Healing avoidant attachment typically requires 12 to 24 months of consistent therapeutic work, though small shifts can begin within weeks. Approximately 22 to 25 percent of adults have avoidant attachment (Mickelson et al., 1997). Research shows that transference-focused psychotherapy produced significant increases in secure attachment classification after 12 months of treatment (Levy et al., 2006), while avoidant clients showed the least symptom change of any attachment style by session 32 (Wiseman and Tishby, 2014).
If you're searching for a timeline, you're likely frustrated—maybe with yourself, with the pace of change, or with the nagging question of whether change is even possible. That frustration makes sense. The trait that needs healing—emotional avoidance—is the same trait that slows the healing process. This article provides honest, research-grounded benchmarks rather than vague reassurance, so you know what to realistically expect. If you're still identifying whether this pattern fits you, start with How Do I Know If I Have Avoidant Attachment?.
Key takeaway: Healing avoidant attachment typically takes 12 to 24 months of consistent therapeutic work, with avoidant individuals progressing more slowly than anxious ones. Only 25 percent of life events produce enduring attachment changes. Daily practices like security priming can accelerate progress, but meaningful shifts require patience and repetition rather than a single breakthrough.
What Does Research Say About Avoidant Attachment Healing Timelines?
Research provides three key benchmarks for avoidant attachment healing, and none of them offer a quick fix. 12 months of therapy is the earliest point where measurable shifts from insecure to secure attachment have been documented, and avoidant individuals consistently show the slowest initial progress of any attachment style.
In a randomized controlled trial of 90 patients, Levy et al. (2006) found that transference-focused psychotherapy was the only treatment arm—compared to DBT and supportive psychotherapy—to produce significant increases in secure attachment classification on the Adult Attachment Interview after 12 months. This remains one of the strongest data points for how long measurable attachment change takes in a clinical setting.
Avoidant clients face a steeper climb than their anxious counterparts. Wiseman and Tishby (2014) studied 67 clients in psychodynamic psychotherapy and found that clients high in attachment avoidance showed the least symptom change from intake to session 32—approximately eight months of treatment—regardless of therapist attachment style. Progress happens, but it happens slowly.
Perhaps the most sobering finding comes from a multiwave longitudinal study of over 4,000 participants tracked for 6 to 40 months. Fraley et al. (2021) found that while half of significant life events produced immediate attachment changes, only 25 percent led to enduring shifts. Most people reverted to their baseline attachment style. The life events that did produce lasting change shared one feature: the person perceived them positively.
Knowing these benchmarks lets you measure real progress rather than comparing yourself to an unrealistic timeline. For a broader look at attachment change timelines across all styles, see How Long Does It Take to Change Your Attachment Style?.
Your Avoidant Healing Timeline (self-assessment for dismissive-avoidant attachment)
- Rate your current awareness of deactivating strategies on a scale of 1 to 10
- Note how many close relationships currently include emotional vulnerability from you
- Identify one moment this week where you noticed an impulse to withdraw—did you catch it in the moment or only after?
- Write these down and revisit them every 3 months to track your trajectory
This works for dismissive-avoidant attachment because it creates concrete, measurable markers rather than abstract "feeling better." Avoidant individuals tend to intellectualize progress—this exercise grounds healing in observable data points that bypass the tendency to dismiss emotional shifts as insignificant.
Why Does Avoidant Attachment Take Longer to Heal Than Anxious Attachment?
Avoidant attachment heals more slowly than anxious attachment because of three neurobiological factors that make the nervous system resistant to the very interventions designed to help. Your body learned to survive by shutting down emotional signals, and that adaptation now works against the healing process itself.
