Integration (Months 4–12 and Beyond)
New relational patterns require less effort. Recovery from activation shortens — what once took days might take hours, then minutes. Secure functioning becomes more automatic, though not constant. The path toward earned secure attachment is non-linear. You don't rewire attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often.
Biomarkers of progress you may notice: improved sleep quality, reduced startle response, ability to stay present during conflict rather than dissociating or flooding, less physical tension at baseline, and shorter recovery time after relational triggers. Measurable markers include improved heart rate variability, reduced cortisol reactivity, and — on neuroimaging — restored prefrontal-amygdala connectivity.
Nervous System Progress Journal (somatic tracking for all attachment styles)
- Morning — rate your baseline activation 1–10 and note one body sensation (for example, "6 — shoulders tight, stomach clenched")
- Evening — note your highest activation moment, what triggered it, and approximately how long it took to return to baseline
- Weekly review — look for patterns: Is your baseline shifting lower? Is recovery time shortening? Are you noticing activation earlier?
This works because it builds interoceptive tracking — the foundation of self-regulation. For disorganized attachment: also note how many times you switched between activation and shutdown in a day. Over weeks, you may notice the switching slows. That's your nervous system stabilizing, one degree at a time. Two minutes a day is enough.
When Should You Seek Professional Help for Nervous System Dysregulation?
Self-guided practices are valuable, but complex attachment trauma often requires professional support for safe processing. This isn't a failure of effort — it reflects the reality that some nervous system patterns need careful titration that another trained human being provides.
You may recognize some of these patterns in yourself — and noticing them already reflects the awareness that makes change possible. Seek a trauma-informed therapist if you experience:
- Dissociative episodes — losing time, feeling detached from your body, or watching yourself from outside
- Chronic physical symptoms without medical explanation — research links ACE scores of 4 or higher to 6.29 times the odds of emotional abuse comorbidity and widespread somatization (Palomba et al., 2017)
- Inability to maintain relationships despite genuinely wanting connection
- Flashbacks, intrusive memories, or nightmares that self-regulation techniques don't reduce
- Substance use or compulsive behaviors to manage nervous system activation
- Feeling worse after attempting somatic or body-based practices on your own — this can indicate trauma material surfacing faster than your window of tolerance can hold
When looking for a therapist, ask specifically about training in Somatic Experiencing, EMDR, or IFS. A trauma-informed therapist understands titration — the practice of approaching traumatic material in small, carefully dosed increments rather than overwhelming the nervous system. General talk therapy without body-based training may inadvertently reinforce avoidant patterns (staying in the intellect) or anxious patterns (storytelling without regulation).
Can therapy change your attachment style? explores the broader evidence for therapeutic attachment change. For attachment-style-specific therapy guidance, see our guides for avoidant and disorganized attachment.
Frequently Asked Questions
Can a dysregulated nervous system be healed?
Yes. Neuroplasticity allows the nervous system to form new pathways throughout life. Therapies like EMDR, Somatic Experiencing, and trauma-sensitive yoga produce measurable changes in brain structure, stress hormones, and vagal tone — indicating genuine neural rewiring, not just symptom management.
How long does it take to heal your nervous system from trauma?
Research suggests initial stabilization within four to eight weeks, with significant symptom reduction in three to six months of consistent therapy. An IFS pilot study showed PTSD remission in 16 weeks, and a yoga trial showed 52 percent remission in 10 weeks. Full integration of new nervous system patterns typically takes one to two years.
What does a dysregulated nervous system feel like?
Common signs include chronic muscle tension, racing heartbeat, difficulty sleeping, emotional numbness, exaggerated startle response, digestive issues, and difficulty staying present during conversations. The specific pattern depends on your attachment style — anxious types tend toward hyperarousal while avoidant types tend toward shutdown.
How do you know if your nervous system is damaged from trauma?
Key indicators include disproportionate reactions to minor stressors, difficulty calming down after conflict, chronic physical symptoms without medical explanation, emotional numbness or dissociation, and hypervigilance in relationships. These reflect a nervous system stuck in defensive states, not permanent damage — they are reversible patterns.