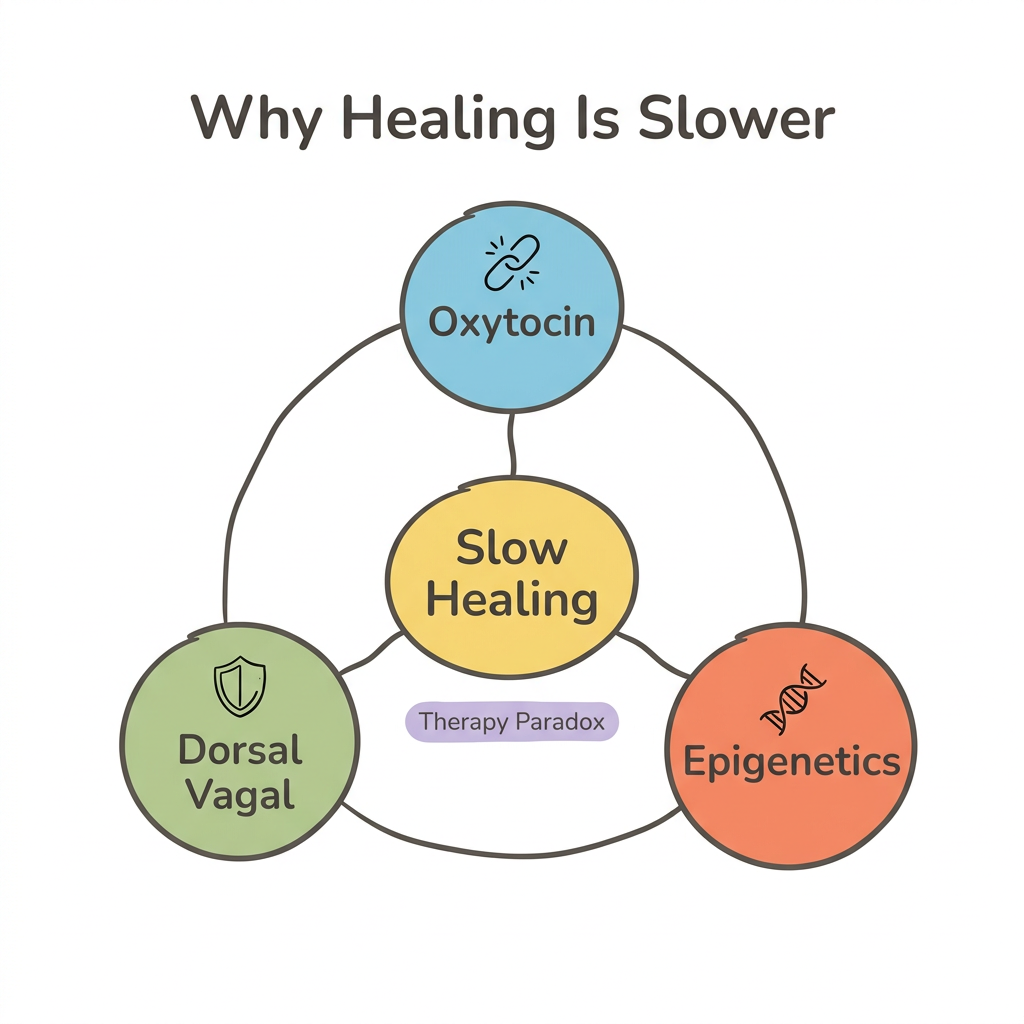
1. Reduced oxytocin responsiveness. Research on oxytocin administration found that only low-avoidance individuals showed increased social affiliation after receiving oxytocin. High-avoidance individuals instead showed faster detection of disgust faces—their nervous systems literally interpreted a bonding neurochemical as a threat signal. This means avoidant individuals don't get the same neurochemical reward from social connection that makes bonding interventions effective for anxious individuals.
2. Through the lens of polyvagal theory, dorsal vagal dominance maps avoidant attachment to chronic shutdown and numbing—the nervous system's freeze response. Where anxious attachment produces hyperactivation (racing heart, urgent reaching for contact), avoidant attachment produces hypoactivation: flatness, emotional numbness, and a sense of not needing anyone. Rewiring from shutdown to engagement requires passing through sympathetic activation first—which feels like anxiety. You can learn more about this pathway in Can You Heal Your Nervous System from Attachment Trauma?.
3. Epigenetic cortisol changes compound the challenge further. Research on 109 individuals found increased methylation of the glucocorticoid receptor gene (NR3C1) in avoidant attachment—resulting in less efficient HPA axis negative feedback and altered stress regulation. The encouraging finding: epigenetic changes are potentially reversible through therapeutic intervention.
There is also what researchers call the "therapy paradox." Avoidant individuals are the least likely to seek therapy because their core defense is self-sufficiency. When they do enter treatment, Wiseman and Tishby's (2014) data shows they progress most slowly in early sessions. Early therapy often feels pointless—not because it isn't working, but because the avoidant pattern is showing up in the therapy room itself.
A meta-analysis of security priming studies (Gillath and Karantzas, 2022) confirmed this disparity: across 120 studies and 18,949 participants, security priming produced an overall effect size of d=.51, but avoidant individuals showed weaker responses than anxious individuals.
Noticing Shutdown (somatic body scan for avoidant attachment)
- Set a timer for 2 minutes
- Place one hand on your chest, one on your stomach
- Notice areas of numbness, tension, or "nothing"—these are dorsal vagal signals
- Without trying to change anything, name what you notice: "My chest feels flat," "My jaw is tight," "I feel nothing below my neck"
- Practice daily for one week, noting any shifts in what you feel
This builds interoceptive awareness—the foundation for reconnecting with emotional needs. Avoidant attachment develops when caregivers discourage emotional expression, training the nervous system to suppress body-based signals. By simply noticing what your body is doing, you begin reversing that suppression without forcing anything.
What Are the Stages of Healing Avoidant Attachment?
Healing avoidant attachment follows four overlapping stages that typically unfold over 12 to 24 months with therapeutic support. These stages are not perfectly linear—you will move between them, and progress in one area often precedes regression in another before stabilizing.
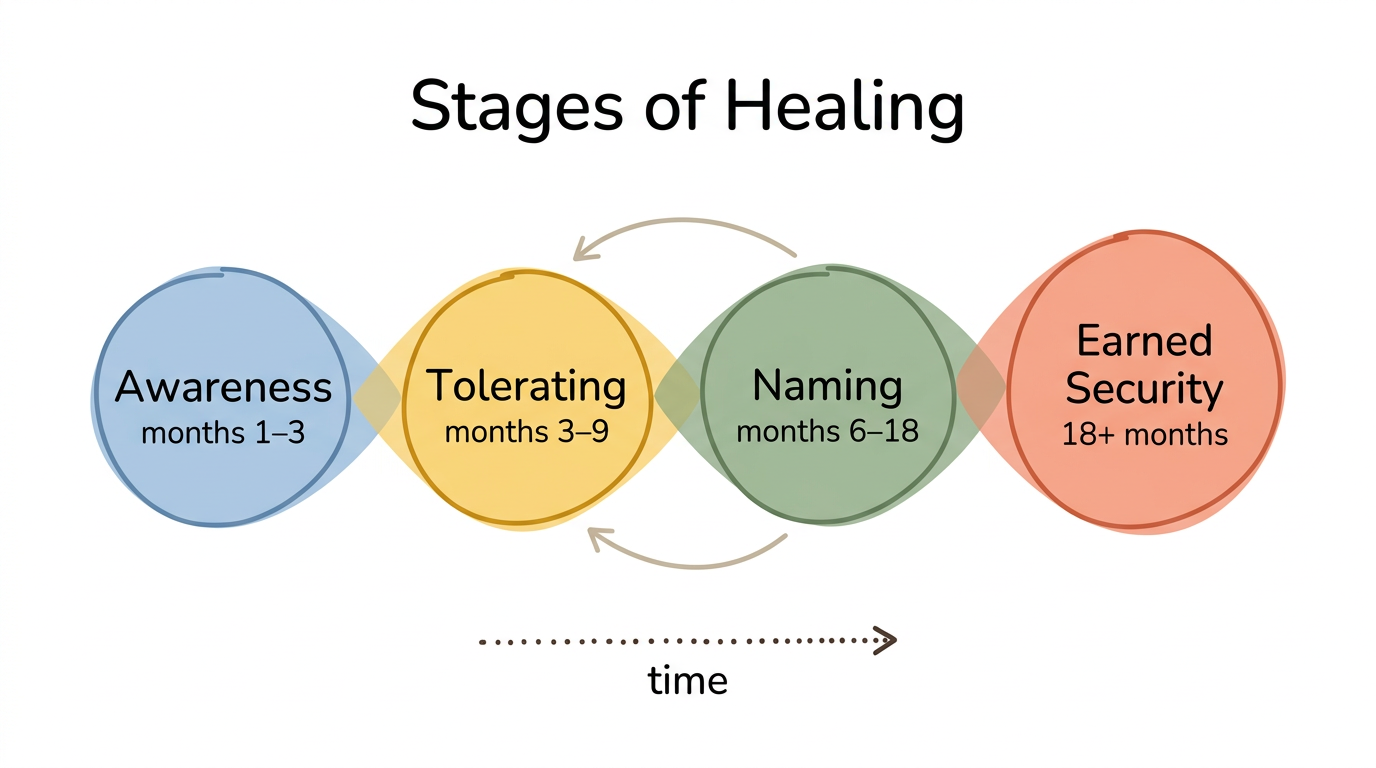
Stage 1: Awareness of deactivating strategies (months 1 to 3). You start recognizing the patterns: pulling away when someone gets close, focusing on a partner's flaws to justify distance, idealizing past relationships, intellectualizing emotions instead of feeling them. At this stage, awareness usually arrives after the fact—you realize you withdrew hours or days later. Recognition alone is significant. Most people with avoidant attachment have spent years experiencing these patterns as simply "who I am" rather than learned protective responses.