Can you rewire your brain from attachment trauma?
Yes. Neuroimaging studies show that therapy can increase hippocampal volume, strengthen prefrontal-amygdala connectivity, and restore excitatory-inhibitory brain balance. Neurofeedback research shows a 79.3 percent PTSD remission rate by directly targeting these brain circuits. The brain retains capacity for structural change throughout adulthood.
What is the best therapy for nervous system dysregulation?
The most effective approaches combine body-based processing with relational safety. Somatic Experiencing (effect sizes d = 0.94–1.26), EMDR (g = 0.93), and trauma-sensitive yoga (52 percent PTSD remission) have the strongest evidence. The best choice depends on your attachment style and whether trauma is relational or single-incident.
How does trauma get stuck in the body?
Trauma encodes in the autonomic nervous system as incomplete defensive responses — fight, flight, or freeze reactions that never completed. Van der Kolk's research shows this creates persistent patterns of muscle tension, altered stress hormone production, and sensory-motor circuits that keep the body in survival mode even when danger has passed.
Does the nervous system ever fully recover from trauma?
Full recovery means developing a resilient nervous system with a wide window of tolerance rather than returning to a pre-trauma state. Research shows measurable improvements in heart rate variability, cortisol regulation, and brain structure with treatment. Many trauma survivors develop greater emotional awareness and relational capacity than they had before.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Neuroscience and Attachment Theory
- Feldman, R. (2017). The neurobiology of human attachments. Trends in Cognitive Sciences, 21(2), 80–99.
- Feldman Lab. (2021). Social dialogue triggers aligned and synchronized biobehavioral states. Nature Scientific Reports.
- Neurobiology of disorganized attachment: A review. (2023). Neuroscience Insights.
- Mikulincer, M., & Shaver, P. R. (2024). Attachment orientations and emotion regulation. PMC.
Polyvagal Theory and Nervous System
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. W. W. Norton.
- Polyvagal Theory: Current status, clinical applications, and future directions. PMC.
- Heart rate variability and cardiac vagal tone in psychophysiological research. (2017). Frontiers in Psychology.
Trauma and the Body
- Van der Kolk, B. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Viking.
- Siegel, D. J. (2012). Healing Trauma: Attachment, Mind, Body, and Brain. W. W. Norton.
- Siegel, D. J. The window of tolerance. (2022). Psychology Today.
- Schwartz, A. (2021). How relationships change the brain and heal attachment. DrArielle Schwartz.com.
Adverse Childhood Experiences and Epidemiology
- Palomba, A., et al. (2017). Clinical profile associated with adverse childhood experiences: The onset of a nervous system dysregulation. PMC.
- Impact of adverse childhood experiences on depression: The role of insecure attachment and emotion dysregulation. (2023). PMC.
- Attachment style statistics 2026. WifiTalents.
Treatment Efficacy
- Brom, D., et al. (2017). Somatic Experiencing for posttraumatic stress disorder: A randomized controlled outcome study. Journal of Traumatic Stress. (Scoping review via PMC.)
- EMDR meta-analysis for PTSD. Psicothema.
- Attachment-Based EMDR randomized controlled trial. (2025). ScienceDirect.
- Hodgdon, H. B., et al. (2021). Internal Family Systems (IFS) therapy for PTSD: A pilot effectiveness study. Journal of Aggression, Maltreatment & Trauma.
- Van der Kolk, B. A., et al. (2014). Yoga as an adjunctive treatment for PTSD: A randomized controlled trial. Journal of Clinical Psychiatry, 75(6), e559–e565.
- Neurofeedback for PTSD: A meta-analysis. (2023). PMC.
This article is for educational purposes only and is not a substitute for professional mental health care. If you are experiencing symptoms of trauma, please consult a licensed therapist or mental health professional. Crisis support is available through the 988 Suicide and Crisis Lifeline (call or text 988) and the Crisis Text Line (text HOME to 741741).