Stage 2: Tolerating proximity distress (months 3 to 9). Your nervous system begins registering closeness as uncomfortable rather than invisible. Where you once felt nothing when someone reached for emotional connection, you now feel something—agitation, restlessness, the urge to check your phone, a sudden need to be alone. This discomfort is actually progress. It means your nervous system is moving from dorsal vagal shutdown into sympathetic activation. The work here is staying present with that discomfort 10 percent longer each time.
Stage 3: Naming emotional needs (months 6 to 18). Saying "I missed you" or "I need reassurance" out loud to another person represents a profound shift for someone whose nervous system learned that emotional needs drive people away. This stage often overlaps with Stage 2 and requires earned secure attachment—developing new relational experiences that gradually overwrite the old template.
Stage 4: Earned security becoming automatic (18+ months). Reaching for connection begins to feel less effortful. You still notice avoidant impulses under stress—earned security does not erase the original pattern—but your default response shifts. Muller (2016) documented a case of avoidant personality disorder achieving full remission through long-term psychodynamic therapy, though AvPD has only a 31 percent remission rate after 24 months, underscoring how extended this timeline can be for severe presentations.
Which Stage Am I In? (reflective journaling for avoidant attachment)
- Read each stage description above
- Identify which stage resonates most with your current experience
- Write one specific example from the past week that illustrates your current stage
- Note one behavior from the next stage you'd like to practice—just one
Avoidant individuals often need intellectual structure before emotional engagement. Stages provide a cognitive framework that makes the ambiguous process of healing feel more navigable—and this exercise channels the avoidant strength of analysis toward self-understanding rather than self-avoidance.
Which Therapies Produce the Fastest Results for Avoidant Attachment?
Emotionally Focused Therapy (EFT) and Transference-Focused Psychotherapy (TFP) have the strongest evidence for shifting avoidant attachment, though the "best" therapy depends on whether you're working individually or with a partner. For a comprehensive comparison, see What Therapy Is Best for Avoidant Attachment?.
| Therapy Type | Typical Duration | Evidence Level | Best For | Key Finding |
|---|---|---|---|---|
| EFT | 8–20 sessions | RCTs and meta-analysis | Couples | 77 percent of couples recovered in 10–12 sessions; avoidance reduction was the strongest predictor of relationship satisfaction (Johnson et al., 1999) |
| TFP | 12+ months | RCT (Levy et al., 2006) | Individual (personality-level change) | Only treatment to shift AAI classification from insecure to secure in a controlled trial |
| CBT + Emotional Processing | 16–20 sessions | RCT (Newman et al., 2016) | Individual (cognitive) | Enhanced outcomes specifically for dismissive clients compared to CBT plus supportive listening alone |
| Security Priming | 3+ weeks daily | Meta-analysis (120 studies) | Daily self-practice | d=.51 overall effect; d=.62 for affect domain—though weaker for avoidant individuals |
| Somatic/Polyvagal | 6–18+ months | Emerging | Body-based processing | Expands window of tolerance from dorsal vagal shutdown toward ventral vagal engagement |
EFT stands out for couples work because decreases in attachment avoidance were the strongest predictor of lasting relationship satisfaction at follow-up (Johnson et al., 1999). For individual therapy, TFP produced the only measurable attachment reclassification in a randomized controlled trial—though it requires a 12-month commitment. Newman et al. (2016) found that adding interpersonal emotional processing to CBT specifically enhanced outcomes for dismissive and avoidant clients, suggesting that standard CBT alone may not reach the relational core of avoidant patterns. You can also explore whether therapy can change your attachment style more broadly.
Values Beneath the Wall (ACT-informed exercise for dismissive-avoidant attachment)
- List 3 moments you pulled away from someone in the past month
- For each, ask: "What was I protecting?"
- Then ask: "What did I actually want in that moment?"
- Notice the gap between the protective behavior and the underlying value—connection, safety, being truly known
- Choose one small action this week aligned with the underlying value rather than the protective impulse
This works for dismissive-avoidant attachment because it bypasses the defense of "I don't need anyone." ACT's values framework reveals what matters beneath the withdrawal—not by challenging the wall directly, but by looking at what the wall was built to protect.
Can You Speed Up Avoidant Attachment Healing?
You can accelerate avoidant attachment healing through evidence-based daily practices, though "faster" still means months of consistent effort rather than days. Security priming has the strongest evidence for producing measurable shifts outside of therapy sessions.
Gillath et al. (2008) demonstrated that repeated security priming over three weeks produced persisting increases in self-esteem, positive mood, and compassion compared to controls. A subsequent meta-analysis by Gillath and Karantzas (2022) confirmed these effects across 120 studies with 18,949 participants, finding an overall effect size of d=.51 and d=.62 for the affect domain—the largest effect. Security priming also reduces amygdala activation in response to social and linguistic threat, demonstrating that neural patterns can shift even with brief interventions.
However, avoidant individuals show a weaker response to security priming than anxious individuals (Gillath and Karantzas, 2022). Your nervous system has spent years dampening exactly the signals that priming tries to activate. This does not mean priming doesn't work for you—it means the effects accumulate more gradually and consistency matters even more.
Three evidence-informed accelerators work alongside therapy:
- Daily security priming (5 minutes)—visualizing a safe attachment figure activates the neural networks associated with secure bonding, even when your conscious mind dismisses it
- Start with small, tolerable shifts rather than pushing for emotional breakthroughs. Somatic window expansion through polyvagal-informed practices gradually moves you from dorsal vagal shutdown toward ventral vagal engagement
- Micro-moments of vulnerability—sharing one honest feeling per day with someone you trust, even something small like "that bothered me" or "I liked spending time with you"
You don't rewire avoidant attachment in a single insight. You rewire it by noticing 10 percent earlier, responding 10 percent differently, 10 percent more often.
5-Minute Security Priming Practice (for avoidant attachment)
- Choose a person—real or imagined—who represents unconditional acceptance
- Close your eyes and visualize their face for 30 seconds
- Recall a specific moment they showed you care—focus on sensory details (their voice, a gesture, the setting)
- Notice any body sensations: warmth, softening, tightness, or nothing at all. All responses are valid data
- Repeat daily for 3 weeks—the duration shown to produce lasting effects in research (Gillath et al., 2008)
If you're skeptical, that skepticism is the avoidant pattern doing its job. This exercise is grounded in a meta-analysis of 120 studies with 18,949 participants—not wishful thinking. Your nervous system responds to repeated safe relational imagery whether your conscious mind "believes in it" or not.
How Do You Know If Avoidant Attachment Healing Is Working?
The earliest sign of avoidant healing is catching deactivating strategies in real-time rather than after the fact. You notice the impulse to scroll your phone when your partner is being vulnerable, the mental cataloging of their flaws when things get close, the sudden "need" for space that arrives right after intimacy.
Discomfort replacing numbness is progress. This is counterintuitive but essential. When closeness begins to feel uncomfortable rather than invisible, your nervous system is shifting from dorsal vagal shutdown to sympathetic activation. That agitation, restlessness, or urge to flee is your body waking up—not evidence that something is wrong. Understanding how attachment affects your nervous system can help you recognize these shifts as they happen.
Here are concrete markers organized by healing stage:
Early signs (months 1 to 6):
- You recognize withdrawal patterns the same day they happen instead of days later
- Closeness produces visible discomfort rather than numbness
- You can articulate what you're avoiding, even if you can't stop avoiding it yet
Mid-stage signs (months 6 to 12):
- Naming emotional needs to a trusted person becomes possible, even if it feels mechanical
- You tolerate relational disappointment without disappearing entirely
- Longing for connection surfaces without being immediately suppressed
Later, around the 12-month mark and beyond, the shifts become more structural. Reaching for connection feels less effortful, though not yet automatic. You can sit with someone else's emotions without shutting down or fixing. Tolerating relational disappointment without withdrawal becomes your more frequent response, even if the old pattern still surfaces under high stress.
If you're curious about the broader trajectory, Can Avoidant Attachment Be Healed? covers the evidence for long-term change.
Progress Signals Check-In (body-based tracking for avoidant attachment)
- At the end of each week, rate on a 1 to 10 scale: "How much emotional sensation did I allow this week?"
- Note one moment you felt the urge to withdraw—did you notice it sooner than you would have three months ago?
- Track one body-based shift: Can you feel your heartbeat when you check in? Does your chest soften when someone is kind to you? Do you notice your stomach when you're upset?
- Record answers monthly to see your trajectory over time
This redirects attention to internal shifts that precede behavioral change. Avoidant individuals often measure healing only by relationship outcomes—"Am I in a good relationship yet?"—but the polyvagal progression from shutdown to activation to engagement happens inside your body first. Tracking somatic signals gives you evidence of change your mind might otherwise dismiss.
When Should You Seek Professional Help for Avoidant Attachment?
You should consider professional help when your awareness of avoidant patterns outpaces your ability to change them on your own—when you can see the wall going up but can't stop building it. Your self-sufficiency has served you. It kept you functioning when emotional needs felt dangerous. And right now, it may be the thing standing between you and the connection you actually want.
The therapy paradox is real: avoidant individuals are the least likely attachment style to seek help because self-sufficiency functions as a defense. Recognizing that pattern in yourself is already significant. Here are signs that professional support would accelerate your healing:
- Relationships consistently end the same way—you withdraw, they pursue, the cycle exhausts both of you. Understanding how avoidant attachment affects relationships can clarify whether this pattern applies
- You're aware of your deactivating strategies but unable to interrupt them in the moment
- Emotional numbness affects your quality of life—not just relationships, but your capacity to feel pleasure, grief, or excitement
- Physical symptoms linked to chronic emotional suppression appear: persistent jaw tension, digestive issues, or a sense of living "neck up"
- You've read extensively about attachment theory but knowledge alone hasn't shifted the pattern
Expect that early sessions may feel pointless. Wiseman and Tishby (2014) confirmed that avoidant clients show the least progress in the first eight months. This is the avoidant pattern showing up in the therapy room—not evidence that therapy doesn't work. A therapist experienced in attachment can work with that resistance rather than against it.
The Cost-of-Avoidance Inventory (for dismissive-avoidant individuals considering therapy)
- List 3 relationships that ended or suffered because of emotional withdrawal
- For each, name the emotional cost honestly: regret, loneliness, lost connection, the person you didn't let yourself be
- Compare that accumulated cost to the discomfort of committing to 12 months of weekly therapy
- This is not about guilt—it's about honest accounting of what avoidance costs you versus what vulnerability might return
Dismissive-avoidant individuals respond to logical cost-benefit analysis more readily than emotional appeals. This exercise channels your analytical strength—the same one that keeps you safe—toward a clear-eyed evaluation of whether the current strategy is still working.
Frequently Asked Questions
Can avoidant attachment be fully healed?
Avoidant attachment can shift toward earned security, though "fully healed" is misleading. Research shows measurable attachment reclassification after 12 months of therapy (Levy et al., 2006). Most people develop a secure-dominant style while retaining some avoidant tendencies under stress—and that is a meaningful, research-supported outcome.
Can you heal avoidant attachment without therapy?
Self-directed healing is possible but typically slower. Security priming produced a d=.51 effect across 120 studies (Gillath and Karantzas, 2022). However, avoidant individuals show weaker responses to self-administered interventions than anxious individuals. Therapy accelerates progress by providing a corrective relational experience that self-practice cannot replicate.
What are the stages of healing avoidant attachment?
Four stages unfold over 12 to 24 months: recognizing deactivating strategies, tolerating proximity discomfort without withdrawing, naming emotional needs to another person, and earned security becoming automatic. These stages overlap—regression during stressful periods is normal and expected.
How do you know if an avoidant is healing?
Early signs include catching withdrawal impulses in real-time rather than days later, and feeling discomfort with closeness instead of numbness. A key polyvagal marker worth understanding: moving from emotional shutdown to feeling agitated by closeness—activation replacing numbness—is actually progress, even though it feels worse.
Why is avoidant attachment so hard to change?
Three neurobiological factors slow avoidant healing: reduced oxytocin responsiveness limits bonding rewards, dorsal vagal dominance defaults the nervous system to shutdown rather than connection-seeking, and epigenetic cortisol changes alter stress regulation. The core defense—self-sufficiency—also makes avoidant individuals least likely to seek the help that would accelerate change.
Can an avoidant person fall in love?
Yes. Avoidant individuals experience love but suppress its expression through deactivating strategies—idealizing ex-partners, focusing on a current partner's flaws, or creating emotional distance when intimacy deepens. Healing involves learning to tolerate love's vulnerability rather than developing the capacity to love, which already exists beneath the protective patterns.
How long does it take for an avoidant to come back after pulling away?
Without healing work, the pull-away and return cycle repeats every few days to weeks, driven by the oscillation between needing space and needing connection. With therapeutic support, the withdrawal duration typically shortens as the person learns to recognize deactivating strategies and tolerate closeness discomfort sooner rather than needing complete retreat.
Is dismissive avoidant harder to heal than fearful avoidant?
They present different challenges rather than a clear hierarchy of difficulty. Dismissive avoidant individuals often resist therapy longer due to stronger self-sufficiency defenses, but once engaged, their healing path is more straightforward. Fearful-avoidant individuals may seek help sooner but face the additional complexity of oscillating between approach and avoidance.
Want to Go Deeper?
Meadow includes a structured assessment to help you understand your specific attachment patterns, followed by a 66-day program of daily practices designed to build earned security.
Start your free week →References
Attachment Change and Therapy Outcomes
Levy, K. N., Meehan, K. B., Kelly, K. M., Reynoso, J. S., Weber, M., Clarkin, J. F., & Kernberg, O. F. (2006). Change in attachment patterns and reflective function in a randomized control trial of transference-focused psychotherapy for borderline personality disorder. Journal of Consulting and Clinical Psychology, 74(6), 1027–1040.
Wiseman, H., & Tishby, O. (2014). Client attachment, attachment to the therapist and client-therapist attachment match: How do they relate to change in psychodynamic psychotherapy? Psychotherapy Research, 24(3), 392–406.
Fraley, R. C., Gillath, O., & Deboeck, P. R. (2021). Do life events lead to enduring changes in adult attachment styles? A naturalistic longitudinal investigation. Journal of Personality and Social Psychology, 120(6), 1567–1606.
Muller, R. T. (2016). Earned secure attachment in psychotherapy: From avoidant personality disorder to earned security. American Journal of Psychotherapy, 70(3), 233–263.
Security Priming
Gillath, O., Selcuk, E., & Shaver, P. R. (2008). Moving toward a secure attachment style: Can repeated security priming help? Social and Personality Psychology Compass, 2(4), 1651–1666.
Gillath, O., & Karantzas, G. (2022). Attachment security priming: A meta-analysis. Personality and Social Psychology Review, 26(3), 183–206.
Norman, L., Lawrence, N., Iles, A., Benattayallah, A., & Karl, A. (2015). Attachment-security priming attenuates amygdala activation to social and linguistic threat. Social Cognitive and Affective Neuroscience, 10(6), 832–839.
Therapy Modalities
Johnson, S. M., Hunsley, J., Greenberg, L., & Schindler, D. (1999). Emotionally focused couples therapy: Status and challenges. Clinical Psychology: Science and Practice, 6(1), 67–79.
Newman, M. G., Castonguay, L. G., Jacobson, N. C., & Moore, G. A. (2016). Adult attachment as a moderator of treatment outcome for generalized anxiety disorder: Comparison between cognitive-behavioral therapy (CBT) plus interpersonal and emotional processing therapy (I/EP) and CBT plus supportive listening. Journal of Consulting and Clinical Psychology, 83(5), 915–925.
Neuroscience and Biology
Feldman, R. (2017). The neurobiology of human attachments. Trends in Cognitive Sciences, 21(2), 80–99.
Ein-Dor, T., Verbeke, W., Mokry, M., & Vrtička, P. (2022). Epigenetic modification of the oxytocin and glucocorticoid receptor genes is linked to attachment avoidance in young adults. Neuroscience Insights, 17.
Alvares, G. A., Hickie, I. B., & Guastella, A. J. (2010). Acute effects of intranasal oxytocin on subjective and behavioral responses to social rejection. Experimental and Clinical Psychopharmacology, 18(4), 316–321.
Prevalence
Mickelson, K. D., Kessler, R. C., & Shaver, P. R. (1997). Adult attachment in a nationally representative sample. Journal of Personality and Social Psychology, 73(5), 1092–1106.
This article is for educational purposes only and is not a substitute for professional mental health treatment. If avoidant attachment patterns are significantly affecting your relationships or quality of life, please consult a licensed therapist experienced in attachment-based approaches.
